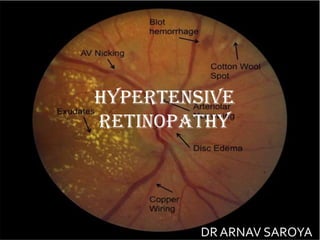
HYPERTENSIVE RETINOPATHY - DR ARNAV SAROYA
•Download as PPTX, PDF•
0 likes•543 views
THIS PRESENTATION COVERS ALL ASPECTS OF HTN RETINOPATHY - EPIDEMIOLOGY , PATHOPHYSIOLOGY , CLINICAL FEATURES AND TREATMENT
Report
Share
Report
Share
Recommended
HYPERTENSIVE RETINOPATHY.pptx

This document summarizes hypertensive retinopathy, which occurs when retinal vessels are damaged due to elevated blood pressure. It discusses the types and clinical features of hypertensive retinopathy, including changes to retinal arteries and veins seen on examination. It also covers classifications of hypertensive retinopathy based on vessel changes and light reflexes. Risk factors, pathophysiology, and complications are described. Treatment involves controlling blood pressure through lifestyle changes and medication. Uncontrolled high blood pressure can lead to further eye and systemic damage.
Hypertensive retinopathy converted

This document discusses hypertensive retinopathy, which is caused by high blood pressure damaging the small blood vessels in the retina. It begins by covering the prevalence of hypertensive retinopathy and associated risk factors. Next, it describes the diagnostic techniques and signs seen during an eye examination, such as arteriolar narrowing, tortuosity, and arteriovenous nicking. The classification of hypertensive retinopathy severity from Grade I to IV is then explained. The document concludes by discussing the pathophysiology, management through blood pressure control, and associated ocular conditions.
Hypertensive retinopathy

This document discusses hypertensive retinopathy, which refers to retinal vascular changes caused by high blood pressure. It notes that the prevalence of hypertensive retinopathy is approximately 15% among hypertensive patients without other vascular diseases. The key signs include arteriolar narrowing, arteriovenous nicking, and cotton wool spots. The pathogenesis involves initial vasoconstriction, then exudation and fluid leakage due to damaged blood vessels, and finally arteriolar sclerosis. Hypertensive choroidopathy and optic neuropathy can also occur in severe untreated cases and are characterized by lesions such as Elsching spots. Strict blood pressure control and regular eye screening are important for treatment and prevention of further vision loss
Hypertensive retinopathy

This lecture is based on medical students those are preparing for postgraduate degree namely FCPS/MS/MD/ any any subject coz hypertension is a systemic disease and by seeing the ocular fundus we can asses the general condition of blood vessels in major organ.
Hypertensive retinopathy

Hypertensive retinopathy is a very important topic for PG examinations of all types. Especially, the fundal changes are important; Keith and Wegner Grading is also a repeated topic in PG. This slide represents all information in a compressed fashion. Have fun!
Hypertensive retinopathy

Hypertensive retinopathy refers to changes in the retina and choroid that occur due to high blood pressure. There are three main factors that contribute to its pathogenesis: vasoconstriction, arteriosclerotic changes, and increased vascular permeability. Clinically, it presents as arteriolar narrowing, AV nicking, cotton wool spots, hemorrhages, and hard exudates. It can be chronic or malignant, with malignant seeing a more rapid progression. Treatment involves strict blood pressure control.
Macular hole

Macular hole is a defect in the macula involving its full thickness. It was first described in 1869. Idiopathic macular holes are the most common type and affect people over age 55. Staging of macular holes ranges from stage 1 to 4 based on size and pathology. Symptoms include decreased vision and metamorphopsia. Diagnosis involves examination, OCT, and sometimes FA. Treatment is usually vitrectomy surgery for stages 2-4 to relieve traction on the macula. Prognosis depends on pre-op vision and hole size/duration, with most patients gaining vision after surgery.
Age-Related Macular Degeneration

Age-related macular degeneration (AMD) is a leading cause of blindness that results from thickening of Bruch's membrane with age, interfering with metabolism in the retinal pigment epithelium (RPE) and photoreceptors. This causes deposits called drusen that damage the overlying RPE and underlying tissue. There are two forms: dry AMD involves gradual RPE and photoreceptor atrophy, while wet AMD features choroidal neovascularization that leaks fluid and blood, causing rapid vision loss if untreated. Risk factors include age, genetics, smoking, and diet.
Recommended
HYPERTENSIVE RETINOPATHY.pptx

This document summarizes hypertensive retinopathy, which occurs when retinal vessels are damaged due to elevated blood pressure. It discusses the types and clinical features of hypertensive retinopathy, including changes to retinal arteries and veins seen on examination. It also covers classifications of hypertensive retinopathy based on vessel changes and light reflexes. Risk factors, pathophysiology, and complications are described. Treatment involves controlling blood pressure through lifestyle changes and medication. Uncontrolled high blood pressure can lead to further eye and systemic damage.
Hypertensive retinopathy converted

This document discusses hypertensive retinopathy, which is caused by high blood pressure damaging the small blood vessels in the retina. It begins by covering the prevalence of hypertensive retinopathy and associated risk factors. Next, it describes the diagnostic techniques and signs seen during an eye examination, such as arteriolar narrowing, tortuosity, and arteriovenous nicking. The classification of hypertensive retinopathy severity from Grade I to IV is then explained. The document concludes by discussing the pathophysiology, management through blood pressure control, and associated ocular conditions.
Hypertensive retinopathy

This document discusses hypertensive retinopathy, which refers to retinal vascular changes caused by high blood pressure. It notes that the prevalence of hypertensive retinopathy is approximately 15% among hypertensive patients without other vascular diseases. The key signs include arteriolar narrowing, arteriovenous nicking, and cotton wool spots. The pathogenesis involves initial vasoconstriction, then exudation and fluid leakage due to damaged blood vessels, and finally arteriolar sclerosis. Hypertensive choroidopathy and optic neuropathy can also occur in severe untreated cases and are characterized by lesions such as Elsching spots. Strict blood pressure control and regular eye screening are important for treatment and prevention of further vision loss
Hypertensive retinopathy

