Icm peritoneal dialysis 234
- 7. Principles of peritoneal dialysis Continuous Ambulatory Peritoneal Dialysis-CAPD
- 8. Principles of peritoneal Continuous Cycling Peritoneal Dialysis (CCPD) or Automated Peritoneal Dialysis ( APD ) Cycler Nightly Intermittent Peritoneal Dialysis
- 12. Diffusion through the pores of capillary wall
- 14. Principles of peritoneal dialysis 1)transcellular, water-only aquaporin; 2) intercellular gap lined by a dense glycocalyx 3) intercellular gap with a less dense glycocalyx that permits macromolecules to pass
- 15. Peritoneal solute transport : diffusion through the pores of capillary wall
- 16. Normal Distribution (Gauss Curve ) Weight Height
- 18. Normal distribution Results of baseline PET Ramesh Khanna & Karl D. Nolph
- 19. Assessement of PD adequacy PET (peritoneal equilibrium test) determines quick or slow passage of toxins from the blood into the dialysis fluid ‘high-fast transporters’ v.s. ‘low-slow transporters’ helps to decide about the PD scheme (dwell duration and intervals, CAPD vs. CCPD) performed in hospital, takes 5 hours involves doing a CAPD exchange using a 2.27% G, samples of PD fluid and blood are taken at set times
- 20. Distribution of Peritoneal Membrane Filtration Capacity
- 21. PET (peritoneal equilibration test) Transporter Waste Water Best type of removal removal PD High Fast Poor Frequent exchanges, short dwells – APD Average OK OK CAPD or APD Slow Slow Good CAPD, 5 exchanges daily + 1 exchange at night
- 26. Structure of Icodextrin α (1→6) branch Main α (1→4) chain
- 32. Neoangiogenesis in Peritoneum VEGF staining Glucose Solutions
- 35. Peritoneal Transport Status + Mortality JASN January 2006
- 36. Peritoneal Transport Status + Mortality Peritoneal transport status is a highly significant risk factor for both mortality and death-censored technique failure in incident PD patient populations. JASN January 2006
- 37. Peritoneal Transport Status + Mortality Peritoneal transport status is a highly significant risk factor for both mortality and death-censored technique failure in incident PD patient populations. This risk is independent of demographic characteristics, BMI, comorbid clinical illnesses, peritoneal small solute clearances, and residual renal function. JASN January 2006
- 38. Peritoneal Transport Status + Mortality Peritoneal transport status is a highly significant risk factor for both mortality and death-censored technique failure in incident PD patient populations. This risk is independent of demographic characteristics, BMI, comorbid clinical illnesses, peritoneal small solute clearances, and residual renal function. This association was not found in APD patients. JASN January 2006
- 39. Meta-Analysis: Peritoneal Membrane Transport, Mortality, and Technique Failure JASN September 2006
- 40. Meta-Analysis: Peritoneal Membrane Transport, Mortality, and Technique Failure A higher rate of peritoneal membrane solute transport is associated with increased mortality in PD patients. JASN September 2006
- 41. Meta-Analysis: Peritoneal Membrane Transport, Mortality, and Technique Failure A higher rate of peritoneal membrane solute transport is associated with increased mortality in PD patients. Peritoneal solute clearance does not significantly influence patient outcome within usual PD dosing regimens whereas clinical volume status may. JASN September 2006
- 42. PET (peritoneal equilibration test) Transporter Waste Water Best type of removal removal PD High Fast Poor Frequent exchanges, short dwells – APD Average OK OK CAPD or APD Slow Slow Good CAPD, 5 exchanges daily + 1 exchange at night
- 44. Ultrafiltration Failure in PD In UF failure, fluid removal is insufficient
- 45. Ultrafiltration Failure in PD In UF failure, fluid removal is insufficient This can lead to fluid overload
- 46. Ultrafiltration Failure in PD In UF failure, fluid removal is insufficient This can lead to fluid overload Excess of fluid and sodium can lead to cardiovascular mortality
- 49. UF failure occurs in 35% of long term PD patients and is an important factor for transfer to HD
- 50. UF failure occurs in 35% of long term PD patients and is an important factor for transfer to HD
- 51. UF failure occurs in 35% of long term PD patients and is an important factor for transfer to HD UF failure is diagnosed from a 3.86% PET
- 52. UF failure occurs in 35% of long term PD patients and is an important factor for transfer to HD UF failure is diagnosed from a 3.86% PET
