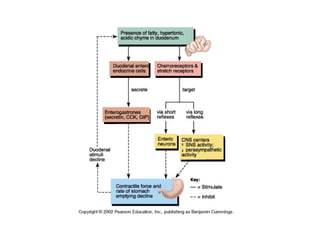
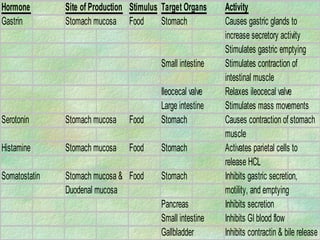
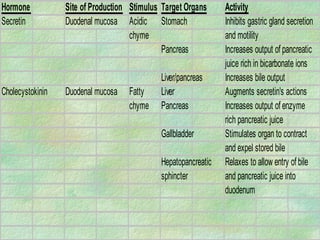
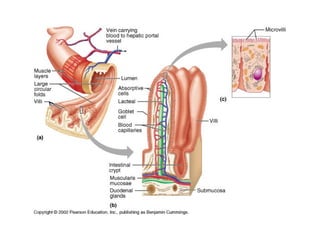
The document discusses digestion and absorption in the gastrointestinal tract. It describes:
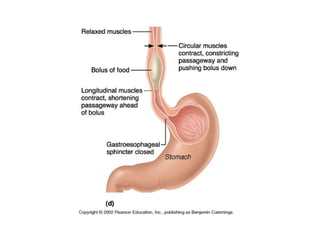
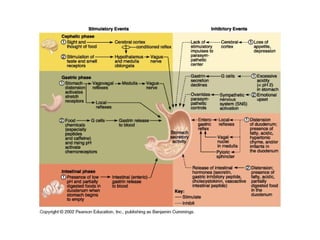
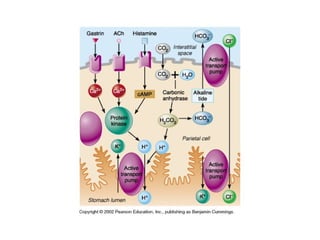
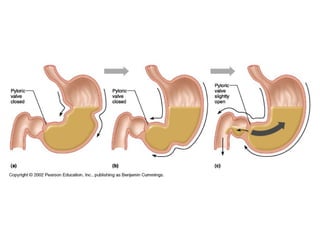
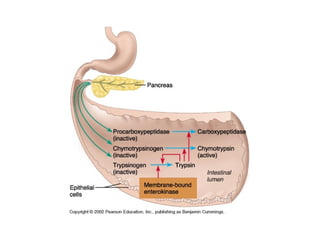
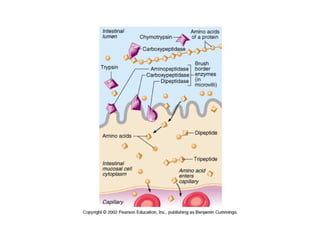
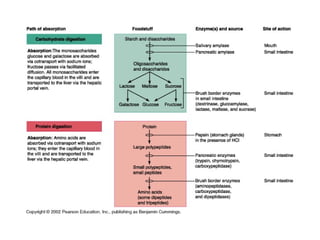
- The mechanical and chemical breakdown of food that occurs in the mouth, stomach, and small and large intestines. This includes the roles of enzymes like pepsin, trypsin, amylase, and lipases.
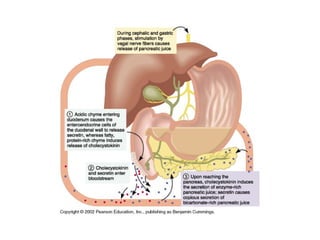
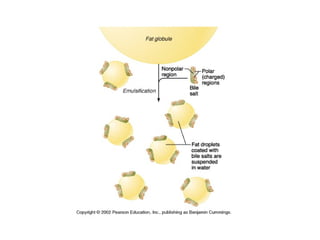
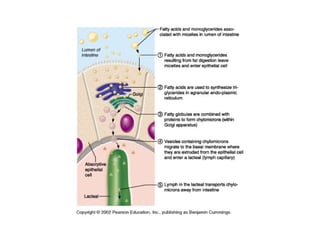
- How nutrients are absorbed in the small intestine, including the roles of micelles in fat absorption and iron-binding proteins in iron transport.
- Causes of malabsorption like problems delivering bile or pancreatic juices or damage to the intestinal lining.