This lecture is based on medical students those are preparing for postgraduate degree namely FCPS/MS/MD/ any any subject coz hypertension is a systemic disease and by seeing the ocular fundus we can asses the general condition of blood vessels in major organ.
Hypertensive retinopathy

Hypertensive retinopathy is a very important topic for PG examinations of all types. Especially, the fundal changes are important; Keith and Wegner Grading is also a repeated topic in PG. This slide represents all information in a compressed fashion. Have fun!
Hypertensive retinopathy

Hypertensive retinopathy refers to changes in the retina and choroid that occur due to high blood pressure. There are three main factors that contribute to its pathogenesis: vasoconstriction, arteriosclerotic changes, and increased vascular permeability. Clinically, it presents as arteriolar narrowing, AV nicking, cotton wool spots, hemorrhages, and hard exudates. It can be chronic or malignant, with malignant seeing a more rapid progression. Treatment involves strict blood pressure control.
Macular hole

Macular hole is a defect in the macula involving its full thickness. It was first described in 1869. Idiopathic macular holes are the most common type and affect people over age 55. Staging of macular holes ranges from stage 1 to 4 based on size and pathology. Symptoms include decreased vision and metamorphopsia. Diagnosis involves examination, OCT, and sometimes FA. Treatment is usually vitrectomy surgery for stages 2-4 to relieve traction on the macula. Prognosis depends on pre-op vision and hole size/duration, with most patients gaining vision after surgery.
Age-Related Macular Degeneration

Age-related macular degeneration (AMD) is a leading cause of blindness that results from thickening of Bruch's membrane with age, interfering with metabolism in the retinal pigment epithelium (RPE) and photoreceptors. This causes deposits called drusen that damage the overlying RPE and underlying tissue. There are two forms: dry AMD involves gradual RPE and photoreceptor atrophy, while wet AMD features choroidal neovascularization that leaks fluid and blood, causing rapid vision loss if untreated. Risk factors include age, genetics, smoking, and diet.
Retinal Vein Occlusion

Retinal vein occlusion (RVO) is an obstruction of the retinal venous system by thrombus formation and may involve the central, hemi-central or branch retinal vein.
The most common aetiological factor is compression by adjacent atherosclerotic retinal arteries.
Other possible causes are external compression or disease of the vein wall e.g. vasculitis.
Peripheral fundus & its disorders

Peripheral fundus & its disorders
Presented by Dr Rohit Rao
This document summarizes the key anatomical structures and pathologies of the peripheral retina. It describes the ora serrata, pars plana, vitreous base, dentate processes, meridional folds, and other peripheral features. It then discusses various degenerative conditions like lattice degeneration, retinoschisis, and pavingstone degeneration. Treatment options for retinal breaks including cryopexy and laser photocoagulation are also summarized.
Diabetic retinopathy

This document discusses diabetic retinopathy and its effects. It begins by noting the increasing prevalence of diabetes worldwide and that diabetes is a leading cause of blindness. It then describes the classification of diabetic retinopathy from mild non-proliferative to proliferative stages. Specific lesions associated with each stage are defined, including microaneurysms, hemorrhages, exudates, neovascularization, and retinal detachment. Risk factors for progression and visual loss from macular edema are also covered. The document emphasizes the importance of good blood sugar control in preventing and slowing the progression of diabetic retinopathy.
Central serous chorioretinopathy

Central serous chorioretinopathy (CSC) is characterized by a serous retinal detachment at the macula due to leakage from the choroidal vasculature beneath the retinal pigment epithelium (RPE). It commonly affects young and middle-aged males and has been associated with corticosteroid use, type A personality, and obstructive sleep apnea. Symptoms include blurred or decreased vision. Diagnosis is made based on imaging findings of serous retinal detachment, RPE changes, and evidence of choroidal vascular hyperpermeability. While typically self-limiting, treatments including anti-mineralocorticoid medications, laser photocoagulation, and photodynamic therapy may help shorten
Hypertension and ocular changes

hypertensive retinopathy, ghtn ocular changes, hypertensive choroidopathy, clinical features, pathognomonic signs, management
Structural and oct changes in diabetic retinopathy1

1) Diabetic retinopathy is caused by chronic hyperglycemia and results in progressive retinal dysfunction. Prolonged hyperglycemia damages blood vessels and the blood-retinal barrier.
2) OCT is useful for diagnosing and monitoring diabetic retinopathy. It provides high-resolution cross-sectional images of the retina to assess structural changes over time.
3) Features of diabetic retinopathy on OCT include macular edema, hard exudates, neurosensory detachment, and changes associated with proliferative retinopathy like tractional retinal detachment.
Anatomy of macula

The document discusses the anatomy, embryology, and function tests of the macula lutea. It describes the macula lutea as a 5.5mm circular area at the posterior pole of the retina that subserves central vision. It notes the macula's delayed development until 8 months gestation and specialization of the fovea which contains the highest concentration of cones. The document outlines various macular function tests used to evaluate macular diseases, including visual acuity, Amsler grid, microperimetry, and electroretinography. It provides details on the anatomy and cell layers of the fovea centralis and techniques for assessing macular integrity with tests like the Maddox rod.
Diabetic retinopathy

This document defines and describes diabetic retinopathy, its risk factors, pathogenesis, pathological lesions, classifications, and macular edema. Diabetic retinopathy is a progressive microangiopathy caused by breakdown of the blood-retinal barrier from damage to the small blood vessels of the retina. It can progress from non-proliferative to proliferative stages and is a leading cause of blindness if left untreated. The document outlines the stages and features used to classify diabetic retinopathy severity.
Keratoplasty

Dr. Karan Bhatia provides an overview of keratoplasty (corneal transplantation). There are different types including penetrating keratoplasty (replacing the full thickness of the diseased cornea), partial thickness lamellar keratoplasty, and rotational keratoplasty. Penetrating keratoplasty has been the standard procedure but carries risks. The history and techniques of penetrating keratoplasty are described in detail including pre-operative evaluation, donor cornea excision, recipient cornea trephination, suturing, and post-operative management. Potential complications are also reviewed. Lamellar keratoplasty is introduced as an alternative to penetrating keratoplasty to reduce risks
Diabetic and hypertensive retinopathy

