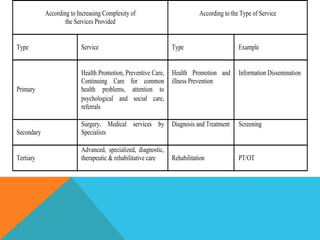
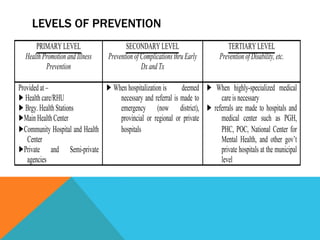
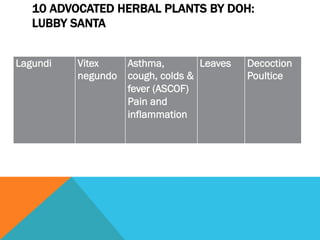
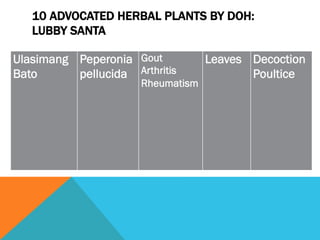
Community health nursing involves promoting health, preventing disease, and managing factors affecting health at the community level. It aims to raise the overall health status of populations. A community is defined as a group of people living in a specific geographical area with common characteristics or interests. Community health nursing utilizes the nursing process to provide care to individuals, families, population groups, and communities. It combines public health science with nursing skills and social assistance. The community is considered the patient, with the family as the unit of care.