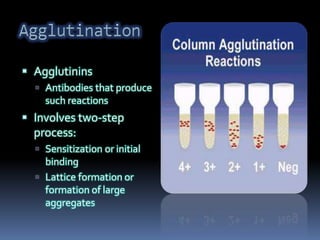
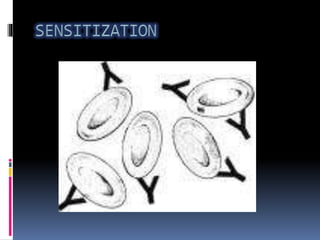
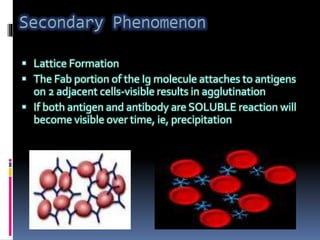
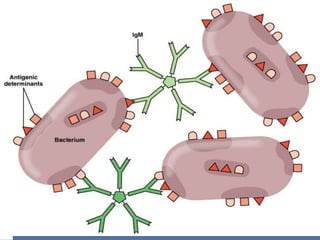
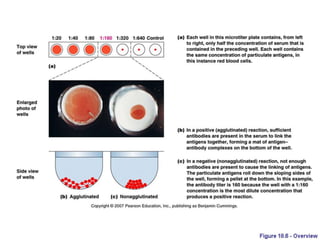
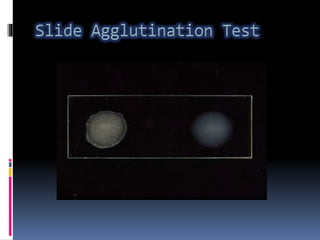
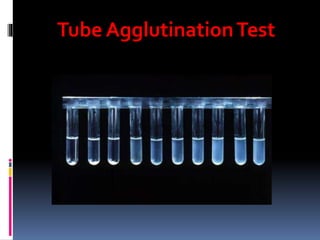
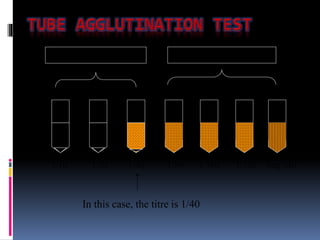
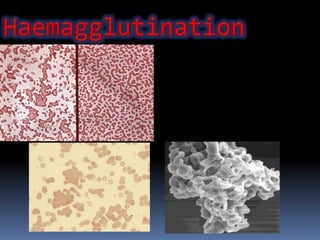
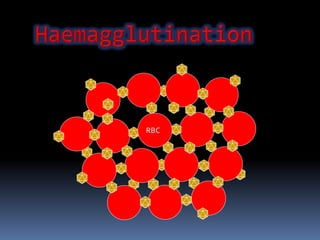
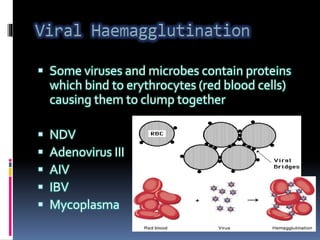
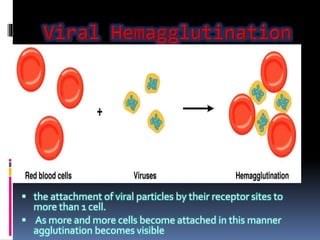
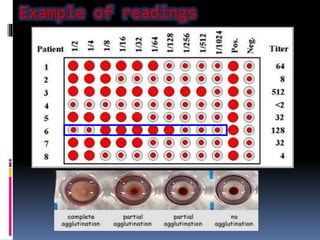
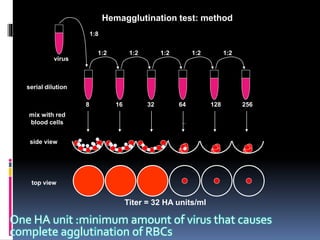
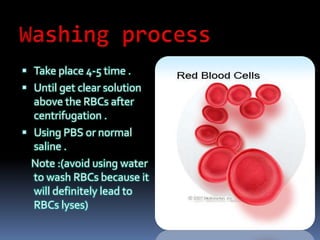
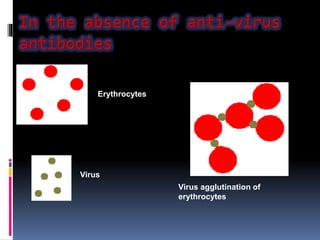
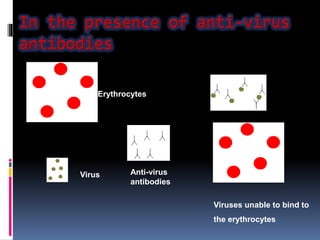
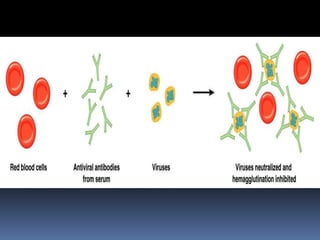
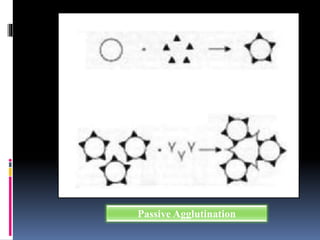
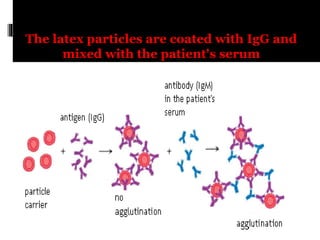
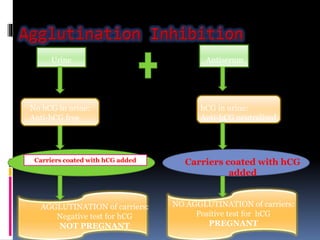