This document summarizes diabetic retinopathy and hypertensive retinopathy. It discusses the pathogenesis, risk factors, classification, clinical features and treatment of diabetic retinopathy. It describes how diabetes can damage retinal blood vessels and lead to proliferative changes. It also outlines the screening guidelines for diabetic retinopathy. The document also summarizes hypertensive retinopathy, describing how high blood pressure can cause vascular changes in the retina. It discusses the different grades of hypertensive retinopathy and the aim of treatment to control high blood pressure.
CRAO and BRAO

This document discusses retinal artery occlusion. Key points:
- It typically affects people in their mid-60s and is more common in men.
- Embolism, usually from the heart or carotid artery, is the most common cause.
- Symptoms include sudden severe vision loss in one eye. On examination, the retina appears opaque and edematous with a narrowed artery.
- Visual loss is usually permanent if not treated within 90 minutes. Prompt diagnosis and treatment aimed at dissolving the clot are needed to preserve vision.
Fundus Fluoroscein Angiography

This document discusses fluorescein angiography (FA), a technique used to examine the circulation of the retina and choroid. FA involves injecting a fluorescent dye called sodium fluorescein and then taking photographs of the retina as the dye circulates through the eye. The dye is absorbed by the blood vessels and any leaks or blockages are visible. Precautions are taken and potential side effects explained to the patient. The sequence of FA images provides information about blood flow and any pathological conditions.
Diabetic retinopathy

This document discusses diabetic retinopathy, its causes, stages, treatments, and prevention. It is progressive retinal vessel dysfunction caused by long-term hyperglycemia. Key factors that contribute to its development include hypertension, hyperlipidemia, female sex, pregnancy, smoking, obesity, and poor metabolic control. Stages include non-proliferative and proliferative retinopathy. Treatments include anti-VEGF drugs, laser photocoagulation, vitrectomy, and strict control of blood sugar and blood pressure to prevent its progression.
Optic neuritis treatment trial

Optic neuritis is an inflammatory condition of the optic nerve that commonly affects people ages 20-50. It is more common in females. The document defines optic neuritis and discusses its various classifications, clinical features, diagnosis, relationship to multiple sclerosis, treatment, and prognosis. Treatment typically involves intravenous steroids like methylprednisolone to hasten recovery of vision, though long-term outcomes are generally good with many patients regaining near-normal vision. The presence of lesions on MRI increases the risk of developing multiple sclerosis within 10 years.
Hypertensive Retinopathy

Hypertensive Retinopathy (HTN-R) for undergraduate MBBS Students.
Covers the basics of Aetiology, pathophysiology, clinical features, Classification and management of HTN-R.
Also encompasses salient points for PGMEE
Cystoid macular oedema

This document discusses cystoid macular edema (CME), including its pathogenesis, etiology, associated ocular conditions, manifestations, diagnosis and testing. Specifically, it focuses on pseudophakic or Irvine-Gass syndrome CME, which can occur after cataract surgery. The summary discusses how CME results from fluid accumulation in the retina, its appearance on fluorescein angiography, risk factors for pseudophakic CME like vitreous loss during surgery, and how it is diagnosed using techniques like optical coherence tomography.
Cystoid macular oedema

Cystoid macular edema is a pathological accumulation of fluid in the macula that can be caused by conditions like diabetic retinopathy, retinal vein occlusions, or following cataract surgery. It is diagnosed using optical coherence tomography or fluorescein angiography and treated initially with anti-inflammatory eye drops, corticosteroid injections, or anti-VEGF drugs to reduce fluid accumulation. Laser therapy or vitrectomy may also be used in some cases to treat underlying causes like vitreomacular traction.
Diabetic Maculopathy

Diabetic maculopathy is a form of damage to the eye causing by diabetic macular oedema where fluids build up on the macula. It can be cured by laser surgeries.
Posterior uveitis by Dr. VIJAY PRATAP VIPSY

This document discusses various types of uveitis including classification, signs, symptoms, complications, investigations, and treatments. It covers infective causes like toxoplasmosis, tuberculosis, syphilis, and fungal infections. It also discusses immune-mediated uveitis associated with conditions like VKH syndrome, Behcet's disease, and sarcoidosis. Intermediate uveitis is characterized by inflammation of the pars plana, peripheral retina, and choroid. Posterior uveitis involves the retina and choroid and can be caused by infections, autoimmune diseases, or unknown etiologies.
Ocular Manifestations of Systemic Disease

This document discusses various systemic diseases that can manifest ocularly and be detected on eye examination. It covers 10 categories of disease including congenital, traumatic, vascular, neoplastic, autoimmune, idiopathic, infectious, metabolic/endocrine, and drugs/toxins. For each category, specific diseases are described along with their characteristic ocular signs and symptoms. The importance of comprehensive eye exams for evaluating systemic health is emphasized.
Hypertension

Hypertension is defined as a sustained blood pressure greater than 140/90 mm Hg. It is a major risk factor for atherosclerosis and cardiovascular disease. The pathogenesis of essential hypertension involves genetic and environmental factors that alter cardiac output and peripheral resistance. Primary defects include renal sodium retention and vasoconstriction/hypertrophy. Secondary causes include endocrine, renal, and neurological conditions.
BloodVessels.ppt

The document discusses hypertension (high blood pressure) and its pathogenesis and complications. It provides details on:
1) The classification and diagnosis of hypertension according to guidelines.
2) The types of hypertension including essential and secondary causes. Secondary causes include renal, endocrine, cardiovascular and neurological factors.
3) The role of the endothelium and kidneys in regulating blood pressure. Dysfunction can lead to hypertension.
4) Complications of both benign and malignant hypertension affecting organs like the brain, heart, kidneys, and vasculature.
More Related Content
What's hot
Retinal Vein Occlusion

Retinal vein occlusion (RVO) is an obstruction of the retinal venous system by thrombus formation and may involve the central, hemi-central or branch retinal vein.
The most common aetiological factor is compression by adjacent atherosclerotic retinal arteries.
Other possible causes are external compression or disease of the vein wall e.g. vasculitis.
Peripheral fundus & its disorders

