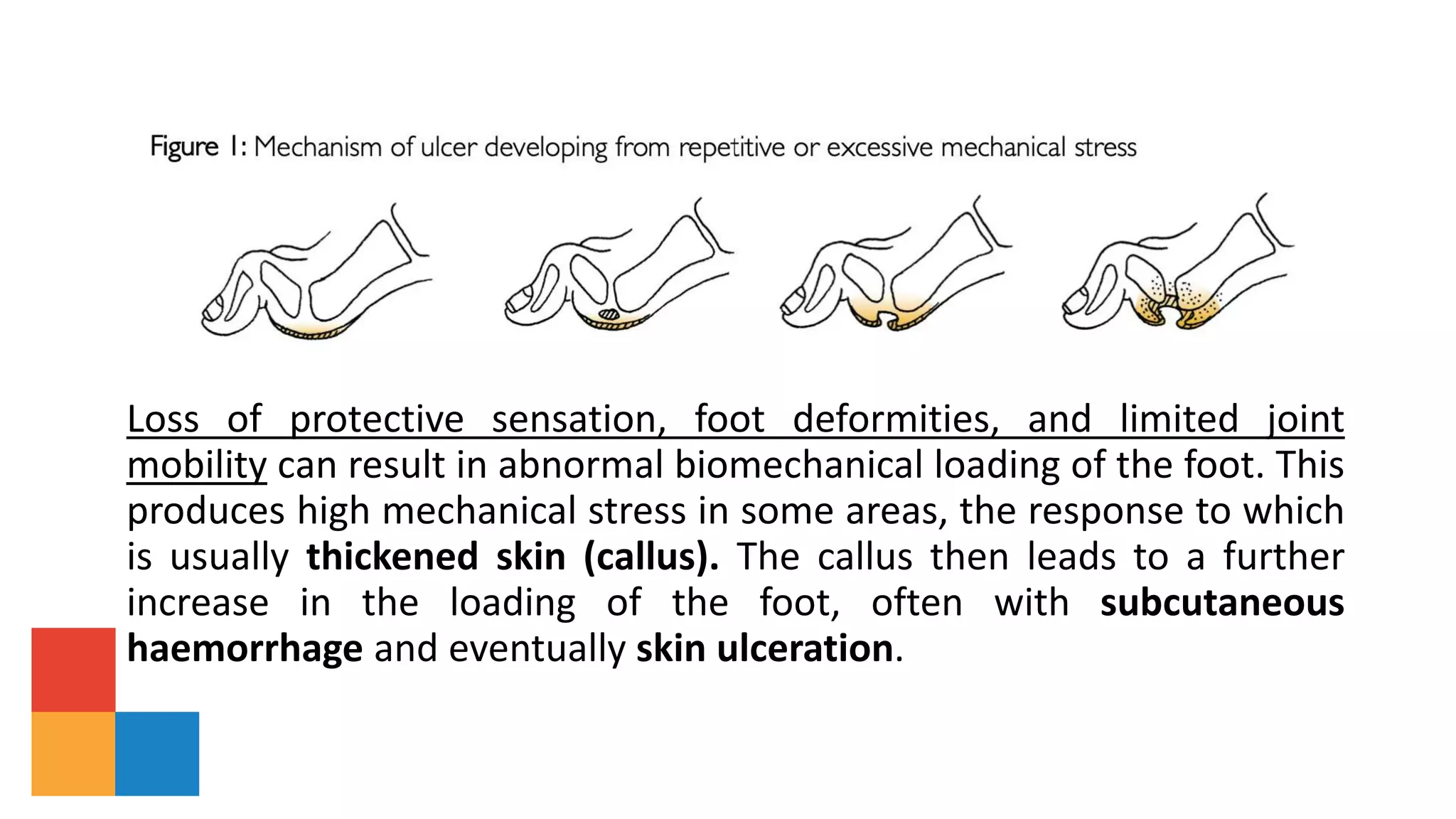
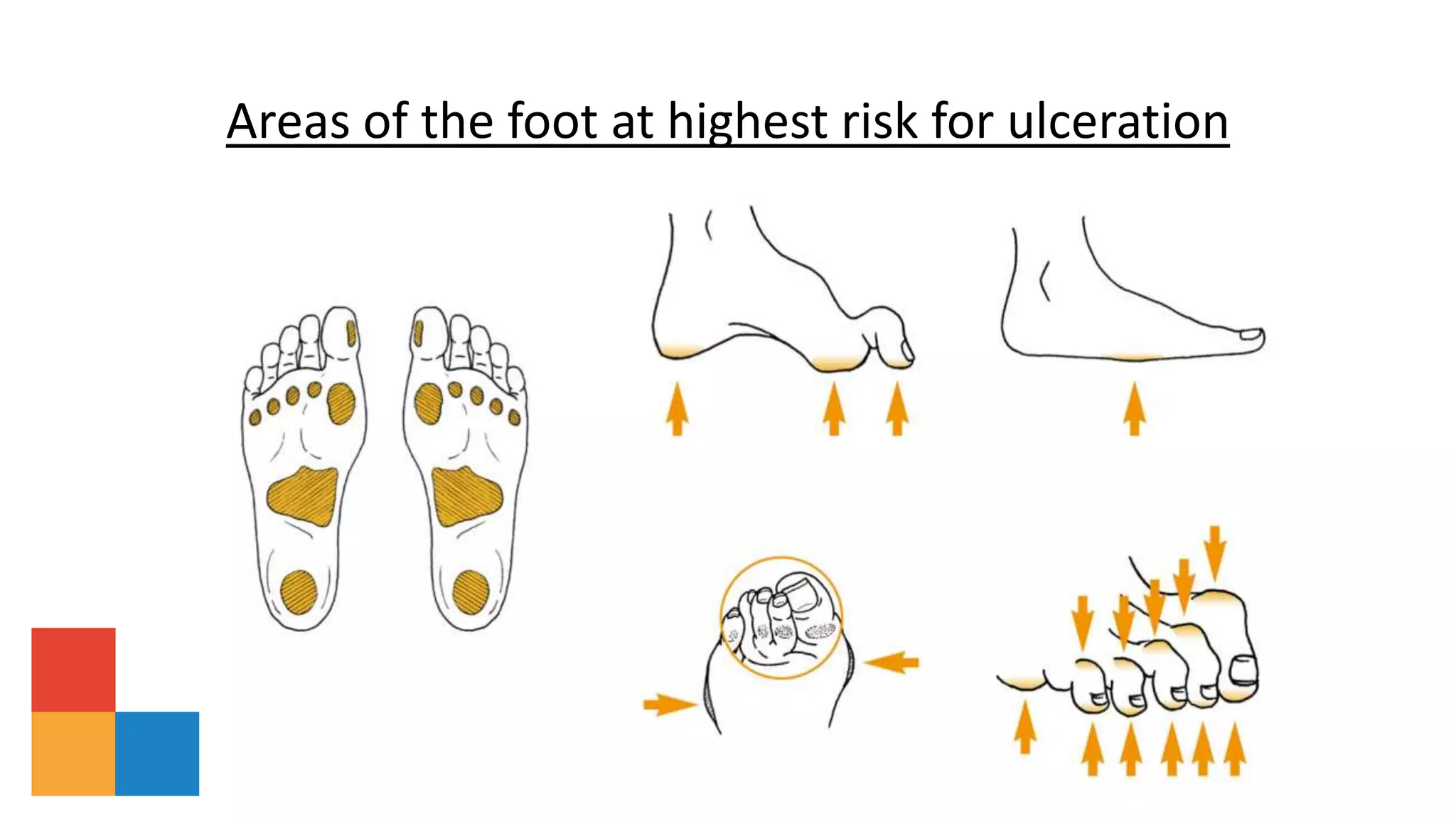
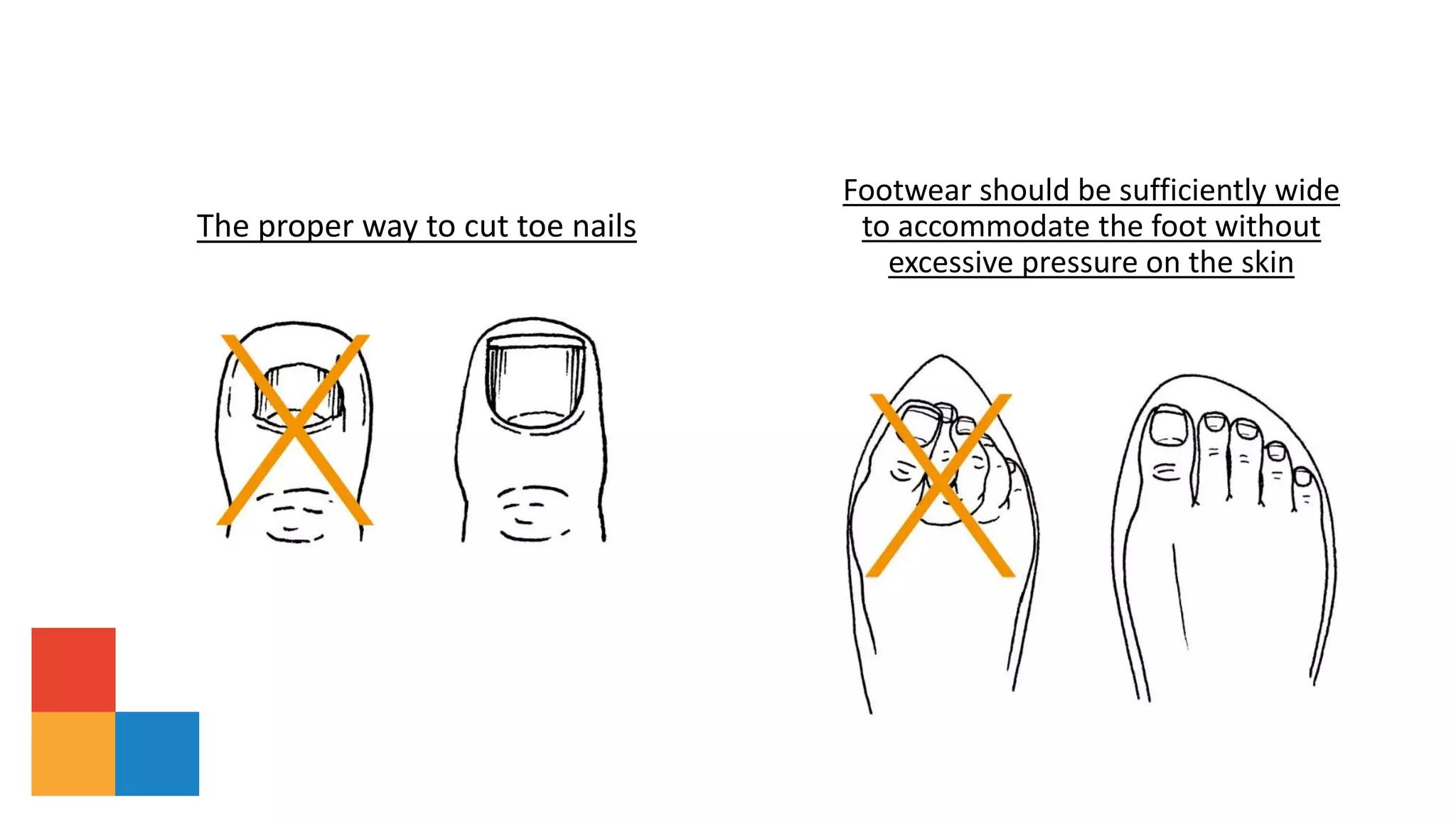
The document summarizes guidelines from the International Working Group on the Diabetic Foot (IWGDF) for the prevention and management of diabetic foot disease. It provides an overview of updates to the 2019 guidelines, including new recommendations and reordering of ulcer treatment principles. Key aspects of diabetic foot disease and ulcer assessment, classification, and treatment are described, including risk factors, offloading, wound care, infection treatment, and revascularization. Guidelines for active Charcot neuro-osteoarthropathy are also summarized.