Menstruation cycle
- 1. MENSTRUATION CYCLE MR.SHYAM BHATEWARA LECTURER AT INDEX NURSING COLLEGE
- 2. DEFINITION Menstrual cycle is the visible manifestation of cyclic physiological uterine bleeding due to shedding of endometrium & blood outflow through the vagina followed by invisible role of hormone, known as menstruation cycle.
- 3. HPO Axis Hypothalamus :- GnRH (gonadotropin releasing hormone) Pitutary:- Anterior pituitary called adeno-hypophysis Gn hormone (gonadotropin hormone) Ovary :- oestrogen & progesterone
- 4. GnRH Activate anterior pituitary hormone Secrete hormone FSH & LH These hormone are work on ovary And ovary release oestrogen & progesterone Menstruation cycle occur
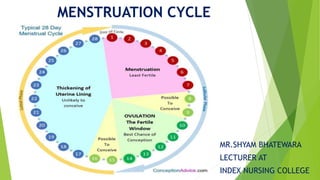
- 5. IMPORTANT POINT FOR MENSTRUATION CYCLE Duration of cycle = 28 days 1st menstruation cycle called menarche Amount of blood loss during one cycle 35 ml (20-80 ml) Menstrual phase = 1-7 days Duration of bleeding = 2-7 days (3-5 days) Puberty = development of secondary sexual characteristics age of puberty -10-16 years in female - 12-16 years in male
- 6. ACCORDING TO TANNER & MARSHALL 5 STAGES OF PUBERTY 1. Breast development – Thelarche (1st sign of puberty in female) 2. Axillary hair development – Adrenarche 3. Pubic hair development –pubarche 4. Increase in hight 5. 1st menstrual cycle- menarche (last sign of puberty in female) Peak age of menarche – 13 years 1st menstrual cycle mostly eggless Last menstrual cycle is also eggless
- 7. REPRODUCTIVE AGE Reproductive age = child bearing age Menarche to menopause 30 years 15 years to 45 years Female ovary has 13 menses in a year Around 400 menses in complete reproductive life
- 8. NO. OF FOLLICLES 20 weeks of female fetus – 7 million on. Of follicles(70 lacs) At birth – 2 million Reproductive age – 4 million After menopause – less than 10000no. Of follicles
- 9. MENSTRUAL BLOOD Menstrual blood is totally waste & dark red blood in colour contain- Mucus Dead endometrial cells Prostaglandins Micro-organisms Menstrual does not clot because of plsmin
- 10. CHANGES DURING MENSTRUAL CYCLE 1. Ovarian changes – a) Follicular phase b) Luteal phase 2. Uterine changes- a) Bleeding phase b) Proliferative phase c) Secretory phase
- 11. OVARIAN CHANGES 1. Follicular phase- It is first half of the menstrual cycle It also called pre-ovulatory phase Up to 14 days Immature follicles become mature in the presence of FSH 2. Luteal phase- 15 – 28 days 2nd half of menstrual cycle Post ovulatory phase Formation of corpus luteum Corpus luteum is yellow colour body formation after rapture of graafian follicle Function- secretion of hormone progesterone( in large amount) & oestrogen (in small amount )
- 12. UTERINE CHANGES Bleeding phase/ menstrual phase:- (menses, periods, catamania) Bleeding phase 1-5 days may up to 7 days At the end of the bleeding phase thickness of endometrium 1-2 mm Normal thickness 8-10 mm
- 13. If fertilization not occur Corpus luteum disappear at 26- 28 dyas Decrease progesterone & oestrogen Causes vasoconstriction Contraction of uterine artery Decrease blood supply to the uterus Hypoxia & ischemia occur Endometrial cells dead Shedding of Endometrial cells Blood vessels open & bleeding from uterus Blood & dead cells collected in uterus nerve stimulation of uterus Posterior pituitary release Oxytocin Act on myometrium of uterus Causes uterine contraction Blood through the vagina
- 14. PROLIFERATIVE PHASE 6-14 days Division of the endometrium cells Increase no of endometrial cells Due to oestrogen hormone Growing follicles release oestrogen hormon Division of endometrial cells
- 15. SECRETARY PHASE Also known as preparatory phase 15-28 days Secretory activity of corpus luteum Progesterone increase size of endometrial cells at this phase endometrium is prepared for next M. cycle if fertilization not occur Endometrium also prepare for implantation if fertilization occur
- 16. HORMONAL REGULATION OF MENSTRUATION CYCLE Follicle phase – FSH Ovulation – LH Luteal phase- FSH & LH Bleeding phase- decrease progesterone & oestrogen Proliferative phase – oestrogen hormone Secretory phase - progesterone & oestrogen
