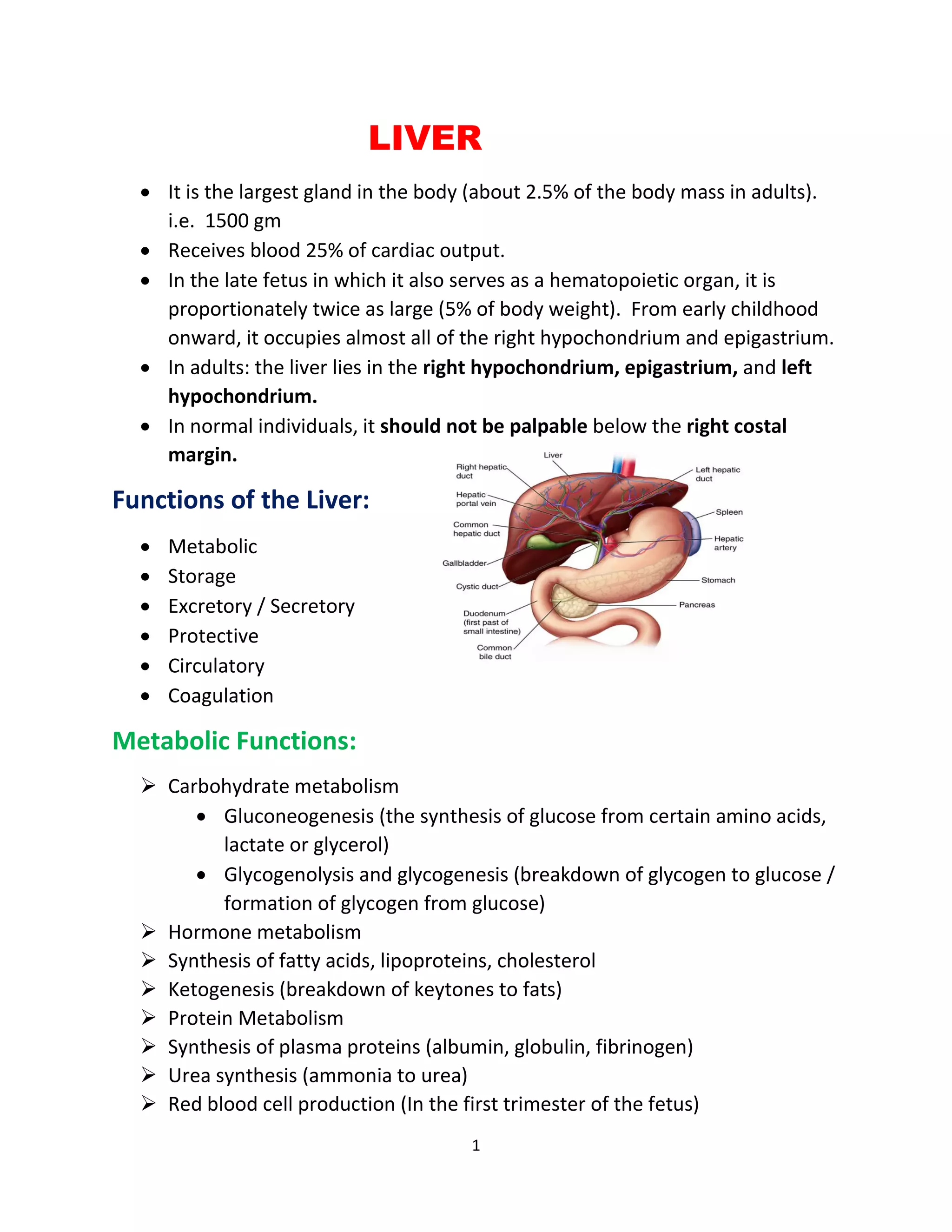
The liver is the largest gland in the body and performs many critical metabolic functions like carbohydrate and protein metabolism. It also plays an important role in hormone regulation, bile production, and blood clotting factor synthesis. Chronic liver disease can lead to liver fibrosis and cirrhosis over many years. Cirrhosis is characterized by liver scarring and nodule formation, resulting in loss of liver function. Common causes include alcohol abuse, viral hepatitis, and non-alcoholic fatty liver disease. Complications arise due to portal hypertension and liver failure. Diagnosis involves liver biopsy or lab tests showing abnormalities in liver enzymes and clotting factors.