Peripheral fundus & its disorders
Presented by Dr Rohit Rao
This document summarizes the key anatomical structures and pathologies of the peripheral retina. It describes the ora serrata, pars plana, vitreous base, dentate processes, meridional folds, and other peripheral features. It then discusses various degenerative conditions like lattice degeneration, retinoschisis, and pavingstone degeneration. Treatment options for retinal breaks including cryopexy and laser photocoagulation are also summarized.
Diabetic retinopathy

This document discusses diabetic retinopathy and its effects. It begins by noting the increasing prevalence of diabetes worldwide and that diabetes is a leading cause of blindness. It then describes the classification of diabetic retinopathy from mild non-proliferative to proliferative stages. Specific lesions associated with each stage are defined, including microaneurysms, hemorrhages, exudates, neovascularization, and retinal detachment. Risk factors for progression and visual loss from macular edema are also covered. The document emphasizes the importance of good blood sugar control in preventing and slowing the progression of diabetic retinopathy.
Central serous chorioretinopathy

Central serous chorioretinopathy (CSC) is characterized by a serous retinal detachment at the macula due to leakage from the choroidal vasculature beneath the retinal pigment epithelium (RPE). It commonly affects young and middle-aged males and has been associated with corticosteroid use, type A personality, and obstructive sleep apnea. Symptoms include blurred or decreased vision. Diagnosis is made based on imaging findings of serous retinal detachment, RPE changes, and evidence of choroidal vascular hyperpermeability. While typically self-limiting, treatments including anti-mineralocorticoid medications, laser photocoagulation, and photodynamic therapy may help shorten
Hypertension and ocular changes

hypertensive retinopathy, ghtn ocular changes, hypertensive choroidopathy, clinical features, pathognomonic signs, management
Structural and oct changes in diabetic retinopathy1

1) Diabetic retinopathy is caused by chronic hyperglycemia and results in progressive retinal dysfunction. Prolonged hyperglycemia damages blood vessels and the blood-retinal barrier.
2) OCT is useful for diagnosing and monitoring diabetic retinopathy. It provides high-resolution cross-sectional images of the retina to assess structural changes over time.
3) Features of diabetic retinopathy on OCT include macular edema, hard exudates, neurosensory detachment, and changes associated with proliferative retinopathy like tractional retinal detachment.
Anatomy of macula

The document discusses the anatomy, embryology, and function tests of the macula lutea. It describes the macula lutea as a 5.5mm circular area at the posterior pole of the retina that subserves central vision. It notes the macula's delayed development until 8 months gestation and specialization of the fovea which contains the highest concentration of cones. The document outlines various macular function tests used to evaluate macular diseases, including visual acuity, Amsler grid, microperimetry, and electroretinography. It provides details on the anatomy and cell layers of the fovea centralis and techniques for assessing macular integrity with tests like the Maddox rod.
Diabetic retinopathy

This document defines and describes diabetic retinopathy, its risk factors, pathogenesis, pathological lesions, classifications, and macular edema. Diabetic retinopathy is a progressive microangiopathy caused by breakdown of the blood-retinal barrier from damage to the small blood vessels of the retina. It can progress from non-proliferative to proliferative stages and is a leading cause of blindness if left untreated. The document outlines the stages and features used to classify diabetic retinopathy severity.
Keratoplasty

Dr. Karan Bhatia provides an overview of keratoplasty (corneal transplantation). There are different types including penetrating keratoplasty (replacing the full thickness of the diseased cornea), partial thickness lamellar keratoplasty, and rotational keratoplasty. Penetrating keratoplasty has been the standard procedure but carries risks. The history and techniques of penetrating keratoplasty are described in detail including pre-operative evaluation, donor cornea excision, recipient cornea trephination, suturing, and post-operative management. Potential complications are also reviewed. Lamellar keratoplasty is introduced as an alternative to penetrating keratoplasty to reduce risks
Diabetic and hypertensive retinopathy

This document summarizes diabetic retinopathy and hypertensive retinopathy. It discusses the pathogenesis, risk factors, classification, clinical features and treatment of diabetic retinopathy. It describes how diabetes can damage retinal blood vessels and lead to proliferative changes. It also outlines the screening guidelines for diabetic retinopathy. The document also summarizes hypertensive retinopathy, describing how high blood pressure can cause vascular changes in the retina. It discusses the different grades of hypertensive retinopathy and the aim of treatment to control high blood pressure.
CRAO and BRAO

This document discusses retinal artery occlusion. Key points:
- It typically affects people in their mid-60s and is more common in men.
- Embolism, usually from the heart or carotid artery, is the most common cause.
- Symptoms include sudden severe vision loss in one eye. On examination, the retina appears opaque and edematous with a narrowed artery.
- Visual loss is usually permanent if not treated within 90 minutes. Prompt diagnosis and treatment aimed at dissolving the clot are needed to preserve vision.
Fundus Fluoroscein Angiography

This document discusses fluorescein angiography (FA), a technique used to examine the circulation of the retina and choroid. FA involves injecting a fluorescent dye called sodium fluorescein and then taking photographs of the retina as the dye circulates through the eye. The dye is absorbed by the blood vessels and any leaks or blockages are visible. Precautions are taken and potential side effects explained to the patient. The sequence of FA images provides information about blood flow and any pathological conditions.
Diabetic retinopathy

This document discusses diabetic retinopathy, its causes, stages, treatments, and prevention. It is progressive retinal vessel dysfunction caused by long-term hyperglycemia. Key factors that contribute to its development include hypertension, hyperlipidemia, female sex, pregnancy, smoking, obesity, and poor metabolic control. Stages include non-proliferative and proliferative retinopathy. Treatments include anti-VEGF drugs, laser photocoagulation, vitrectomy, and strict control of blood sugar and blood pressure to prevent its progression.
Optic neuritis treatment trial

Optic neuritis is an inflammatory condition of the optic nerve that commonly affects people ages 20-50. It is more common in females. The document defines optic neuritis and discusses its various classifications, clinical features, diagnosis, relationship to multiple sclerosis, treatment, and prognosis. Treatment typically involves intravenous steroids like methylprednisolone to hasten recovery of vision, though long-term outcomes are generally good with many patients regaining near-normal vision. The presence of lesions on MRI increases the risk of developing multiple sclerosis within 10 years.
Hypertensive Retinopathy