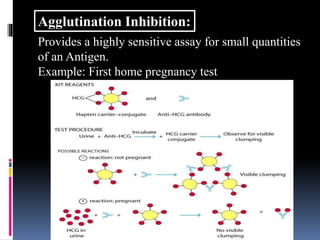
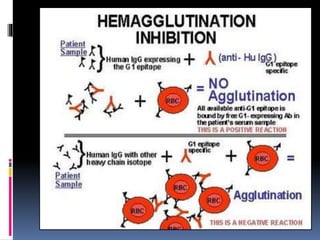
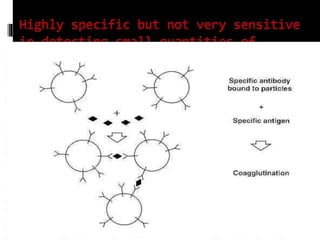
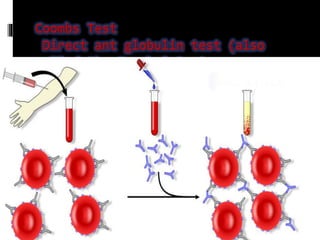
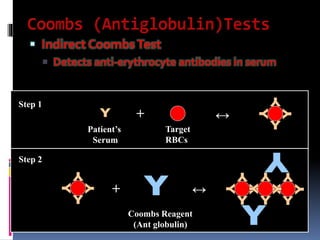
Agglutination is the clumping of particulate antigens caused by antibody binding. It was first observed in 1896 using bacterial cells and serum antibody. Antibodies that cause agglutination are called agglutinins. Agglutination involves an initial antigen-antibody binding step followed by lattice formation into large aggregates. Erythrocytes, bacteria, and latex particles can all participate. The reaction is influenced by factors like ionic strength, pH, temperature, and viscosity. It can be directly observed on cell surfaces or indirectly using antigen-coated carriers like latex beads. Agglutination tests are used to diagnose various infectious diseases.