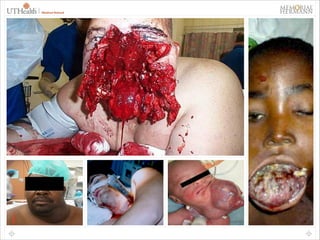
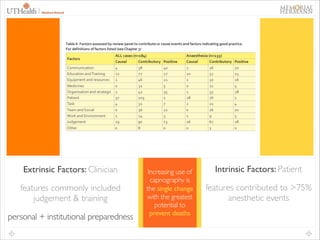
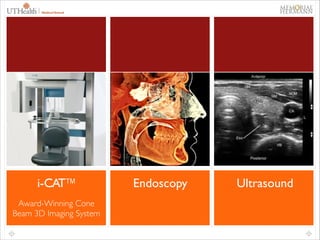
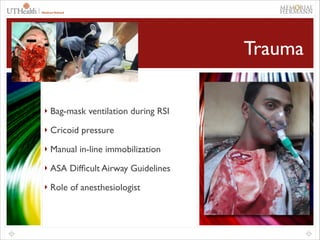
This document provides an overview of difficult airway management concepts. It begins by outlining the scope of the problem, noting that 1-3% of general anesthetics involve an unanticipated difficult airway. Key factors that contribute to difficult airways are discussed, including patient characteristics and clinician experience. A variety of airway devices and techniques to secure the airway are presented, including video laryngoscopy, fiberoptic intubation, supraglottic airways, and surgical options like cricothyrotomy. The document emphasizes the importance of thorough pre-operative airway assessment and having a well-thought out plan for managing difficult airway scenarios.