Hypertensive Retinopathy (HTN-R) for undergraduate MBBS Students.
Covers the basics of Aetiology, pathophysiology, clinical features, Classification and management of HTN-R.
Also encompasses salient points for PGMEE
Cystoid macular oedema

This document discusses cystoid macular edema (CME), including its pathogenesis, etiology, associated ocular conditions, manifestations, diagnosis and testing. Specifically, it focuses on pseudophakic or Irvine-Gass syndrome CME, which can occur after cataract surgery. The summary discusses how CME results from fluid accumulation in the retina, its appearance on fluorescein angiography, risk factors for pseudophakic CME like vitreous loss during surgery, and how it is diagnosed using techniques like optical coherence tomography.
Cystoid macular oedema

Cystoid macular edema is a pathological accumulation of fluid in the macula that can be caused by conditions like diabetic retinopathy, retinal vein occlusions, or following cataract surgery. It is diagnosed using optical coherence tomography or fluorescein angiography and treated initially with anti-inflammatory eye drops, corticosteroid injections, or anti-VEGF drugs to reduce fluid accumulation. Laser therapy or vitrectomy may also be used in some cases to treat underlying causes like vitreomacular traction.
Diabetic Maculopathy

Diabetic maculopathy is a form of damage to the eye causing by diabetic macular oedema where fluids build up on the macula. It can be cured by laser surgeries.
Posterior uveitis by Dr. VIJAY PRATAP VIPSY

This document discusses various types of uveitis including classification, signs, symptoms, complications, investigations, and treatments. It covers infective causes like toxoplasmosis, tuberculosis, syphilis, and fungal infections. It also discusses immune-mediated uveitis associated with conditions like VKH syndrome, Behcet's disease, and sarcoidosis. Intermediate uveitis is characterized by inflammation of the pars plana, peripheral retina, and choroid. Posterior uveitis involves the retina and choroid and can be caused by infections, autoimmune diseases, or unknown etiologies.
Ocular Manifestations of Systemic Disease

This document discusses various systemic diseases that can manifest ocularly and be detected on eye examination. It covers 10 categories of disease including congenital, traumatic, vascular, neoplastic, autoimmune, idiopathic, infectious, metabolic/endocrine, and drugs/toxins. For each category, specific diseases are described along with their characteristic ocular signs and symptoms. The importance of comprehensive eye exams for evaluating systemic health is emphasized.
What's hot (20)
Structural and oct changes in diabetic retinopathy1

Structural and oct changes in diabetic retinopathy1
Similar to HYPERTENSIVE RETINOPATHY - DR ARNAV SAROYA
Hypertension

Hypertension is defined as a sustained blood pressure greater than 140/90 mm Hg. It is a major risk factor for atherosclerosis and cardiovascular disease. The pathogenesis of essential hypertension involves genetic and environmental factors that alter cardiac output and peripheral resistance. Primary defects include renal sodium retention and vasoconstriction/hypertrophy. Secondary causes include endocrine, renal, and neurological conditions.
BloodVessels.ppt

The document discusses hypertension (high blood pressure) and its pathogenesis and complications. It provides details on:
1) The classification and diagnosis of hypertension according to guidelines.
2) The types of hypertension including essential and secondary causes. Secondary causes include renal, endocrine, cardiovascular and neurological factors.
3) The role of the endothelium and kidneys in regulating blood pressure. Dysfunction can lead to hypertension.
4) Complications of both benign and malignant hypertension affecting organs like the brain, heart, kidneys, and vasculature.
General medicine update for every doctor hypertension

Hypertension is a leading global cause of death and disability. It doubles the risk of cardiovascular diseases like heart disease and stroke. While treating hypertension reduces these risks, many hypertensive patients remain untreated or inadequately treated. Hypertension affects the eyes by damaging blood vessels in the retina, optic nerve, and choroid which can lead to vision loss if uncontrolled. Doctors are advised to gradually lower blood pressure using recommended first-line drug classes and monitor for associated organ damage.
18.kidney in pregnancy, HTN.pptx

This document discusses hypertension (high blood pressure). It defines hypertension according to the JNC 7 classification and discusses its causes, which include both essential (primary) hypertension in 90-95% of cases as well as secondary hypertension due to factors like kidney, endocrine, cardiovascular, or neurological disease. The document outlines how hypertension increases risk for diseases like heart failure, stroke, and kidney disease. It also discusses malignant hypertension, which involves very high blood pressures that can lead to rapid organ damage and death if not treated.
Hypertension

This document discusses hypertension (high blood pressure). It defines hypertension and lists risk factors such as obesity, sodium intake, stress, and lack of physical activity. It describes mechanisms of hypertension including increased intravascular volume, the renin-angiotensin system, the sympathetic nervous system, vascular changes, and immune/inflammatory factors. Secondary causes of hypertension like kidney disease and primary aldosteronism are explained. Treatment involves lifestyle modifications and drug therapy. Blood pressure goals of therapy and the distinction between hypertensive emergencies and urgencies are also summarized.
HYPERTENSION Shoukat Sir .pptx

Hypertension is a major risk factor for cardiovascular disease. This document discusses the epidemiology, pathophysiology, classification, and treatment of hypertension. Regarding pathophysiology, factors discussed include intravascular volume, the autonomic nervous system, the renin-angiotensin-aldosterone system, vascular mechanisms, and immune/inflammatory mechanisms. Treatment involves lifestyle modifications and medications such as diuretics, ACE inhibitors, ARBs, calcium channel blockers, and aldosterone antagonists.
Hypertensive Retinopathy

Hypertension can damage the eye and lead to hypertensive retinopathy. Chronic high blood pressure causes gradual changes to the retinal blood vessels including arteriolar narrowing, nicking at arteriovenous crossings, and changes to the light reflex seen in the vessels. Malignant or acute hypertension can additionally cause retinal hemorrhages, cotton wool spots, and exudates due to damage to the small blood vessels in the retina. Strict control of blood pressure is important to prevent further eye damage and risk of other end-organ complications.
Hypertension

