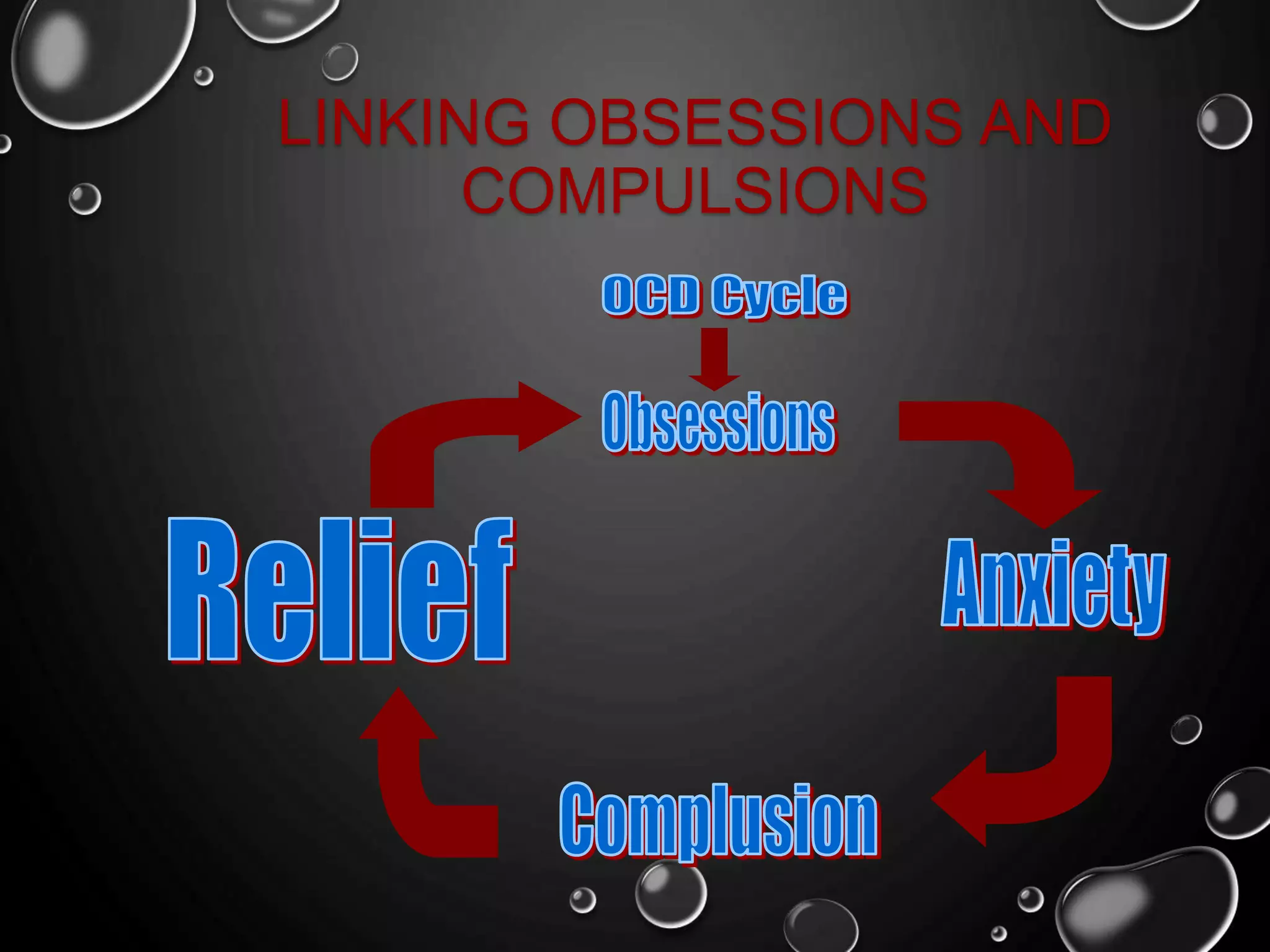
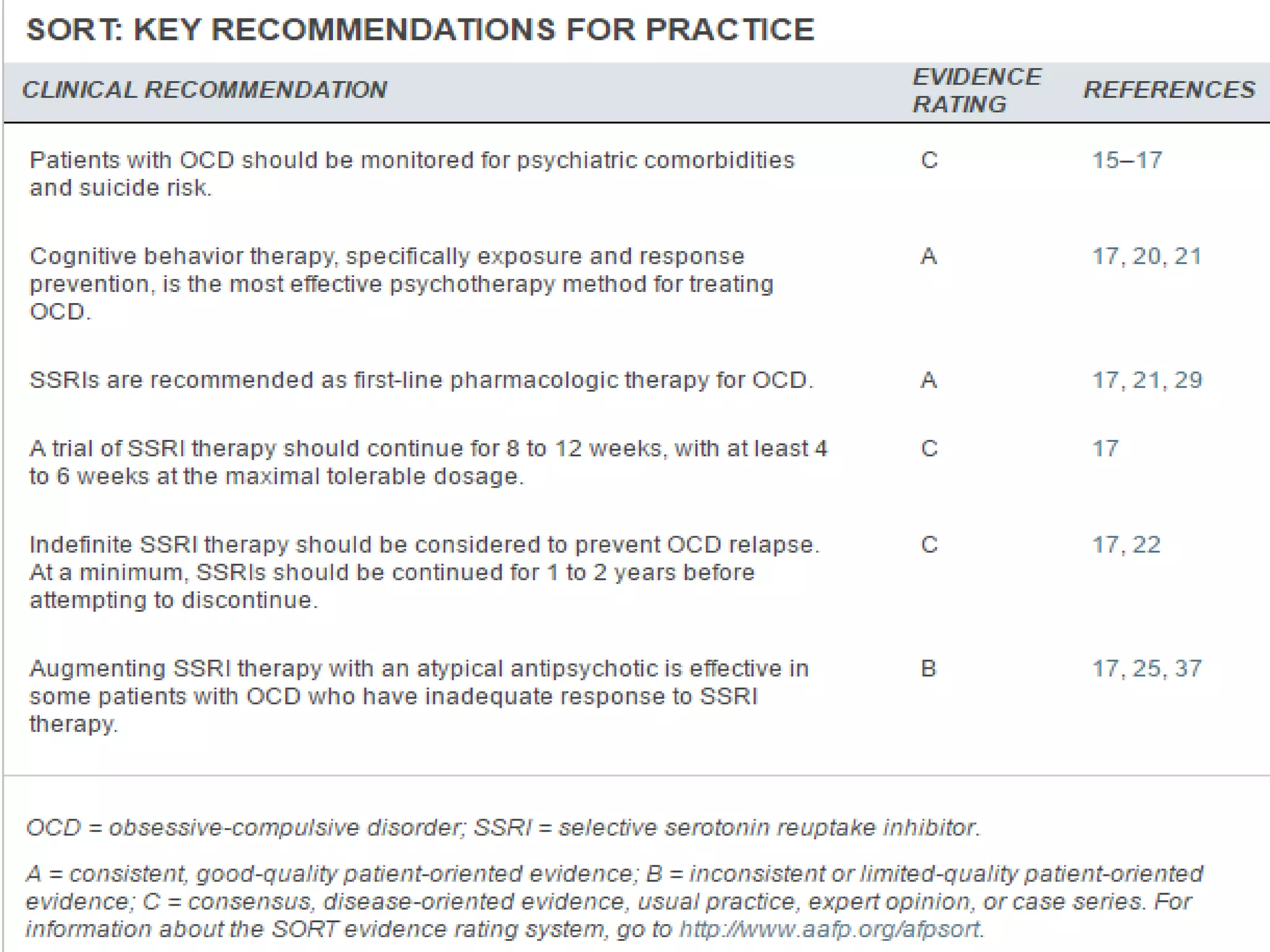
This document provides an overview of obsessive-compulsive disorder (OCD), including its definition, epidemiology, clinical manifestations, diagnosis, differential diagnosis, management, and recommendations. OCD is characterized by recurrent obsessions and compulsions that cause distress or impairment. It has a lifetime prevalence of 2.3% and typically starts in childhood or adolescence. Treatment involves cognitive-behavioral therapy, selective serotonin reuptake inhibitors, or a combination of both.