The document provides an overview of the London Better Care Fund programme, including:
- The BCF aims to integrate health and social care services to provide more coordinated person-centered care.
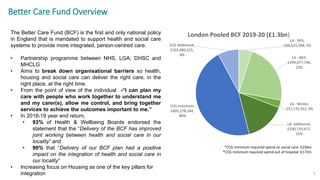
- In London, over £1.3 billion was pooled in the 2019-2020 BCF, with most spent on residential placements, community services, and integrated care planning.
- London performs well on BCF metrics like reablement and reducing residential admissions compared to other regions, but non-elective admissions are rising.
- The BCF requires joint planning between health and local authorities, including on issues like housing, home adaptations, and passing down funding to districts.
- The future of the BCF beyond 2020-