The document discusses hypertension (high blood pressure), including its definition, causes, risk factors, complications, diagnosis, and management. Some key points:
- Hypertension is defined as a systolic blood pressure over 140 mmHg or diastolic over 90 mmHg. It affects over 20% of adults in Bangladesh.
- It has various causes like genetics, obesity, sodium intake, stress, and can be essential (90-95% of cases) or secondary to other medical conditions.
- If left untreated, it can damage organs like the heart, brain, kidneys, and eyes, leading to complications like heart attack, stroke, kidney disease, and vision loss.
- Diagnosis involves
HYPERTENSION

Hypertension, or high blood pressure, is a common health problem that typically has no symptoms until late stages. It contributes to diseases like heart disease and stroke. The document defines hypertension as a diastolic pressure over 90 mm Hg or systolic over 140 mm Hg. While the causes are unknown for most people (essential hypertension), it can be secondary to other conditions. Complications involve damage to the heart, blood vessels, brain, kidneys and eyes. Evaluation of patients with hypertension aims to identify risk factors, secondary causes, and evidence of organ damage.
Htn

This document discusses hypertension (high blood pressure) and its mechanisms, causes, and effects. It defines hypertension and explains that it doubles the risk of cardiovascular diseases by increasing cardiac output and peripheral resistance. Primary causes of hypertension include increased vascular volume from sodium intake, activation of the sympathetic nervous system, and the renin-angiotensin-aldosterone system. Secondary causes include renal disease, obesity, sleep apnea, pheochromocytoma, Cushing's syndrome, and others. The document outlines approaches to evaluating patients for hypertension through history, physical exam, and laboratory tests to identify underlying conditions and target organ damage.
Samir Rafla Principles of Cardiology pages 112 to end revised

Hypertension is a major risk factor for cardiovascular disease that accelerates atherosclerosis and increases the workload of the heart. This puts hypertensive patients at risk for conditions like heart attack, stroke, renal failure, and heart failure. The document discusses evaluation and management of hypertension, including classification of blood pressure levels and investigation of secondary causes. Key tests involve assessing for end organ damage to the eyes, heart, kidneys, and ruling out secondary causes through tests like renal ultrasound and 24-hour urine collections. Treatment involves lifestyle modifications and medications, with surgery sometimes needed for treatable secondary causes.
Life threatening side effects of Psychotropics

This document summarizes several life-threatening side effects of psychotropic medications, focusing on antipsychotics. It discusses QT prolongation which can lead to fatal arrhythmias. It also discusses diabetic ketoacidosis, drug-induced SIADH which can cause hyponatremia, increased risk of pneumonia, and serious hematological and cardiovascular side effects of clozapine including agranulocytosis, thromboembolism, myocarditis, and cardiomyopathy. Monitoring and management of these side effects is important for patient safety.
Hypertensive Retinopathy.pptx

Hypertension can cause hypertensive retinopathy by damaging blood vessels in the retina. It progresses through vasoconstrictive, sclerotic, and exudative phases causing signs like hemorrhages, exudates, and cotton wool spots. Retinal imaging can diagnose and monitor the condition. Treatment focuses on controlling blood pressure through medication and lifestyle changes to prevent further vision loss and systemic complications. Patients with severe retinopathy have increased risk of other vascular issues and require close monitoring.
CVS pathology -4 Hypertension (HTN) 2019, sufia husain

The document discusses hypertension (high blood pressure), including its definition, risk factors, causes, classification, pathogenesis, effects on organs, and complications. It notes that hypertension has no symptoms in early stages but can damage organs over time, leading to heart disease, stroke, kidney failure, and retinal damage. Uncontrolled high blood pressure is also defined as malignant hypertension, which can cause rapid organ damage within years.
Chapter 6 Endocrine disorders by Dr. Derejepdf

Chronic kidney disease (CKD) is common in patients with diabetes and is diagnosed through elevated albuminuria and reduced estimated glomerular filtration rate (eGFR). CKD attributed to diabetes occurs in 20-40% of patients and can progress to end-stage renal disease requiring dialysis. Diabetic retinopathy, caused by chronic hyperglycemia, is the most common cause of blindness and is assessed through eye exams. Neuropathy is assessed through history and examination of sensation, with annual 10-g monofilament testing to check for high-risk feet. Foot care includes inspection, assessment of deformities and pulses, and referral for ongoing surveillance in high-risk patients to prevent ulcers and amputations.
Hypertension

This document discusses hypertension (high blood pressure), including its causes, symptoms, diagnosis, and treatment. It defines hypertension and describes its classification. It also outlines lifestyle modifications and medications that are used to treat hypertension. The goals of treatment are to lower blood pressure and prevent target organ damage to the heart, brain, kidneys and eyes. Nursing care focuses on educating patients, monitoring for side effects, ensuring compliance with treatment, and evaluating treatment effectiveness.
Hypertension

Hypertension, or high blood pressure, is defined as blood pressure above 140/90 mmHg. It can be classified into stages based on systolic and diastolic blood pressure readings. The majority of cases are primary or essential hypertension, while a small percentage are secondary to other conditions. Target organ damage to the heart, brain, kidneys and eyes can occur if hypertension is not controlled. Lifestyle modifications and medications are used to treat and manage hypertension. Nursing care involves educating patients, monitoring for complications, and promoting treatment adherence.
Hypertension Emergencies and their managementpptx

This Presentation talks about Hyprtension, the mode of presentation of hypertensive crisis and the effective management of hypertensive crisis to prevent case fatalities.
11.HTN.pptx

This document provides an overview of hypertension including its definition, classification, epidemiology, pathophysiology, symptoms, complications, diagnosis, and treatment. Some key points:
- Hypertension is defined as blood pressure above 140/90 mmHg and increases risk of damage to organs like the brain, heart, kidneys, and eyes. It often has no symptoms.
- It becomes more common with age and is a major risk factor for heart attacks, strokes, and kidney failure.
- Treatment involves lifestyle changes like diet, exercise, and reducing sodium as well as medications like diuretics, ACE inhibitors, ARBs, calcium channel blockers, and beta blockers.
- Goals of
Similar to HYPERTENSIVE RETINOPATHY - DR ARNAV SAROYA (20)
General medicine update for every doctor hypertension

General medicine update for every doctor hypertension
Samir Rafla Principles of Cardiology pages 112 to end revised

