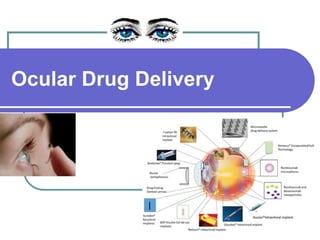
Ocular DDS.pptx
- 2. Ophthalmic Vs Ocular ❑ They are specialized & Conventional dosage forms designed to be instilled onto the external surface of the eye (topical), administered inside (intraocular) or adjacent (periocular) to the eye or used in conjunction with an ophthalmic device. ● The most commonly employed ophthalmic dosage forms are solutions, suspensions, and ointments. ● These preparations when instilled into the eye are rapidly drained away from the ocular cavity due to tear flow and lacrimal nasal drainage. ❖ The newest dosage forms for ophthalmic drug delivery are called as OCULAR DDS: gels, gel- forming solutions, ocular inserts , intravitreal injections and implants.
- 3. Drugs used in the eye: ● Miotics (Contraction of pupil) e.g. pilocarpine Hcl ● Mydriatics (Dilation of pupil) e.g. atropine ● Cycloplegics (paralyzes the ciliary body) e.g. atropine ● Anti-inflammatories e.g. corticosteroids ● Anti-infectives (antibiotics, antivirals and antibacterials) ● Anti-glucoma drugs (reduce the intra-ocular pressure) e.g. pilocarpine Hcl ● Surgical adjuncts e.g. irrigating solutions ● Diagnostic drugs e.g. sodiumfluorescein ● Anesthetics e.g. tetracaine
- 4. Need of ocular drug delivery ● These Novel devices and/or formulations may help to surpass ocular barrier and associated side effects with conventional topical drops. ● It provides prolong drug retention thus better absorption and consequently improved bioavailability. ● Helps to avoid pre-corneal elimination. ● Patient compliance is facilitated.
- 5. Anatomy and Physiology of the Eye:
- 9. Anterior portion – Cornea, Conjunctiva, Aqueous humor, Iris, Ciliary body, Lens Posterior Portion – Sclera, Choroid, Retina, Vitreous body Cornea Devoid of blood vessels Derives nourishment form tear fluid and aqueous humor 12mm in diameter, 520µm in thickness
- 12. ● limited volume of administration (30 μL); ● fast clearance from ocular surface; ● Metabolism of the active by tear enzymes; ● nonproductive uptake into systemic circulation via highly vascularized conjunctiva, choroid, uveal tract and inner retina ● anterior membrane barriers (cornea, conjunctiva, and sclera); ● aqueous humor outflow; ● long diffusional path ; and ● acellular nature of the vitreous, which may negatively impact the pharmacokinetics and distribution of topically applied drugs. Barriers: Ocular DDS
- 14. Pathway for ocular absorption:
- 17. Ocular drug delivery routes
- 18. Barriers for Ocular Drug Absorption Depending on the route of administration: 1. Topical Precorneal factors Solution drainage, Blinking, Tear dilution, Tear turnover, Induced lacrimation, Conjuctival absorption 2. Physical barriers Cornea Sclera Conjuctiva 3. Oral 4. Periocular and intravitreal 5. Parentetal Blood aqueous barrier Blood retinal barrier
- 19. Barriers for Ocular Drug Absorption – Topical Route Mostly in the form of eye drops Employed to treat anterior segment diseases Site of action is usually different layers of the cornea, conjunctiva, sclera, iris and ciliary body. Precorneal factors: • Solution drainage, blinking, tear film, tear turn over, and induced lacrimation • Human tear volume is estimated to be 7 μl • Mucin present in the tear film plays a protective role by forming a hydrophilic layer that moves over the glycocalyx of the ocular surface and clears debris and pathogens • Contact time with the absorptive membranes is lower • Less than 5% of the applied dose reaches the intraocular tissues
- 21. Mechanical barriers for topical drug absorption Cornea Limits the entry of exogenous substances into the eye and protects the ocular tissues Divided into the epithelium, stroma, and endothelium The corneal epithelium is lipoidal in nature Offers resistance for permeation of topically administered hydrophilic drugs Corneal epithelium… Corneal epithelial cells are joined to one another by desmosomes Tight junctional complexes retards paracellular drug permeation from the tear film into intercellular spaces of the epithelium as well as inner layers of the cornea Layers of the Cornea Stroma Comprises 90% of the corneal thickness Highly hydrated structure Barrier to permeation of lipophilic drug molecules Endothelium Endothelial junctions are leaky - facilitate the passage of macromolecules between the aqueous humor and stroma Drugs should have an amphipathic nature in order to permeate through these layers
- 22. Sclera Consists of collagen fibers and proteoglycans embedded in an extracellular matrix Permeability - comparable to that of the corneal stroma Positively charged molecules exhibit poor permeability presumably due to their binding to the negatively charged proteoglycan matrix Permeability of drug molecules across the sclera is inversely proportional to the molecular radius
- 24. Barriers for Ocular Drug Absorption – Parenteral Route Anterior segment: blood–aqueous barrier Posterior segment: blood–retinal barrier
