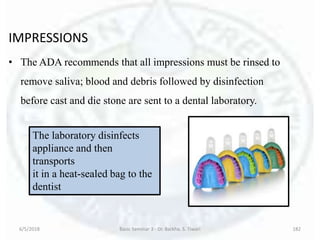
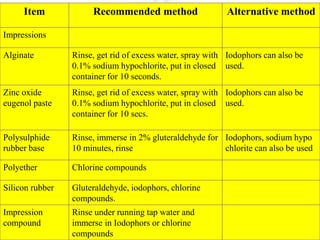
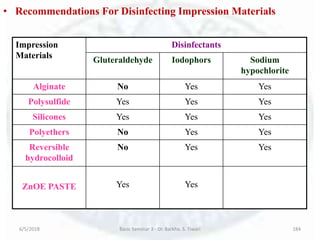
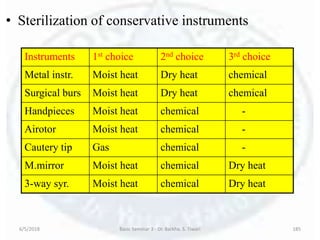
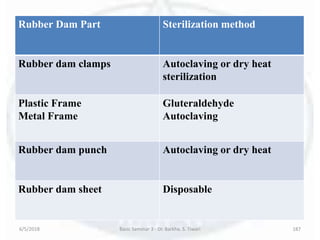
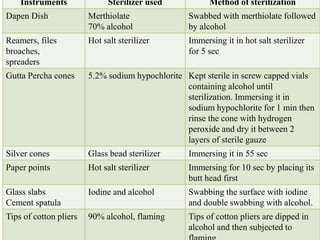
The document discusses sterilization and disinfection, covering historical developments, definitions, principles, and various methods. It highlights key figures in microbiology such as Louis Pasteur and Joseph Lister, and distinguishes between terms like sterilization, disinfection, and biocides. The document also elaborates on the processes, monitoring techniques, and different agents used for effective sterilization and disinfection.







































































































































![In dentistry:
• 3% of hydrogen peroxide is used as an irrigant
• The rapid release of nascent oxygen [O] in contact with
organic tissue effervescence dislodges the necrotic tissue
and dentinal debris.
6/5/2018 Basic Seminar 3 - Dr. Barkha. S. Tiwari 152](https://image.slidesharecdn.com/basicseminar3-sterilizationanddisinfection-180605145230/85/Basic-seminar-3-sterilization-and-disinfection-152-320.jpg)