- 53. UF failure occurs in 35% of long term PD patients and is an important factor for transfer to HD UF failure is diagnosed from a 3.86% PET Failure to achieve a UF of > 1.0L is associated with increased mortality
- 54. UF failure occurs in 35% of long term PD patients and is an important factor for transfer to HD UF failure is diagnosed from a 3.86% PET Failure to achieve a UF of > 1.0L is associated with increased mortality
- 55. UF failure occurs in 35% of long term PD patients and is an important factor for transfer to HD UF failure is diagnosed from a 3.86% PET Failure to achieve a UF of > 1.0L is associated with increased mortality Long term exposure to dialysis solutions is likely to be the most important risk factor
- 56. Causes of UF failure • Large vascular surface of peritoneum (due to neo- angiogenesis, vasodilation), leading to high (fast) transport including fast lost of osmotic (glucose) pressure • Decreased function of aquaporins • High lymphatic absorption
- 57. Extraneal vs. 4.25% Dextrose 600 * * Long Dwell Net UF (mL) Icodextrin 500 400 300 4.25% Dextrose 200 100 0 Baseline Week 1 Week 2 *P < 0.005 vs 4.25% dextrose. Finkelstein, et al. J Am Soc Nephrol 2005;16:546-554.
- 58. Icodextrin + fluid balance Davies et al, JASN: 2003:14:2338
- 59. Icodextrin + fluid balance Icodextrin vs 2.27% dextrose in long dwell. Davies et al, JASN: 2003:14:2338
- 60. Icodextrin + fluid balance Icodextrin vs 2.27% dextrose in long dwell. Better preservation of UF (+193 vs -201) Davies et al, JASN: 2003:14:2338
- 61. Icodextrin + fluid balance Icodextrinvs 2.27% dextrose in long dwell. Better preservation of UF (+193 vs -201) Sustained reduction in weight. Davies et al, JASN: 2003:14:2338
- 62. Icodextrin + fluid balance Icodextrin vs 2.27% dextrose in long dwell. Better preservation of UF (+193 vs -201) Sustained reduction in weight. Preservation of RRF Davies et al, JASN: 2003:14:2338
- 64. Etiology of Fibrosis GDP AGE PD Fibrosis Biofilm Inflammation Plasticizers
- 65. Morphologic changes of peritoneum due to PD Before starting PD: normal peritoneum
- 66. Morphologic changes of peritoneum due to PD After 3 years on PD, submesothelial fibrosis and neo- angiogenesis (increase of vascular area of peritoneum)
- 67. Morphologic changes of peritoneum due to PD COMPLICATION: Encapsulating peritoneal fibrosis
- 68. PERITONEAL FIBROSIS : SIMPLE SCLEROSIS AND SCLEROSING PERITONITIS Simple Sclerosis Sclerosing Peritonitis Frequency very common very rare poor biocompatibility of peritoneal dialysis due to osmotic agents, unknown, only risk factors hyperosmolarity, low pH, peritoneal dialysis-dependent risk factors: buffer duration of dialysis poor biocompatibility acetate buffer Etiology disinfectants catheter in-line bacterial filters particles of plastics plasticizers peritonitis peritoneal dialysis-independent risk factors: beta-blockers tumors genetic predisposition Reproducibility yes with dialysis no with dialysis in animal models no without dialysis yes without dialysis Clinical severe absent manifestations high mortality
- 69. Simple sclerosis Sclerosing Peritonitis of macrophagic origin Giant sclerotic tissue limited to visceral and cells parietal peritoneum Fibroblasts and mesoblasts occur throughout the thickness of sclerotic tissue in the sclerotic tissue, but are often more frequent in deeper layers. In sclerosing simple sclerosis does not exceed peritonitis unlike simple sclerosis, the muscle 40-50 µm layer is compressed. The thickness of the sclerotic tissue is not uniform in a given patient
- 70. In sclerosing peritonitis, unlike simple sclerosis, a dramatic progression of the sclerosis occurs. This is combined with aspects not found in simple sclerosis, such as inflammatory infiltrates, calcifications and typical vascular alterations. The peritoneal surface is reduced to a rough thickened membrane similar to the sole of a shoe .In extreme cases of sclerosing encapsulating peritonitis, the sclerotic process completely fixes groups of intestinal loops, almost completely preventing their movement. Often the sclerosis is not homogeneous, but one area of the abdomen may be more affected than others, forming a mass. This situation has been described with the term "abdominal cocoon“. The cocoon may be perfectly palpable, like a tumor; the sclerotic tissue of the cocoon usually contains loops of the small intestine and sacs of ascites, and often calcifications.