- 25. Blood–aqueous barrier Tight junctional complexes and prevent the entry of solutes into the intraocular environment such as the aqueous humor Blood–retinal barrier Restricts the entry of the therapeutic agents from blood into the posterior segment. Regulates drug permeation from blood to the retina
- 26. Barriers for Ocular Drug Absorption
- 36. ● “Smart” hydrogels, or stimuli-sensitive hydrogels, are very different from inert hydrogels in that they can “sense” changes in environmental properties such as pH and temperature and respond by increasing or decreasing their degree of swelling. ● The stimuli that induce various responses of the hydrogels systems include physical (temperature) or chemical (pH, ions) ones. ● There are many mechanisms have been employed to cause reversible sol-gel phase transition by different stimuli. STIMULI-SENSITIVE HYDROGELS
- 37. STIMULI-SENSITIVE HYDROGELS ● physiological environmental conditions of human body: The stimuli that induce various responses of the hydrogel ● systems include- ● 1. Physical stimuli like: Change in temperature, electric fields, light, pressure, sound, and magnetic fields. ● 2. Chemical stimuli like: Change in pH and ion activation from biological fluid. ● 3. Biological/biochemical (bimolecular) stimuli like: Change in glucose level ● In ophthalmic drug delivery three types of stimuli-sensitive hydrogels - temperature sensitive, pH sensitive, and ● ion-sensitive hydrogels are mainly used.
- 39. Temperature-sensitive hydrogels ● Temperature-sensitive hydrogels are able to swell or de-swell as a result of changing in the temperature of the surrounding fluid. For convenience, temperature-sensitive hydrogels are classified into negatively thermosensitive, positively thermosensitive, and thermally reversible gels. ● Negative temperature-sensitive hydrogels have a lower critical solution temperature (LCST) and contract upon heating above the LCST. Copolymers of (Nisopropylacrylamide) (PNIAAm) are usually used for negative temperature release. Hydrogels show an on off drug release with on at a low temperature and off at high temperature allowing pulsatile drug release. LCST systems are mainly relevant for controlled release of drugs, and of proteins in particular. Thermosensitive polymers may be fixed on liposome membranes; in that case liposomes exhibit control of their content release.
- 40. ● Positive temperature-sensitive hydrogel has an upper critical solution temperature (UCST), such hydrogel contracts upon cooling below the UCST. Polymer networks of poly (acrylic acid) (PAA) and polyacrylamide (PAAm) or poly (acrylamide-co-butyl methacrylate) have positive temperature dependence of swelling. Temperature-sensitive hydrogels
- 41. ● The most commonly used thermoreversible gels are these prepared from poly (ethylene oxide)-b-poly (propylene oxide)-b-poly (ethylene oxide) (Pluronics , Tetronics , poloxamer). ● Polymer solution is a free-flowing liquid at ambient temperature and gels at body temperature, such a system would be easy to administer into desired body cavity. Depending on the ratio and the distribution along the chain of the hydrophobic and hydrophilic subunits, several molecular weights are available, leading to different gelation properties Pluronic F127, which gives colorless and transparent gels, is the most commonly used in pharmaceutical technology. ● At concentrations of 20% w/v and higher aqueous solutions of Poloxamer- 407 remain as a liquid at low temperatures [<15°C] and yield a highly viscous semisolid gel upon instillation into the cul-de-sac. At low temperatures, the Poloxamer forms micellar subunits in solution, and swelling gives rise to large micellar subunits and the creation of cross-linked networks. The result of this phenomenon is a sharp increase in viscosity upon heating. Temperature-sensitive hydrogels
- 42. ● Three principal mechanisms have been proposed to explain the liquid-gel phase transition after an increase in temperature, including: ● 1. Gradual desolvation of the polymer, ● 2. Increased micellar aggregation, and ● 3. The increased entanglement of the polymeric network. ● Despite all the promising results obtained with thermo reversible gels, there remains an important drawback associated with their use; the risk of gelation before administration by increase in ambient temperature during packing or storage. Temperature-sensitive hydrogels
- 43. pH-sensitive hydrogels ● These hydrogels respond to changes in pH of the external environment. These gels have ionic groups (which are readily ionizable side groups) attached to impart peculiar characteristics. Some of the pH sensitive polymers used in hydrogels’ preparations are ● polymethyl methacrylate (PMMA), ● polyacrylamide (PAAm), ● polyacrylic acid (PAA), ● poly dimethylaminoethylmethacrylate (PDEAEMA) ● polyethylene glycol.
