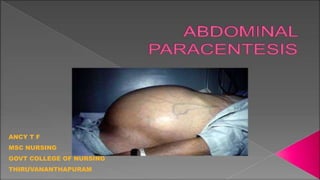
Paracentesis
- 1. ANCY T F MSC NURSING GOVT COLLEGE OF NURSING THIRUVANANTHAPURAM
- 2. Itoduction Paracentesis is a procedure frequently performed in the intensive care unit for diagnostic and therapeutic purposes. Paracentesis was once considered a routine form of treatment for ascites but is now performed primarily for diagnostic examination of ascitic fluid, for treatment of massive ascites that is resistant to nutritional and diuretic.
- 3. DEFINITION Paracentesis is the removal of fluid (ascites) from the peritoneal cavity through a small surgical incision or puncture made through the abdominal wall under sterile conditions.
- 4. PURPOSES To relieve pressure on the abdominal and chest organs due to ascites To study chemical, bacteriological and cellular composition of peritoneal fluid for diagnosis of disease. To drain exudate in peritonitis. To prepare for procedures like peritoneal dialysis.
- 5. 1 To relieve pressure on the abdominal and chest organs due to ascites acitis can make difficutty in breathing,eating, moving It iead to hard to breath 2 To study chemical, bacteriological and cellular composition of peritoneal fluid for diagnosis of disease. serum-albumin 3. To drain exudate in peritonitis Peritoneal exudate fluid is very small in quantity and contains some neutrophilic leukocytes, macrophages and lymphocytes. The peritoneal exudate is therefore usually collected to obtain the leukocytes, especially free macrophages.
- 6. 4.To prepare for procedures like peritoneal dialysis. In alcoholic cirrhotic patients with ascites, gastric emptying of solids is delayed, independently of the volume of ascites.
- 7. INDICATION
- 8. Diagnostic paracentesis patients with suspected spontaneous bacterial peritonitis (SBP) ascites of unknown cause. Other less common diagnostic studies include: triglycerides (chylous ascites), amylase (pancreatic ascites) mycobacterial culture (tuberculous ascites) bilirubin (bile leak).
- 9. Therapeutic Paracentesis patients with significant shortness of breath or abdominal discomfort decompensated cirrhosis abdominal pain from distention percutaneous decompression of resuscitation-induced abdominal compartment syndrome.
- 11. Pre procedure 1. Check For signed consent Form. 2. Prepare the patient by providing the necessary information and Instructions and by offering reassurance. 3. Instruct the patient to void. 4. Gather appropriate sterile equipment. 5. Place the patient in upright position on the edge of the bed or in a chair with feet supported on a stool. 6. Place the sphygmomanometer cuff around patient’s arm.
- 12. Procedure 1. The physician, using aseptic technique, inserts the trocar through a puncture below the umbilicus. The trocar or needle is connected to a drainage tube, the end of which is inserted into a collecting receptacle. 2. Help the patient maintain position throughout the procedure. 3. Measure and record blood pressure at frequent intervals throughout the procedure. 4. Monitor the patient closely for signs of vascular collapse: pallor, increased pulse rate, or decreased blood pressure.
- 13. Post procedure. 1.Return the patient to bed or to a comfortable sitting position. 2 Measure, describe. and record the fluid collected. 3, Label samples of fluid and send to laboratory. 4. Monitor vital signs every 15 min for1 h, every 30 min for 2 h, every hour for 2 h, and then every 4 hr. 5.Measure the patient’s temperature.
- 14. 6. Assess For hypovolemia, electrolyte shifts, changes in mental status, and encephalopathy. 7. When taking vital signs, check puncture site for leakage or bleeding. 8. Provide patient teaching regarding need to monitor for bleeding or excessive drainage from puncture site, importance of avoiding heavy lifting or straining, the need to change position slowly, and frequency of monitoring for Fever.
- 15. COMPLICATIONS
- 16. • bleeding and persistent ascitic leak. • intestinal or urinary bladder perforation, with associated peritonitis and infection. • transient hypotension and paracentesis-induced circulatory dysfunction (PICD) • a drop in blood pressure, which only occurs if a significant volume of fluid is removed • an accidental puncture of a blood vessel, the bowel, or the bladder • an acute kidney injury