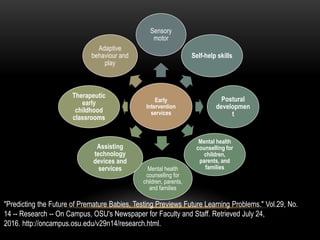
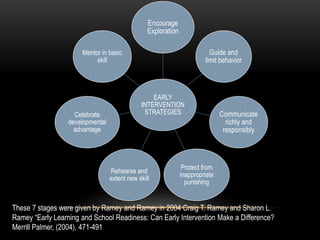
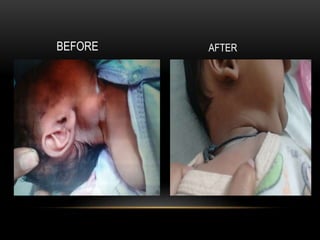
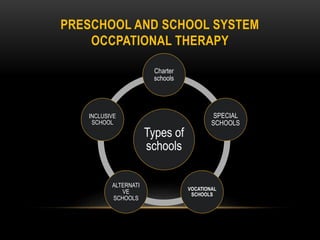
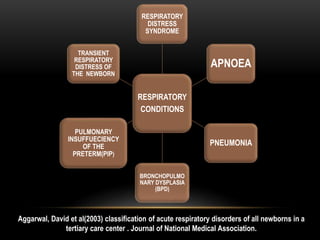
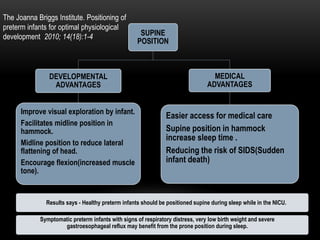
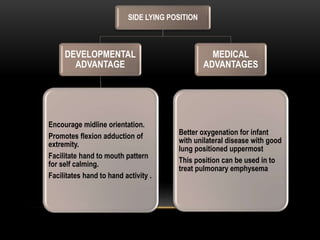
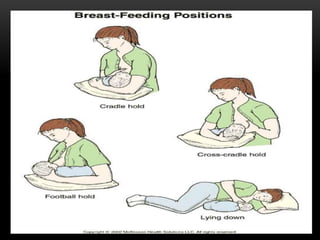
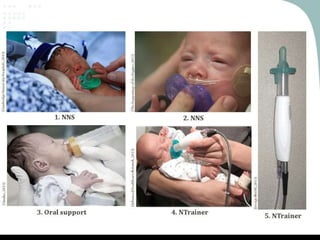
The document discusses the interventions and assessments for high-risk infants from birth to school age, addressing various risk factors and developmental challenges they face. It outlines guidelines for occupational therapy, including techniques for feeding, sensory integration, and the importance of early intervention strategies to enhance developmental outcomes. Additionally, it provides a case study exemplifying effective occupational therapy practices and their impact on a child's recovery.

























![ASSESSMENT TOOLS USED IN EARLY
INTERVENTION
• Inventories measure a child’s development in five domains:
gross motor, fine motor, language, comprehension, and
person-social. Items tap the better predictors of
developmental status only. A 300-item assessment-level
version may be useful in follow-up
• the Infant Development Inventory (IDI), 3 - 72 months;
• Early Child Development Inventory (ECDI) for 3-18 months;
• Preschool Development Inventory (PDI)] each with 60 yes-
no descriptions. ; 3660 months
Child
Development
Inventories (CDI)
• 12 – 96 months
• The 96 items use a combination of direct assessment,
observation, & parental interview.
• The BDIST taps a range of discrete domains including
receptive & expressive language, fine & gross motor,
adaptive, personal-social, & cognitive/academic.
Battelle
Developmental
Inventory
Screening Test
(BDIST)](https://image.slidesharecdn.com/occupationaltherapyinhighrisk-170525081143/85/Occupational-Therapy-in-high-risk-42-320.jpg)