- 44. ● These polymers though in nature are hydrophobic but swells in water depending upon the pH prevalent in the external environment. Any change in pH of the biological environment causes changes in the swelling behavior, ● for example, the hydrogel of caffeine is prepared with polymer PDEAEMA at pH below 6.6. As the polymer shows high swellability but when pH changes to higher side, the polymer showed shrinkage leading to drug release. ● The other pH-sensitive hydrogels are copolymer of PMMA and polyhydroxyethyl methyl acrylate (PHEMA), which are anionic copolymers, swell high in neutral or high pH but do not swell in acidic medium. It was also observed that pH and ionic strength determines kinetics of swelling of PHEMA and guar gum. pH-sensitive hydrogels
- 45. ● Cellulose acetate phthalate (CAP) latex, cross linked acrylic, and derivatives such as carbomer are used. Cellulose acetate derivatives are the only polymer known to have a buffer capacity that is low enough to gel effectively in the cul-de-sac of the eye. The pH change of about 2.8 units after instillation of the native formulation (pH 4.4) into the tear film leads to an almost instantaneous transformation of the highly fluid latex into viscous gel. ● But the low pH of the preparation can elicit discomfort in some patients. The poly acrylic acid and its lightly cross- linked commercial forms (Polycarbophil and Carbopol) exhibit the strongest muco-adhesion. pH-sensitive hydrogels
- 46. ● Ion-sensitive polymers belong to the mainly used in situ gelling materials for ocular drug delivery. Gelling of the instilled solution is also triggered by change in ionic strength. It is assumed that the rate at which electrolytes from the tear fluid is absorbed by the polymer will depend on the osmotic gradient across the surface of the gel. ● It is therefore likely that the osmolality of the solution might have an influence on the rate of the sol-gel transition occurring in the eye. One example is Gelrite, an anionic extra cellular polysaccharide, low acetyl Gellan gum secreted by pseudomonas elodea. Gelrite formulations in aqueous solutions form a clear gel in the presence of the mono or divalent cations typically found in the tear fluids. Ion-sensitive hydrogels
- 47. Ion-sensitive hydrogels ● The electrolyte of the tear fluid and especially Na+, Ca++, and Mg++ cations are particularly suited to initiate gelation of the polymer when instilled as a liquid solution in to the cul-de-sac. Gelrite has been the most widely studied and seems to be preferred compared to the pH sensitive or temperature setting systems. The polymeric concentration is much lower compared to previously described systems. ● Slightly viscous gellan gum solutions in low concentrations (<1%) show markedly increase in apparent viscosity, when introduced into presence of a physiological level of cations, without requiring more ions than 10–25% of those in tear fluid.The precorneal contact times for drugs can thus be extended up to 20-h. Gellan-containing formulations of pilocarpine HCl allowed reduction of drug concentration from 2% to 0.5% obtaining the same bioavailability.
- 51. Ocular Insert Non erodible inserts The Ocusert therapeutic system is a flat, flexible, elliptical device designed to be placed in the inferior cul-de-sac between the sclera and the eyelid and to release Pilocarpine continuously at a steady rate for 7 days Ocusert:
- 52. The device consists of 3 layers….. ● Outer layer – ethylene vinyl acetate copolymer layer. ● Inner Core – Pilocarpine gelled with alginate main polymer. ● A retaining ring - of EVA impregnated with titanium dioxide
- 53. The ocuserts available in two forms. ● Pilo – 20 (20 microgram / hour) ● Pilo – 40 (40 microgram / hour) Use: Chronic glaucoma Advantages ● Increase in ocular residence. ● Drug release at slow and constant rate. ● Increased shelf life compare to aqueous solutions. ● Accurate dosing ● Improved compliance. ● Can administer with inflammed eye. ● Save time of healthcare professional. ● Eliminate systemic side effects. ● Improved patient compliance.