- 77. EPS-cocoon
- 79. Encapsulation of small bowel
- 81. Etiology of Fibrosis RAGE Neovascularization TGF beta, VEGF IL-6 (GG Phenotype) K.Kaneko EMT
- 82. Development of new PD solutions New solutions – Extraneal – Gambrisol Trio – Balance – Physioneal – BicaVera – Nutrineal
- 83. Absorption of glucose from peritoneal solutions 1. Solutions containing glucose (green) lead to significant glucose absorbtion 2. Solutions based on another osmotic agent (blue, violet) do not lead to glucose absorbtion, so decrease total daily glucose load). 1 2
- 84. Absorption of glucose from peritoneal solutions 1. Solutions containing glucose (green) lead to significant glucose absorbtion 2. Solutions based on another osmotic agent (blue, violet) do not lead to glucose absorbtion, so decrease total daily glucose load). Glucose absorbed = 159 g/day 1 2.5 L 2.5 L 2.5 L 2.5 L Physioneal Physioneal Physioneal Physioneal 1.36% 1.36% 1.36% 3.86% 2
- 85. Absorption of glucose from peritoneal solutions 1. Solutions containing glucose (green) lead to significant glucose absorbtion 2. Solutions based on another osmotic agent (blue, violet) do not lead to glucose absorbtion, so decrease total daily glucose load). Glucose absorbed = 159 g/day 1 2.5 L 2.5 L 2.5 L 2.5 L Physioneal Physioneal Physioneal Physioneal 1.36% 1.36% 1.36% 3.86% Glucose absorbed = 50 g/day 2.5 L 2.5 L 2 Physioneal 2.5 L Physioneal 2.5 L 1.36% Nutrineal 1.36% Extraneal
- 86. Composition of Extraneal DIANEAL® PD2 EXTRANEAL™ Dextrose (g/dL) 1.5, 2.5, 4.25 --- Icodextrin (g/dL) --- 7.5 Sodium (mEq/L) 132.0 132.0 Chloride (mEq/L) 96.0 96.0 Calcium (mEq/L) 3.5 3.5 Magnesium (mEq/L) 0.5 0.5 Lactate (mEq/L) 40.0 40.0 Osmolality (mOsm/kg) 346-485 282 pH 5.2 5.2
- 87. Composition of Physioneal DIANEAL® PHYSIONEAL™ Dextrose (g/dl) 1.5, 2.5, 4.25 1.5, 2.5, 4.25 Sodium (mEq/L) 132.0 132.0 Chloride (mEq/L) 95, 96 95, 96 Calcium (mEq/L) 2.5, 3.5 2.5, 3.5 Magnesium (mEq/L) 0.5 0.5 Lactate (mEq/L) 40.0 15.0 (10.0) Bicarbonate (mmol/ --- 25.0 L) pH 5.2 7.4 Osmolality (mOsm/ 346-485 346-485 kg)
- 88. Concentrations of Advanced Glycation End Products Methylglyoxal Glyoxal 3-Deoxyglucosone micromol/L micromol/L micromol/L Dianeal 1.5% 4.0 3.5 224 2.5% 5.1 6.2 335 4.25% 6.9 9.4 525 Physioneal 1.5% 0.4 1.6 138 2.5% 0.4 3.3 158 4.25% 1.1 6.0 253 PDI 2000;20:796
- 89. Standard Solutions VEGF Staining Physioneal Mortier S. et al. Kidney Int 2004;66;1257.
- 90. BicaVera Fresenius 1.5%, 2.5%, 4.25% glucose Bicarbonate as buffer (34 mmol/ L) Neutral pH 7.4 Low GDP
- 91. New Peritoneal Dialysis Solutions - nature Clinical Practice Nephrology- Nov 2007
- 92. הקשבתם ?? ?? Ằ ẽ ẵằ Ẽסוף סוף זה הסוף !!
- 93. Thank you!!
