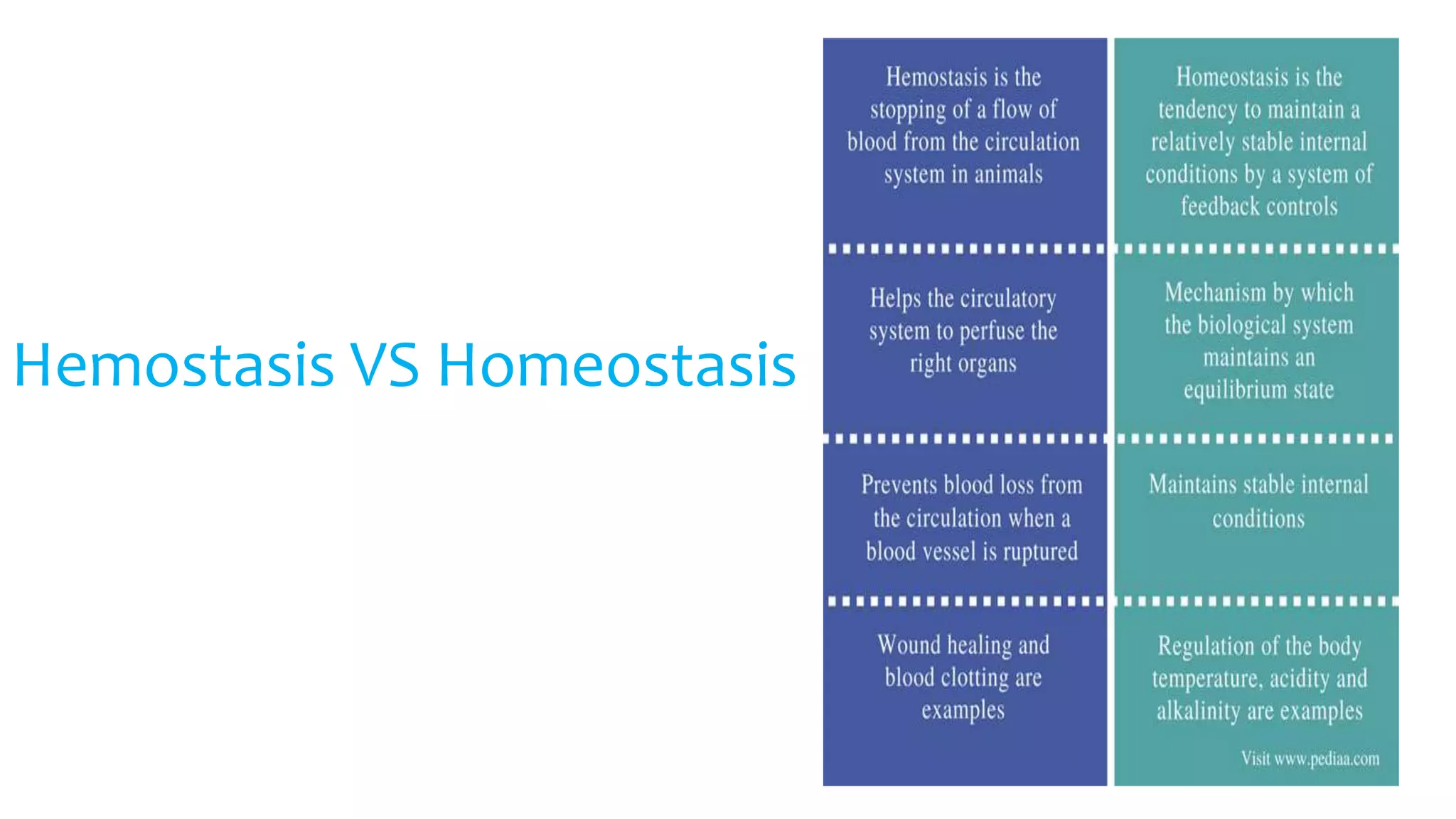
Hemostasis is the process by which bleeding is stopped. It involves three main mechanisms:
