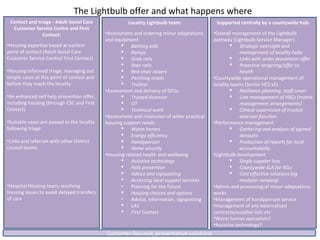
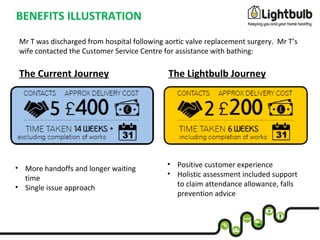
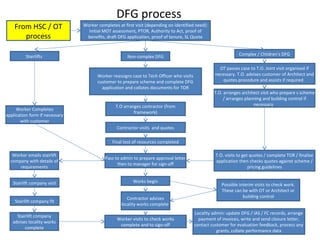
The document outlines plans to transform housing support across Leicestershire through a new integrated service called Lightbulb. Lightbulb will provide a proactive and targeted approach to addressing housing needs, with the goals of improving health outcomes, reducing costs to health and social care, and creating a better customer experience. Key aspects of Lightbulb include establishing Housing Support Coordinators, a Hospital Housing Enabler team, and a holistic housing assessment. Pilots of Lightbulb services demonstrate reductions in service usage, falls, and delayed hospital discharges as well as improved customer outcomes.