- 94. Relative contraindications of PD pleuro-peritoneal * diverticulosis leakage • colostomy hernias • obesity • blindness significant loin pain big polycystic kidneys severe deformant arthritis psychosis significant decrease of lung functions
- 95. Criteria of PD Adequacy
- 96. Perspectives - New dialysis solutions protect peritoneal membrane Physioneal1 ↓ GDPs and AGEs Extraneal2 ↓ Lactate • Isosmolar to plasma Physiologic pH and pCO2 • No glucose exposure ↑ Membrane and immune cell • ↓ GDPs and AGEs function • ↑ Membrane and immune cell function Nutrineal2 No glucose exposure No GDPs or AGEs ↑ Membrane and immune cell function
Editor's Notes
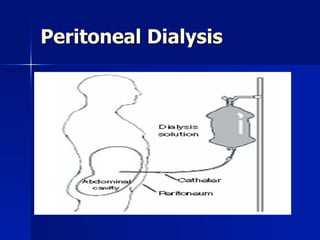
- another way to clean the blood- while leaving it in the body\n- put water in peritoneal membrane- has 2 m\n- the waste products will come out through the dialysis\n(dont have to take the blood out of the body)\n- peritoneal cavity = reservoir of dialysis solution\n- need to put catheter in body\n- dialysis will go out with waste products\n
- \n
- diff kinds of catheters\n\n
- when finish dialysis- disconnect, and put catheter in bandage on abdomen/ underwear...\n\n\n
- venous clamp-\nhow make out fluid? cant put clamp on venous side of splanchnic circulation- so how take out water?\n- how take the excessive water from the blood\n= osmotic force: needs to be concentrated- put osmotic substance in the water that you are putting into the peritoneum so that it will pull out the water form the blood\n- glucose is the osmotic substance used\n\n
- \n
- water out in, close: 7-12, then take it out.....\n- can do it alone at home- ambulatory- doesnt need to come in\n- all the time there is fluid - occurs throughout the whole day\n
- small machine nowadays- that only have to do it at night\nNIPD: nightly intermittent peritoneal dialysis\n- more small cycles are done- continuous small cycle dialysis\n\n
- \n
- \n
- \n
- \n
- \n
- 3 kinds of pores in peritoneum\n- aquaporin (1)\n- small pores- btw the cells\n glycocalyx- lets molecules to pass through small pore (medium molecules)\n- bigger pore- bigger molecules can pass through\n\nso a lot of materials can be cleared- many sizes\n\n\n\n-the protein can pass through- so peritoneal dialysis- lose protein: hypoalbuminemic\n\n
- \n
- \n- height and weight differs\n\n\n
- - peritoneum moves- some molecules go in and out\n\n\n
- distribution in pop of how the peritoneum transports the fluids\n- most ppl: peritoneum is average transporter\n- some high transporters\n- some low transporter\n
- we need to know if the peritoneum is an active or lazy one- wich determines how the dialysis will work\n- PET: in oreder to assess the peritoneum quality\n- help determine the PD scheme- how long the dialysis needs to be in the stomach (if high transporter- doesnt need to be in for very long)\n
- osmotic power lost quickly if high transporter- so, blood will be more osmotic than the fluid, and then it will be absorption of water, rather than clearance of the blood\n- need to change the dialysis on time- or high transporter pt will gain weight\n\n- depend on how transporters work in individual pt\n
- \n
- \n
- \n
- \n
- after 4 hours- need to change\n\n- if glucose more concentrated - take more time to lose\n\n\n
- but glucose not so kind to the body\npolyglucose molecules- not as small as glucose- cant pass- so there is osmosis at all times- so can stay in the abdomen for a long time- wont lose its osmosis\n\n\nIcodextrin is a starch-derived high molecular weight (MW) glucose polymer that is structurally similar to glycogen.1 It consists of oligosaccharide polymers of D-glucopyranose linked by >90% &#x3B1;1-4 and <10% &#x3B1;1-6 glucosidic bonds. \nIcodextrin differs from glycogen in that it has a lower percentage of alpha1-6 linkages, and is thus not as highly branched.2,3 The number of linked glucose molecules ranges anywhere from 4 to >300 with a number-average MW between 5,000 and 6,500 Daltons. The weight-average MW of icodextrin, the most common and accurate way of reporting average MW for large polymers, is between 13,000 and 19,000 Daltons.1,2 \nAs a high molecular weight glucose polymer, icodextrin does not readily diffuse across the peritoneal membrane. Rather, it is slowly removed from the peritoneal cavity via lymphatic absorption. As a result, icodextrin is able to maintain osmotic forces and sustain ultrafiltration over longer dwell periods compared with conventional dextrose-based peritoneal dialysis solutions.\n\n\n
