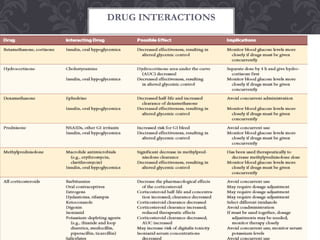
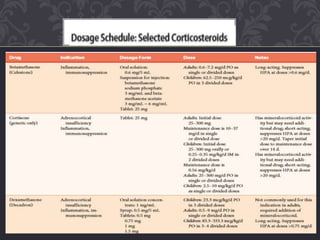
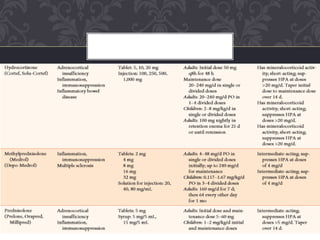
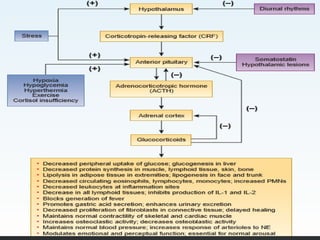
Corticosteroids are steroid hormones produced naturally in the adrenal cortex or administered synthetically. They have anti-inflammatory and immunosuppressive effects and are used to treat various conditions. Common corticosteroids include cortisol, prednisone, and dexamethasone. Nurses monitor patients on corticosteroids for adverse effects like hypertension, infections, weight gain, and bone loss and taper doses when discontinuing long-term therapy to prevent adrenal insufficiency.












![• Patients positive for hepatitis B surface antigen.
• Patients with hypertension and cardiovascular
disorders (e.g., heart failure [HF])
(large doses of drugs with high relative mineralocorticoid potency
(e.g., cortisone and hydrocortisone) can cause elevated blood
pressure, salt and water retention, and increased excretion of
potassium)
• Used with caution in renal insufficiency, acute
glomerulonephritis, or chronic nephritis.](https://image.slidesharecdn.com/corticosteroids-200515055728/85/Corticosteroids-15-320.jpg)