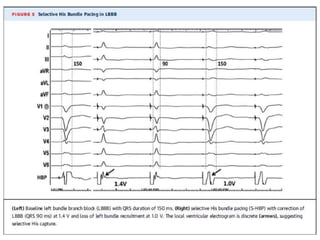
This document discusses His bundle pacing (HBP), which aims to engage the normal conduction system through the His-Purkinje network. HBP may provide physiological stimulation compared to right ventricular pacing. The document covers anatomy and physiology of the His bundle, techniques for selective vs. nonselective HBP, indications including AV node ablation and cardiac resynchronization, long-term outcomes, and challenges such as high capture thresholds and lead revisions. While HBP shows promise, further studies are needed to validate its long-term safety, reliability and impact on arrhythmias.