- \n
- polyglucose- doesnt lose its osmotic force!\n
- can cause peritoneal membrane abnormalities\n- glucose degradation products are bad all the time\n
- \n
- right: accum of glycose end-products (stained brown) after long term peritoneal dialysis \n(diabetics- proliferation of vessels in the eye- retinopathy- glucose can cause proliferation of the vessels- tx of diabetic nephropathy= laser)\n-hypoxia: VEGF\n- when put glucose: make hyperglycemic environment int he abdomen: some pts that are prone to diabetes, become diabetic due to this dialysis\n- EVGF in peritoneum- more blood vessels are formed (similarly to the retina)\n- peritoneum can then transform from average transporter to high transporter- bc absorb faster bc have more vessels\n
- right: with time- more VEGF staining\n
- \n
- during time- start dialysis\n- ppl transform form average transporter to high transporters\n
- high transporters- greater mortality\n
- high transporters- greater mortality\n
- high transporters- greater mortality\n
- \n77% higher RR for mortality HI vs LA\n
- \n77% higher RR for mortality HI vs LA\n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- less water pulled out from pt\n
- \n
- Figure 3. Changes in (a) total body water and (b) extracellular fluid determined from bioelectrical impedance. At each time point, values represent mean &#xB1; SEM change from baseline for patients randomized to icodextrin ( ) or 2.27% glucose ( ). Between-group differences, P < 0.04, P < 0.008. Longitudinal differences from baseline, * P < 0.002, ** P < 0.001. \n
- Figure 3. Changes in (a) total body water and (b) extracellular fluid determined from bioelectrical impedance. At each time point, values represent mean &#xB1; SEM change from baseline for patients randomized to icodextrin ( ) or 2.27% glucose ( ). Between-group differences, P < 0.04, P < 0.008. Longitudinal differences from baseline, * P < 0.002, ** P < 0.001. \n
- Figure 3. Changes in (a) total body water and (b) extracellular fluid determined from bioelectrical impedance. At each time point, values represent mean &#xB1; SEM change from baseline for patients randomized to icodextrin ( ) or 2.27% glucose ( ). Between-group differences, P < 0.04, P < 0.008. Longitudinal differences from baseline, * P < 0.002, ** P < 0.001. \n
- Figure 3. Changes in (a) total body water and (b) extracellular fluid determined from bioelectrical impedance. At each time point, values represent mean &#xB1; SEM change from baseline for patients randomized to icodextrin ( ) or 2.27% glucose ( ). Between-group differences, P < 0.04, P < 0.008. Longitudinal differences from baseline, * P < 0.002, ** P < 0.001. \n
- - after 5 yrs dialysis: peritoneum is MUCH THICKER\n- peritoneum can also become fibrotic- more collagen, more VEGF\n
- \n
- \n
- more vessels and more fibrosis in the peritoneum\n
- rare complication: \n- strangulate/encapsulate the small bowels- obstruction of the intestine\n(after 7/8 yrs)- switch ppl over to hemodialysis: not more than 7 yrs- bc of danger of complications\n
- \n
- \n
- \n
- \n
- \n
- \n
- right: calcification fo peritoneum- intestine- \n\nstrangulation of the bowels \n
- \n
- \n
- \n
- very difficult surgery\n
- rare- but can happen\n\nLAST SLIDE\n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- \n
- Category: Peritoneal Membrane Preservation \nThis slide shows the beneficial effects of the newer PD solutions containing alternate buffers and osmotic agents.\nAll three solutions reduce levels of GDPs and AGEs. With Physioneal, it is because glucose is sterilized at a very low pH. With Extraneal and Nutrineal, it is because there is no glucose in either solution.\nAdditional benefits of Physioneal : Physiologic pH and pCO2, reduced lactate levels.\nAdditional benefit of Extraneal: Same osmolarity as plasma.\nAs a result of its unique properties, each solution has been shown to improve membrane and peritoneal immune cell function.\n
- \n
- \n