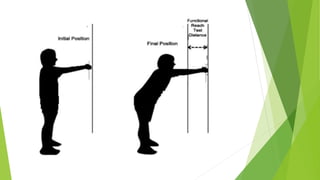
This document discusses several functional assessment scales used to evaluate patients. The Berg Balance Scale assesses static and dynamic balance abilities through 14 tasks. The Barthel Index measures dependence in activities of daily living like feeding, bathing, and mobility. The Functional Independence Measure assesses disability levels and needed assistance for 18 activities. The Action Research Arm Test evaluates upper extremity function through 19 hand and arm tasks. The Functional Reach Test measures forward balance ability, while the Multi-directional Reach Test assesses limits of stability in four directions. All scales are reliable and valid for assessing functional abilities.