- 54. Mechanism of drug release: Diffusion Osmosis Bio-erosion
- 58. Ocular Inserts
- 60. Erodible Inserts The solid inserts absorb the aqueous tear fluid and gradually erode or disintegrate The drug is slowly leached from the hydrophilic matrix They quickly lose their solid integrity and are squeezed out of the eye with eye movement and blinking Do not have to be removed at the end of their use Three types ● LACRISERTS ● SODI ● MINIDISC
- 61. Mechanism of inserts: Soluble or Erodible ● In swelling-controlled devices, the active agent is homogeneously dispersed in a glassy polymer. Since glassy polymers are essentially drug-impermeable, no diffusion through the dry matrix occurs. When the insert is placed in the eye, water from the tear fluid begins to penetrate the matrix, then swelling and consequently polymer chain relaxation and drug diffusion take place. The dissolution of the matrix, which follows the swelling process, depends on polymer structure: linear amorphous polymers dissolve much faster than cross- linked or partially crystalline polymers. Thus, some inserts, even if classified as S, may remain in the eye as empty ‘ghosts’ after releasing their drug content. Release from these devices follows in general Fickian ‘square root of time’ kinetics; in some instances, however, known as case II transport, zero order kinetics have been observed.
- 62. ● In truly erodible or E-type devices, the rate of drug release is controlled by a chemical or enzymatic hydrolytic reaction that leads to polymer solubilization, or degradation to smaller, water soluble molecules. ● These polymers may undergo bulk or surface hydrolysis. Zero order release kinetics can be displayed by erodible inserts undergoing surface hydrolysis, provided that the devices maintain a constant surface geometry and that the drug is poorly water soluble. Mechanism of inserts: Soluble or Erodible
- 63. 1. LACRISERTS ● Sterile rod shaped device made up of hydroxy propyl cellulose without any preservative ● For the treatment of dry eye syndromes ● It weighs 5 mg & measures 12.5 mm in diameter with a length of 3.5 mm ● It is inserted into the inferior fornix
- 64. 1. LACRISERTS
- 65. 2. SODI (Soluble Ocular Drug Inserts) ● Soluble Ocular Drug Inserts ● Small oval wafer ● Made up of water soluble synthetic polymer ● Sterile thin film of oval shape ● Weighs 15-16 mg ● Introduced into the inferior cul-de-sac. Composition- Acryl amide, vinyl pyrolidone, Ethylacrylate. Use – glaucoma
- 66. ● The SODIs are the result of a vast collaborative effort between eminent Russian chemists and ophthalmologists, and led eventually (in 1976) to the development of a new soluble copolymer of acrylamide, N-vinylpyrrolidone and ethyl acrylate (ratio 0.25 : 0.25 : OS), ● SOD1 in the form of sterile thin films of oval shape (9 x 4.5 mm, thickness 0.35 mm), weighing 15-16 mg, and color-coded for different drugs. ● After introduction into the upper conjunctival sac, a SOD1 softens in 10-15 s, conforming to the shape of the eyeball. In the next 10-15 min the film turns into a polymer clot, which gradually dissolves within 1 h while releasing the drug. The sensation of an ‘extraneous body’ in the eye disappears in 5-15 min. 2. SODI
- 67. ● This dosage form was originally developed for astronauts to apply it in the state of weightlessness. Drug release from SODIs does not show vehicle control, and produces a prolonged-pulse entry of the drug. However, due to the capacity of the ocular tissues to act as drug reservoirs, a single SOD1 application has been reported to replace 4-12 drop instillations or 3-6 applications of ointment, ● Drug is released from SODI in a pulsational, uncontrolled manner, and the dosage form ensures its prolonged effect. ● Active ingredients employed in the course of research on SODI include neomycin, kanamycin, atropine, pilocarpine, dexamethasone, sulfapyridine, and tetracaine. 2. SODI
- 68. ● Based on natural polymers, for example, collagen. ● Based on synthetic or semi-synthetic polymers. ● The therapeutic agent is absorbed by soaking the insert in a solution containing the drug, and drying and rehydrating it before use in the eye. The amount of drug contained will depend upon the capacity of the binding agent, concentration of the drug solution into which the insert is soaked, and the duration of soaking. ● The soluble ophthalmic inserts are easily processed by conventional methods – slow evaporating extrusion, compression or injection molding. The release of the drug takes place when tears penetrate into the insert. This induces drug release by diffusion and forms a layer of gel around the core of the insert. This gelification causes further release of the drug, but it is still controlled by diffusion. The release rate, J, is derived from Fick's law, which yields the following expression 2. SODI