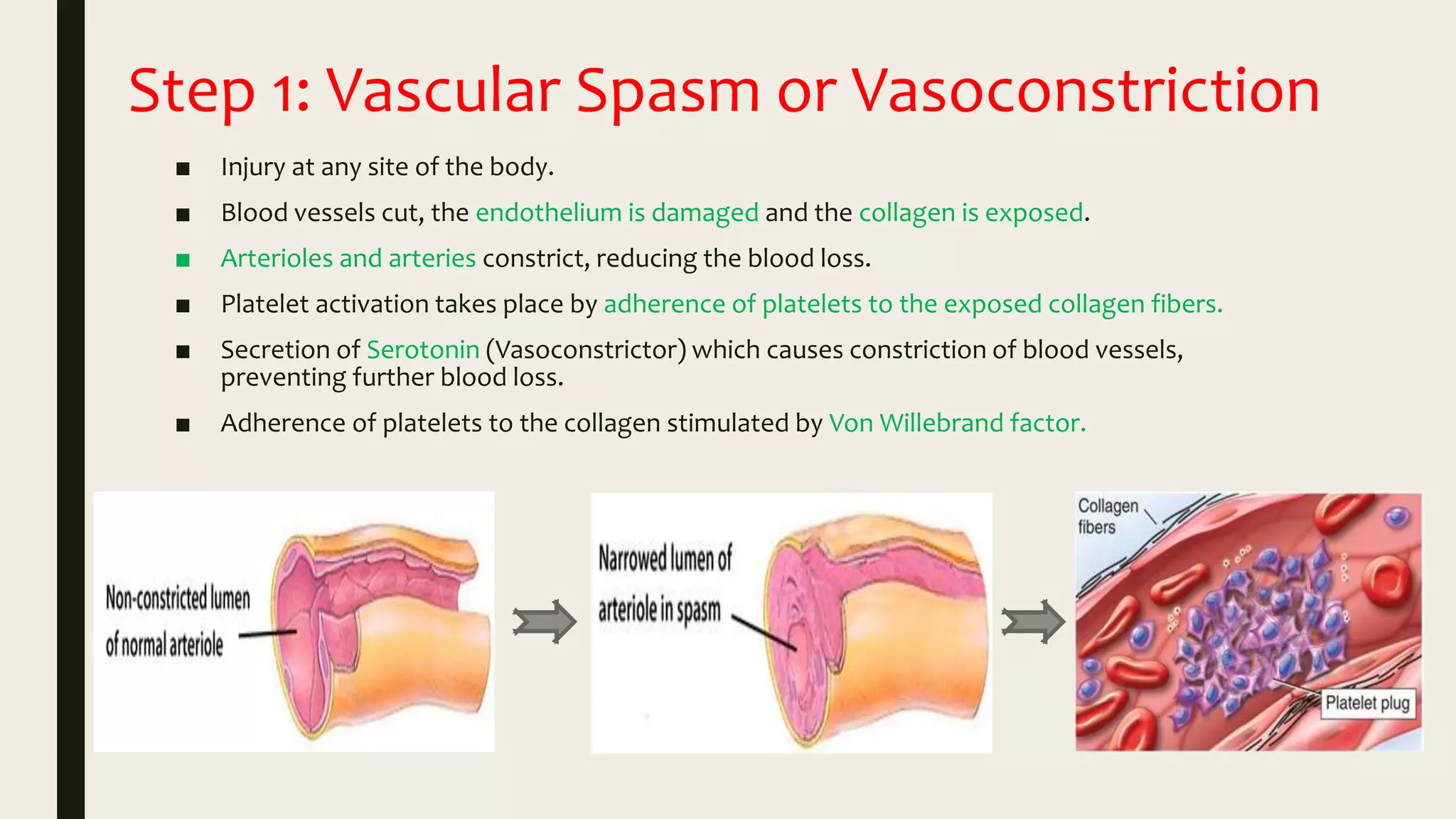
1. Vasoconstriction of blood vessels to reduce blood flow through the damaged vessel.
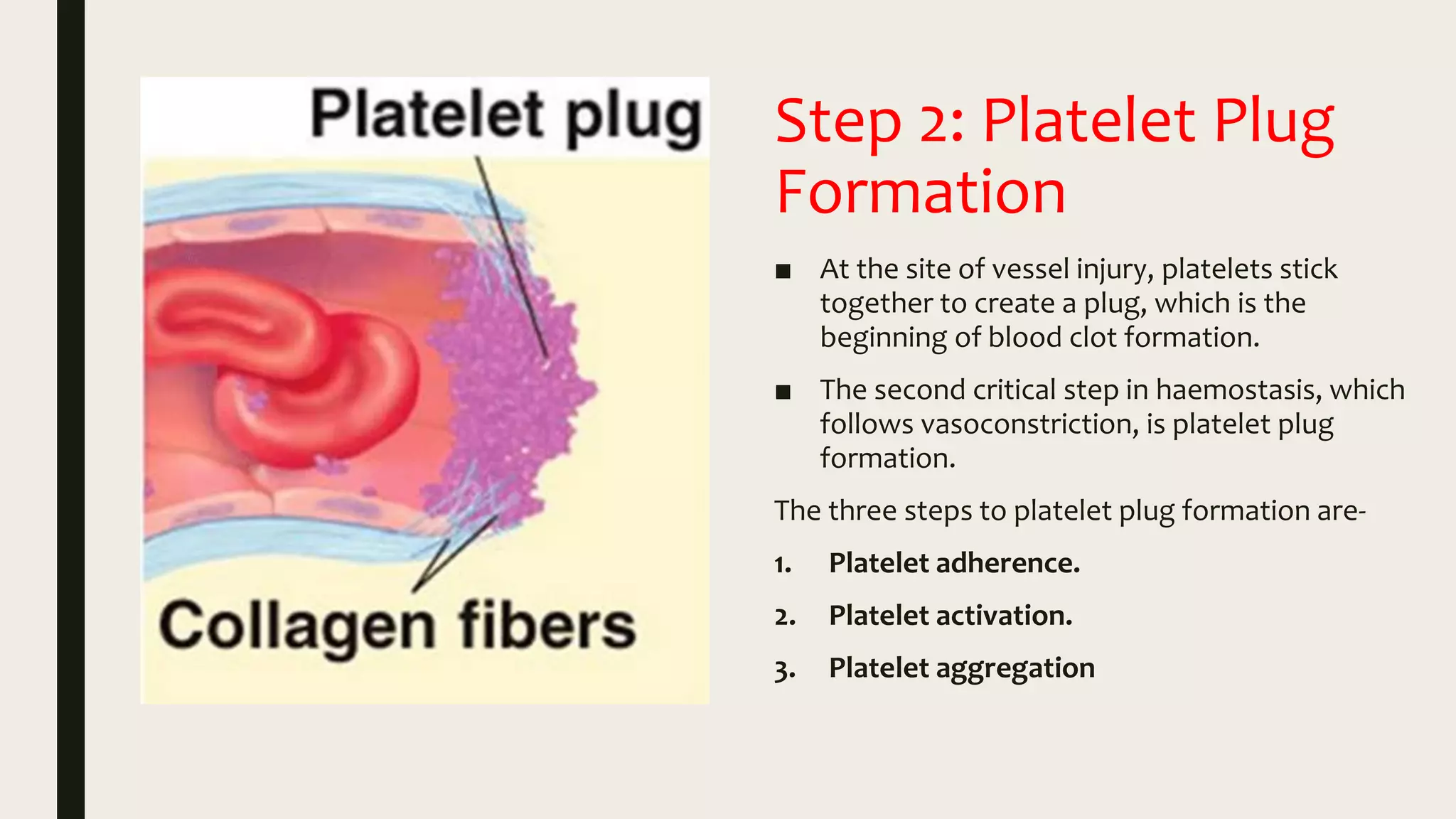
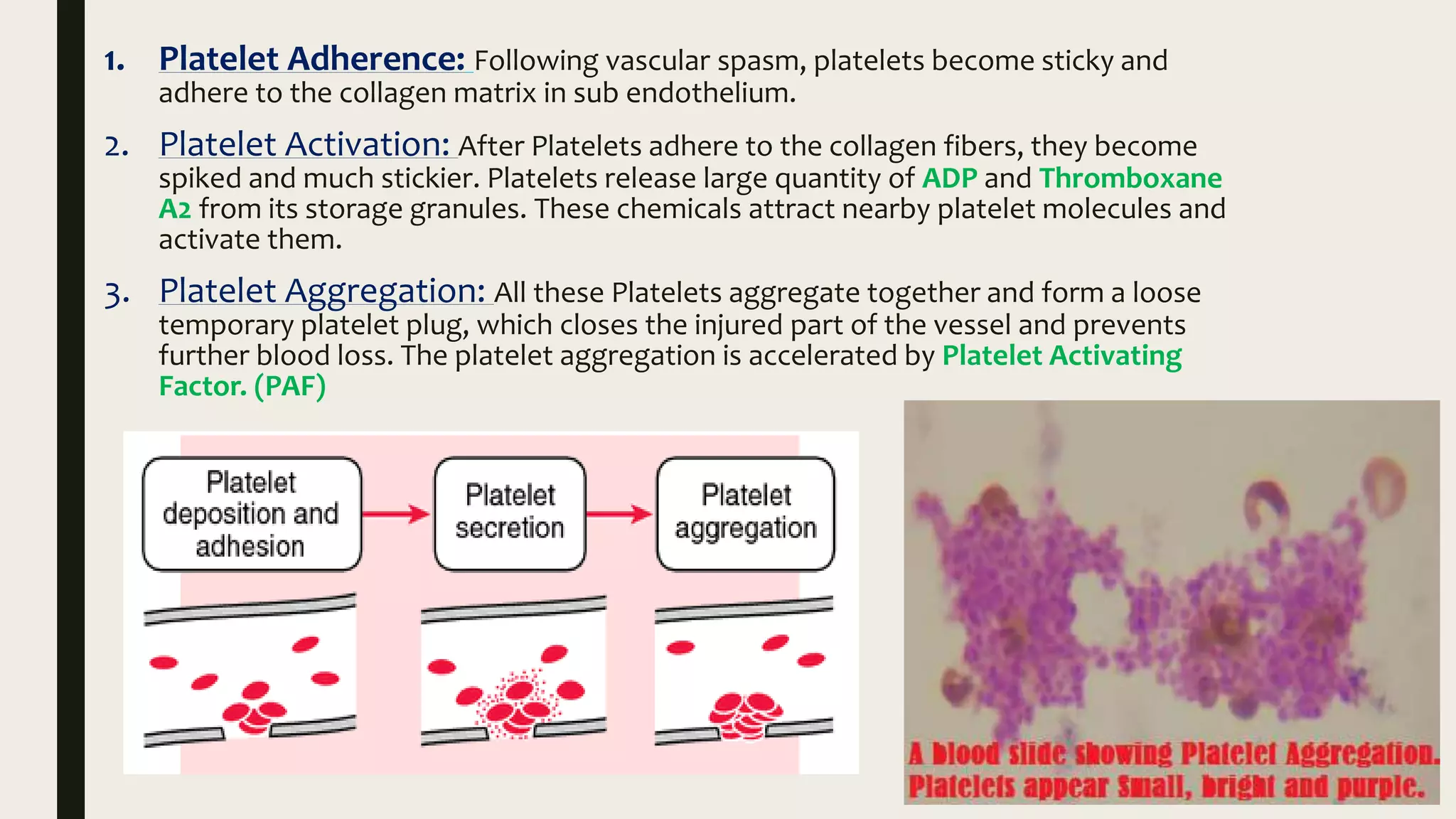
2. Formation of a platelet plug at the site of injury through platelet adhesion, activation, and aggregation. Chemicals released by platelets attract more platelets to form a temporary plug.
3. Coagulation cascade where prothrombin is converted to thrombin which then converts fibrinogen to fibrin, forming a mesh that strengthens the platelet plug.
Over time fibrin is broken down by plasmin in a process called fibrinolysis to remove the clot from the blood vessel. Together these processes