1. Heart failure is a clinical syndrome where the heart is unable to pump enough blood to meet the body's needs. It becomes more prevalent with age due to cardiovascular changes and diseases.
2. Over 550,000 new cases of heart failure are diagnosed yearly in the US, with rates doubling each decade after age 45. The most common causes in the elderly are high blood pressure, coronary artery disease, and valvular heart disease.
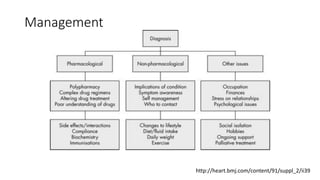
3. Management of heart failure in the elderly focuses on treating the underlying cause, nonpharmacological therapies like exercise and diet, and use of medications like ACE inhibitors, beta-blockers, diuretics, and aldosterone antagonists. Regular monitoring and support are