- 69. Advantages: ● Single SODI appliction: repaces 4-12 eye drops instiation. Or 3-6 applications of ointments. ● Once a day treatment of Glaucoma. ● In 10-15 Sec softens; In 10-15 min turns in viscous liquid; After 30-60 min becomes a polymeric solution. API: Neomycin, kanamycin, atropine, pilocarpine, dexamethasone, sulfapyridine, and tetracaine 2. SODI
- 70. 3.MINIDISC Countered disc with a convex front and a concave back surface in contact with eye ball. Diameter – 4 to 5 mm Composition Soluble copolymers consisting of actylamide, N-vinyl pyrrolidone and ethyl acetate -Silicone based prepolymer-alpha-w-dis (4- methacryloxy)-butyl poly di methyl siloxane. (M2DX) M-Methyl acryloxy butyl functionalities. D – Di methyl siloxane functionalities. Pilocarpine, chloramphenicol Drug release: upto 170hrs.
- 73. Contact lenses - Challenges ● Incorporation of sufficient amounts of the drug into the lens matrix; ● sustaining the drug release for the desired time frame at a controlled rate; ● Good optical clarity; ● Patient comfort during prolonged wear; and biocompatibility. ● Prolonged wear of contact lens is associated with risk of infection such as microbial keratitis and dry eye syndrome. ● Wearing of contact lenses is contraindicated in various inflammatory conditions of anterior segment such as anterior uveitis, vernal conjunctivitis, microbial keratitis and dry eye syndrome, limiting the applicability of this delivery system.
- 74. The routes of drug delivery by contact lens ● Drug- loded contact lenses are worn on the cornea to achieve topical administration for the management of ocular diseases. ● As shown in Fig.2, a human tear film contains approximately 6–7 μl of fluid to form a thickness of 7–10 μm. ● When contact lenses are not worn, the tear film covers the cornea, however, after the insertion of a contact lens the tear film is divided into the PLTF and the POLTF.
- 75. ● The PLTF is located on the anterior side of the contact lens, which has direct exposure to air, while the POLTF is located between the cornea and the posterior segment of the contact lens . ● Therapeutic agents in contact lenses are released into both the PLTF and the POLTF. The drug released from the contact lens into the POLTF can be subsequently delivered into the cornea or radially diffuse outwards into the outer tears, and the periodic lens motion can enhance the radial transport. ● The drug delivered into the cornea can reach the anterior segment for the management of ocular diseases through the corneal route. Reversely, drug released from the contact lens into the PLTF is dominantly absorbed into the conjunctiva, further entering the posterior segment and systemic circulation, or drained by the canaliculus. The routes of drug delivery by contact lens
- 76. The process of manufacturing contact lens by different methods ● a. lathe-cut method; b. spin casting method; c. injection molding method. ● CL: Contact lens; HIGH THEM: High temperature.
- 77. Contact lenses
- 78. Soaking in Drug Solutions ● The traditional method is to soak the preformed contact lens in drug solution so that the drug is adsorbed into the polymeric lenses. Drug loading is achieved be either being dissolved in the aqueous phase of the contact lens, or being physically adsorbed on the polymer matrix. ● Due to the drug concentration difference between the soaking solution and aqueous phase of contact lens, molecular diffusion is the main driving force for drug delivery into contact lenses, and is subsequently also the mechanism of drug release from the contact lens. ● Although soaking of preformed contact lenses in drug solution is an easy way to incorporate the drug, this approach suffers from various limitations including low drug loading and fast diffusion of the drug from the lenses. ● Drug upload and release by the soaking method is related to certain factors such as drug concentration in the soaking solution, the molecular weight of the drug, the lens thickness, the type and water content of the lens.