Samir Rafla Principles of Cardiology pages 112 to end revised
CVS pathology -4 Hypertension (HTN) 2019, sufia husain

CVS pathology -4 Hypertension (HTN) 2019, sufia husain
HYPERTENSION/high blood pressure- a lecture-1.pptx

HYPERTENSION/high blood pressure- a lecture-1.pptx
Recently uploaded
Cell Therapy Expansion and Challenges in Autoimmune Disease

There is increasing confidence that cell therapies will soon play a role in the treatment of autoimmune disorders, but the extent of this impact remains to be seen. Early readouts on autologous CAR-Ts in lupus are encouraging, but manufacturing and cost limitations are likely to restrict access to highly refractory patients. Allogeneic CAR-Ts have the potential to broaden access to earlier lines of treatment due to their inherent cost benefits, however they will need to demonstrate comparable or improved efficacy to established modalities.
In addition to infrastructure and capacity constraints, CAR-Ts face a very different risk-benefit dynamic in autoimmune compared to oncology, highlighting the need for tolerable therapies with low adverse event risk. CAR-NK and Treg-based therapies are also being developed in certain autoimmune disorders and may demonstrate favorable safety profiles. Several novel non-cell therapies such as bispecific antibodies, nanobodies, and RNAi drugs, may also offer future alternative competitive solutions with variable value propositions.
Widespread adoption of cell therapies will not only require strong efficacy and safety data, but also adapted pricing and access strategies. At oncology-based price points, CAR-Ts are unlikely to achieve broad market access in autoimmune disorders, with eligible patient populations that are potentially orders of magnitude greater than the number of currently addressable cancer patients. Developers have made strides towards reducing cell therapy COGS while improving manufacturing efficiency, but payors will inevitably restrict access until more sustainable pricing is achieved.
Despite these headwinds, industry leaders and investors remain confident that cell therapies are poised to address significant unmet need in patients suffering from autoimmune disorders. However, the extent of this impact on the treatment landscape remains to be seen, as the industry rapidly approaches an inflection point.
Clinic ^%[+27633867063*Abortion Pills For Sale In Tembisa Central

Clinic ^%[+27633867063*Abortion Pills For Sale In Tembisa Central Clinic ^%[+27633867063*Abortion Pills For Sale In Tembisa CentralClinic ^%[+27633867063*Abortion Pills For Sale In Tembisa CentralClinic ^%[+27633867063*Abortion Pills For Sale In Tembisa CentralClinic ^%[+27633867063*Abortion Pills For Sale In Tembisa Central
Ketone bodies and metabolism-biochemistry

This slide consists of all the topics of ketone . This can be used for exam purpose for writing about Diabetic keto acidosis etc . Thank you
Hemodialysis: Chapter 4, Dialysate Circuit - Dr.Gawad

- Video recording of this lecture in English language: https://youtu.be/kqbnxVAZs-0
- Video recording of this lecture in Arabic language: https://youtu.be/SINlygW1Mpc
- Link to download the book free: https://nephrotube.blogspot.com/p/nephrotube-nephrology-books.html
- Link to NephroTube website: www.NephroTube.com
- Link to NephroTube social media accounts: https://nephrotube.blogspot.com/p/join-nephrotube-on-social-media.html
TEST BANK For An Introduction to Brain and Behavior, 7th Edition by Bryan Kol...

TEST BANK For An Introduction to Brain and Behavior, 7th Edition by Bryan Kol...rightmanforbloodline
TEST BANK For An Introduction to Brain and Behavior, 7th Edition by Bryan Kolb, Ian Q. Whishaw, Verified Chapters 1 - 16, Complete Newest Versio
TEST BANK For An Introduction to Brain and Behavior, 7th Edition by Bryan Kolb, Ian Q. Whishaw, Verified Chapters 1 - 16, Complete Newest Version
TEST BANK For An Introduction to Brain and Behavior, 7th Edition by Bryan Kolb, Ian Q. Whishaw, Verified Chapters 1 - 16, Complete Newest Versionshare - Lions, tigers, AI and health misinformation, oh my!.pptx

• Pitfalls and pivots needed to use AI effectively in public health
• Evidence-based strategies to address health misinformation effectively
• Building trust with communities online and offline
• Equipping health professionals to address questions, concerns and health misinformation
• Assessing risk and mitigating harm from adverse health narratives in communities, health workforce and health system
Does Over-Masturbation Contribute to Chronic Prostatitis.pptx

In some case, your chronic prostatitis may be related to over-masturbation. Generally, natural medicine Diuretic and Anti-inflammatory Pill can help mee get a cure.
8 Surprising Reasons To Meditate 40 Minutes A Day That Can Change Your Life.pptx

8 Surprising Reasons To Meditate 40 Minutes A Day That Can Change Your Life.pptxHolistified Wellness
We’re talking about Vedic Meditation, a form of meditation that has been around for at least 5,000 years. Back then, the people who lived in the Indus Valley, now known as India and Pakistan, practised meditation as a fundamental part of daily life. This knowledge that has given us yoga and Ayurveda, was known as Veda, hence the name Vedic. And though there are some written records, the practice has been passed down verbally from generation to generation.Promoting Wellbeing - Applied Social Psychology - Psychology SuperNotes

A proprietary approach developed by bringing together the best of learning theories from Psychology, design principles from the world of visualization, and pedagogical methods from over a decade of training experience, that enables you to: Learn better, faster!
Adhd Medication Shortage Uk - trinexpharmacy.com

The UK is currently facing a Adhd Medication Shortage Uk, which has left many patients and their families grappling with uncertainty and frustration. ADHD, or Attention Deficit Hyperactivity Disorder, is a chronic condition that requires consistent medication to manage effectively. This shortage has highlighted the critical role these medications play in the daily lives of those affected by ADHD. Contact : +1 (747) 209 – 3649 E-mail : sales@trinexpharmacy.com
Part II - Body Grief: Losing parts of ourselves and our identity before, duri...

