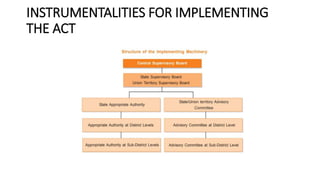
The document discusses the Pre-Conception and Prenatal Diagnostic Techniques (Prohibition of Sex Selection) Act, 1994 (PCPNDT Act). It provides an overview of key aspects of the act including definitions, registration requirements, prohibitions, and penalties. The act aims to regulate prenatal diagnostic techniques and prevent their misuse for sex determination and female feticide. Clinics must register and follow guidelines on maintaining records and obtaining consent. Sex determination is prohibited except for certain medical reasons. Violations can lead to imprisonment, fines, and suspension of medical licenses.






























![FURTHER PERMISSIBLE [“4 A’s”]–
• AGE OF THE PREGNANT WOMAN IS ABOVE 35YEARS
• ABORTIONs - PREGNANT WOMAN HAS UNDERGONE 2 OR MORE
SPONTANEOUS ABORTIONS OR FOETAL LOSS
• AGENTS - PREGNANT WOMAN HAS BEEN EXPOSED TO POTENTIALLY
TERATOGENIC AGENTS SUCH AS DRUGS, RADIATION, INFECTION OR CHEMICALS
• AMENTIA -THE PREGNANT WOMAN OR HER SPOUSE HAS A FAMILY HISTORY OF
MENTAL RETARDATION OR PHYSICAL DEFORMITIES SUCH AS, SPASTICITY OR
ANY OTHER GENETIC DISEASE](https://image.slidesharecdn.com/doc-20220623-wa0005-230217185317-63764618/85/DOC-20220623-WA0005-pptx-32-320.jpg)