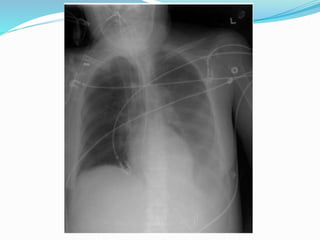
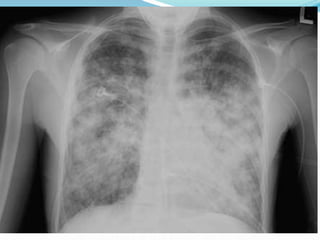
Hospital-acquired pneumonia (HAP) affects approximately 1% of admissions, increasing morbidity, length of stay, and mortality rates, which can range from 20% to 50%. Risk factors include age over 70, severe comorbidities, and poor infection control practices. Diagnosis involves various tests such as chest X-rays and cultures, with treatment varying based on the onset time of the infection and potential pathogens involved.