- 79. Soaking in Drug Solutions ● Drugs with a low molecular weight, between 300 and 500 Da, are released from the contact lens over a few minutes to a few hours . High molecular weight drugs such as hyaluronic acid have difficulties penetrating the aqueous channels of contact lens and only remain on the surface ● Such presoaked lenses allow limited, slow release of the drug into the post-lens lacrimal fluid. Soft contact lenses made from poly- hydroxymethacrylate (pHEMA) hydrogels release the majority of their drug content in one day.
- 80. Soaking in Drug Solutions
- 81. Cyclodextrin-based contact lens A. Copolymerization of acrylic/vinyl CDs derivatives B. Grafting of CDs to preformed polymer networks C. Directing cross-linking of CDs
- 82. ● Molecularly imprinted contact lenses exhibited a more prolonged drug release when compared with lenses soaked in drug solution. Molecularly imprinted contact lenses of ketotifen (diffusion coefficient: 5.57 ± 0.31 × 10 cm2 /s) showed a diffusion coefficient that was nine-times lower than nonimprinted lenses (50.2 ± 4.8 × 10 cm2 /s). Molecularly imprinted polymeric hydrogels
- 83. Conjugation of nanoparticles or drug molecules to contact lens surface ● Another approach to prepare contact lens drug delivery systems is to immobilize the drug or drug-loaded nanocarriers such as liposomes and nanoparticles on the surface of commercial soft contact lenses. ● This can be achieved by surface functionalization of contact lenses to attach the drug or nanocarriers. Surface immobilization of levofloxacin liposomes on NeutrAvidin-coated Hioxifilcon-B contact lenses resulted in slower release than drug soaked lenses. ● However, most of the drug (70%) was released within the first 5 h, with 30% remaining drug release occurring over the next 6 days. Thus, the drawback of this approach is the relatively rapid detachment or disintegration of liposomes in the contact lenses. ● The lipid layer may also impede O2 and CO2 permeability.
- 86. ● Recent research from the Massachusetts Eye & Ear Infirmary (Needham, MA, USA) demonstrated that near zeroorder, 4-week release of ciprofloxacin and fluorescein is feasible from a drug-polymer film (poly[lactide-co- glycolide] [PLGA] 65:35) coated with a hydrogel (pHEMA) contact lens. ● In vitro release studies showed that the drug release rate can be reduced by using highmolecular- weight polymers or increasing the polymer-to-drug ratios. Drug-polymer films integrated with contact lenses
- 87. Liposome-loaded contact lenses ● In this method, drug-loded nanoparticles, liposomes or surfactant are added to the polymerizing medium of hydrogel matrix followed by polymerization to form contact lenses dispersed with drug carriers. ● The overall drug release can be regulated by controlling the release of the drug from the various carriers, followed by the lens matrix to the post-lens tear film. ● Contact lenses created with dispersion of lidocaine loaded liposomes or nano-particles showed nonlinear release of drug for 7 days, with an initial 15–20% burst release over the first few hours followed by near zero-order release for the remaining 7 days.
- 88. Scleral lens delivery systems ● The scleral lenses were first approved by the FDA in 1994 for the management of ectasia and irregular astigmatism. Scleral lenses are large diameter lenses which rest over the sclera, unlike the conventional contact lenses which rest on the cornea. ● These lenses are fitted to not touch the cornea and there is a space created between the cornea and the lens. These lenses are inserted in the eyes after filling with sterile isotonic fluid. ● A scleral lens rests on the sclera and creates a space over the cornea and limbus, acting as a reservoir for tear fluid between the inner surface of the scleral lens and the cornea to form an expanded tear film. ● This expanded tear film over the cornea acts as a liquid bandage in corneal surface irregularities. ● The scleral lens allowed improved retention of topically applied drug on the corneal surface in the expanded tear film, that is, the tear film or artificially introduced tears retained between the corneal surface and the scleral lens. ● The drug may be added to the scleral lens, which acts as a reservoir for sustained release of the drug, or administered externally as an eye drop, which is retained in the expanded precorneal tear film. ● The topical delivery of Avastin for the treatment of corneal neovascularization using scleral lens delivery system showed promising results in a clinical study with five patients.