Learn about body grief and ways to cope with it. We will also explore methods to heal from this challenging experience.
Integrating Ayurveda into Parkinson’s Management: A Holistic Approach

Explore the benefits of combining Ayurveda with conventional Parkinson's treatments. Learn how a holistic approach can manage symptoms, enhance well-being, and balance body energies. Discover the steps to safely integrate Ayurvedic practices into your Parkinson’s care plan, including expert guidance on diet, herbal remedies, and lifestyle modifications.
The Best Ayurvedic Antacid Tablets in India

Treat the symptoms of indigestion, heartburn and stomach reflux with the 10 Best Ayurvedic Antacid Tablets in India.
A Classical Text Review on Basavarajeeyam

Basavarajeeyam is a Sreshta Sangraha grantha (Compiled book ), written by Neelkanta kotturu Basavaraja Virachita. It contains 25 Prakaranas, First 24 Chapters related to Rogas& 25th to Rasadravyas.
Recently uploaded (20)
Cell Therapy Expansion and Challenges in Autoimmune Disease

Cell Therapy Expansion and Challenges in Autoimmune Disease
Clinic ^%[+27633867063*Abortion Pills For Sale In Tembisa Central

Clinic ^%[+27633867063*Abortion Pills For Sale In Tembisa Central
Hemodialysis: Chapter 4, Dialysate Circuit - Dr.Gawad

Hemodialysis: Chapter 4, Dialysate Circuit - Dr.Gawad
TEST BANK For An Introduction to Brain and Behavior, 7th Edition by Bryan Kol...

TEST BANK For An Introduction to Brain and Behavior, 7th Edition by Bryan Kol...
share - Lions, tigers, AI and health misinformation, oh my!.pptx

share - Lions, tigers, AI and health misinformation, oh my!.pptx
Does Over-Masturbation Contribute to Chronic Prostatitis.pptx

Does Over-Masturbation Contribute to Chronic Prostatitis.pptx
8 Surprising Reasons To Meditate 40 Minutes A Day That Can Change Your Life.pptx

8 Surprising Reasons To Meditate 40 Minutes A Day That Can Change Your Life.pptx
Promoting Wellbeing - Applied Social Psychology - Psychology SuperNotes

Promoting Wellbeing - Applied Social Psychology - Psychology SuperNotes
Part II - Body Grief: Losing parts of ourselves and our identity before, duri...

Part II - Body Grief: Losing parts of ourselves and our identity before, duri...
Integrating Ayurveda into Parkinson’s Management: A Holistic Approach

Integrating Ayurveda into Parkinson’s Management: A Holistic Approach
Muscles of Mastication by Dr. Rabia Inam Gandapore.pptx

Muscles of Mastication by Dr. Rabia Inam Gandapore.pptx
HYPERTENSIVE RETINOPATHY - DR ARNAV SAROYA
- 5. 1. Genetic factors can also play a role with certain genotypes associated with an increased risk of hypertensive retinopathy. 2. Smoking is considered to have a strong association with severe or malignant hypertensive retinopathy . 3. Renal dysfunction (persistent microalbuminuria and low creatinine clearance) in patients has shown to be a marker for hypertensive retinopathy and end-organ damage. 4. Arteriosclerotic changes of hypertensive retinopathy are caused by chronically elevated blood pressure, defined as systolic greater than 140 mmHg and diastolic greater than 90 mmHg. Hypertension is usually essential and not secondary to another disease process. ETIOLOGY
- 6. •Retinal blood vessels have distinct features, which differentiate them from other blood vessels • The absence of sympathetic nerve supply • Autoregulation of blood flow • Presence of blood-retinal barrier •Thus, an increase in blood pressure (BP) is transferred directly to the vessels which initially constrict. • However, a further increase in BP overcomes this compensatory tone and damage to the muscle layer and endothelium ensues.
- 18. Bonnet’s sign: Banking of the retinal vein distal to the AV crossing
- 19. Decrease in the arteriovenous ratio to 1:3 ( the normal ratio is 2:3).
- 34. Collaterals.
- 44. •Siegrist's streak: RPE hyperplasia over choroidal infarcts
- 65. COMPLICATIONS • Retinal artery occlusion • Retinal vein occlusion • Macro aneurysm of retinal arteriole • Diabetic retinopathy (DR): Both hypertensive retinopathy and DR together in a patient is called as mixed retinopathy. HTN is also known to be a major risk factor for the progression of DR. • Anterior ischemic optic neuropathy • Age-related macular degeneration • Glaucoma • Retinal arteriolar emboli • Epiretinal membrane formation • Cystoid macular edema
- 66. MANAGEMENT • Systemic hypertension should be controlled as a primary measure for Hypertensive retinopathy. • Change in lifestyle with reduction of general risk factors (salt restriction, avoidance of tobacco) help in controlling hypertension. • Drugs may be used from groups like: • – Diuretics. • – Beta blockers. • – Angiotensin converting enzyme inhibitors. • – Calcium channel blockers. • – Angiotensin receptor antagonists.
- 67. •Patients with severe hypertensive retinopathy are at increased risk of coronary artery disease, stroke or peripheral vascular disease. Arteriosclerotic changes increases the risk of retinal macroaneurysms, retinal artery or vein occlusion. Visual acuity may be reduced due to involvement of optic nerve and macula. •Hypertensive retinopathy with vision threatening complication: Vision threatening complications like retinal oedema may be treated with laser therapy or intravitreal injection of vascular endothelial growth factor (VEGF) drugs.
Editor's Notes
- caused by chronically elevated blood pressure, defined as systolic greater than 140 mmHg and diastolic greater than 90 mmHg
- Severity and duration of htn are directly related to incidence of htn retinopathy .
- In a study by kabedi et al – htn retino in 83.6 % out of total hypertensive patients and chronic kidney disease – most significant factor to predict severe htn ret. Malignant htn – above 180/120
- SECONDARY HTN – bycondtns affecting the kidneys , arteries , heart or endocrine system. Secondary hypertension may be caused by an underlying disease such as: – Primary hyperaldosteronism. – Cushing’s syndrome. – Phaeochromocytoma. – Renal vascular or renal parenchymal disease. – Coarctation of aorta. – Hyperthyroidism. – Hyperparathyroidism
- acute effects of systemic arterial hypertension are a result of vasospasm to autoregulate perfusion[2]. The chronic effects of hypertension are caused by arteriosclerosis and predispose patients to visual loss from vascular occlusions or macroaneurysms