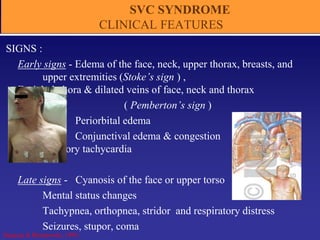
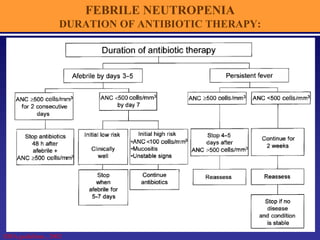
The document provides an overview of oncologic emergencies, including superior vena cava syndrome, febrile neutropenia, hypercalcemia of malignancy, spinal cord compression, brain metastasis, and hyperleukocytosis. It details symptoms, evaluation methods, management strategies, and specific treatments for each condition, emphasizing the importance of appropriate interventions and monitoring. Pain management in cancer patients is also discussed, highlighting radiation therapy as an effective option for alleviating pain.