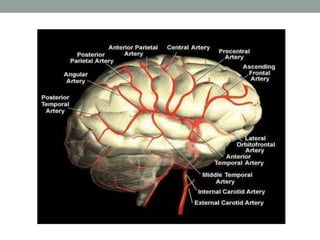
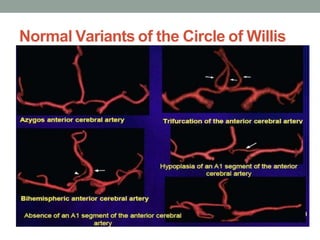
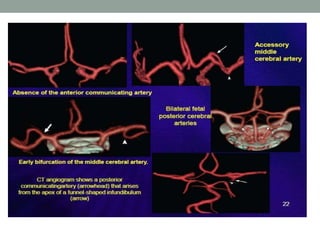
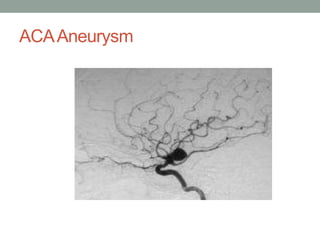
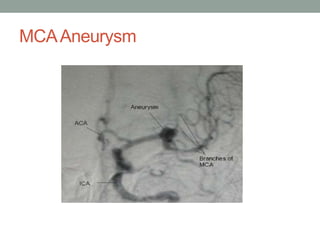
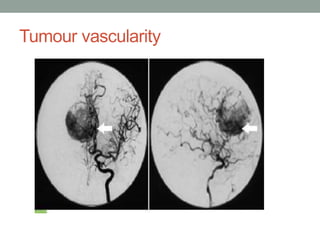
Digital subtraction angiography (DSA) provides high quality images of cerebral vasculature and remains the gold standard. It involves injecting iodinated contrast into arteries and digitally subtracting pre-and post-contrast images to visualize vessels. Modern DSA uses flat panel detectors for higher resolution and lower radiation. It allows 3D reconstruction of vessel anatomy and is useful for diagnosing and treating conditions like aneurysms and AVMs. While very accurate for vessels, DSA cannot simultaneously image bone which CT angiography can provide.