- 89. Scleral lens delivery systems
- 90. Ocular Implants
- 91. Non-biodegradable polymeric implants ● These implants can entrap drug either by dispersion throughout a polymer matrix or storage inside a reservoir surrounded by a release controlling non-biodegradable polymer membrane. ● Drug release from non-biodegradable matrix systems is governed by diffusion and an initial burst is often observed. ● On the other hand, reservoir systems release the drug either through permeable non-biodegradable membranes or ia a small orifice in an impermeable membrane. ● Both of these systems have shown near zero order drug release of effective concentrations over extended periods of time. ● Polyvinyl alcohol (PVA), ethylene vinyl acetate (EVA) and silicon are the most commonly used non-biodegradable polymers for ocular implants.
- 92. ● Silicon and EVA are hydrophobic in nature and are mainly used as membranes with limited permeability in reservoir based systems. On the other hand, PVA is more hydrophilic and therefore permeable to a broader range of drugs. Often a combination of PVA with either EVA or silicon is utilized to optimize drug release from the implant. ● Vitrasert, approved by the FDA in 1996, is a non-biodegradable implant containing 4.5 mgof ganciclovir for the treatment of CMV retinitis. It contains the drug in form of a pellet coated with two layers of nonbiodegradable polymers. The inner coating is PVA, with the outer impermeable coating of EVA on three sides and an additional PVA layer on the remaining side. Drug permeates via the permeable PVA coated side at a rate of approximately 24 μg/day and the implant has shown clinical suppression of disease symptoms over five to eight months. Non-biodegradable polymeric implants
- 93. ● Vitrasert is sutured to the pars plana region of the sclera. Common complications with the use of this implant include endophthalmitis, cataract formation, intraocular pressure increase and risk of retinal detachment. ● In general, non-biodegradable polymers are preferred for implant fabrication to deliver therapeutics to the posterior segment as they release the drug in a more controlled manner over extended periods of time, while also offering easier removal in case of adverse reactions. Fabrication of refillable non- biodegradable implants might therefore be advantageous in terms of patient compliance and overall treatment costs. Non-biodegradable polymeric implants
- 94. Biodegradable polymeric implants ● These implants are made from biodegradable polymers entrapping the drug either throughout a polymer matrix or in form of a reservoir with biodegradable polymer coating. From matrix systems the drug is released through a combination of diffusion and polymer degradation. ● In reservoir based implants drug is mainly released through a pore in the otherwise impermeable membrane with the biodegradable polymer coating degrading relatively slow compared to the drug release out of the system. With matrix biodegradable systems, there is generally an initial burst and then a fairly constant release rate over time, with a final burst observed in reservoir systems. Drug release can vary depending on the surface area, rate of polymer degradation, polymer swelling, molecular weight and nature of the drug molecule. ● Polylactic acid (PLA), polyglycolic acid (PGA), poly(lactic-co-glycolic acid) (PLGA), polycaprolactones (PCL), polyanhydrides (PA) and polyortho esters (POE) are commonly used biodegradable polymers for ophthalmic drug delivery, with PLGA being the most widely studied. These polymers are all aliphatic esters which are degraded in the body by water and/or enzymes with their degradation products being metabolized into CO2 and water.
- 95. ● Ozurdex, the first biodegradable intravitreal implant approved by the FDA, is a cylindrical implant comprising dexamethasone dispersed in a PLGA matrix based on the NOVADUR® technology (Allergan). It contains 700 μg of dexamethasone and has proven to be clinically effective for up to sixmonths in the treatment of diabetic macular edema and non-infectious uveitis. It is injected into the vitreous via a 22-gauge needle and exhibits fast drug release over the first twomonths due to diffusion of the drug and degradation of the polymer after which solely polymer degradation is responsible for the slower drug release over the following four months.
- 97. Stimuli-responsive implants ● Implants made from stimuli-responsive polymers exhibit abrupt changes in structure, solubility, charge, volume and hydrophobic– hydrophilic balance in response to physical or chemical changes in the environment and can be utilized to tune drug release rates.
- 98. Iontophoresis ● Iontophoresis is a noninvasive technique for ocular drug delivery, and therefore avoids the complications of a surgical implantation or frequent and high dose of intravitreal injections. The drug is applied with a weak direct current (DC) that drives charged molecules across the sclera and into the choroid, retina, and vitreous. A ground electrode of the opposite charge is placed elsewhere on the body to complete the circuit. ● The drug serves as the conductor of the current through the tissue. In the rabbit iontophoresis of DEX phosphate, DEX levels in the cornea after a single transcorneal iontophoresis for 1 min (1 mA) were up to 30 fold higher compared to those obtained after frequent eye-drops instillation.
