Ariunaa congenital spine disorders
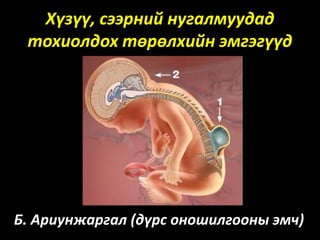
- 1. Хүзүү, сээрний нугалмуудад тохиолдох төрөлхийн эмгэгүүд Б. Ариунжаргал (дүрс оношилгооны эмч)
- 2. Нуруу нугасны төрөлхийн эмгэгүүдийн ангилал 1. Үндсэн ангилал • Abnormalities of Neurulation • Anomalies of Notochord Development • Anomalies of Vertebral Formation and Segmentation • Normal Anatomical Variations • Congenital and Developmental Abnormalities • Anomalies of the Caudal Cell Mass
- 3. 2. Нуруу болон нугасны хөндийд илэрдэг үүсгэвэрүүдийг: • Spinal dysraphism – олон хэлбэрүүдтэй. • Caudal spinal anomalies – нугасны төгсгөл хэсгийн эмгэгүүд гэж ерөнхийд нь ангилна.
- 6. OPEN SPINAL DYSRAPHISM • Бүгд буюу 99% нь myelomeningoceles • Бүх OSD өвчтөнүүд Chiari II өөрчлөлттэй хавсардаг. Spina bifida aperta: MYELOCELE AND MYELOMENINGOCELE • Нугалам үр хөврөлийн хөгжлийн явцдаа бүрэн нийлж чадаагүйгээс үүсдэг.
- 8. Spina bifida occulta: Ихэвчлэн тохиолддог хэлбэр ба рентген шинжилгээгээр л оношлогддог Spina bifida aperta: Meningocele Myelomeningocele Myelocystocele lipomeningocele
- 11. Posterior meningocele. A, Sagittal T1-weighted MR зурганд 12 сартай хүүхдэд дагзны хэсэгт тархи нугасны шингэний бүтэцтэй арагшаа байрлалтай менингоцеле B, Sagittal T2-weighted MR зурагт 5 сартай хүүд хүзүүний нугалмын түвшинд маш том хэмжээтэй арагшаа байрлалтай менингоцеле C, Sagittal T2-weighted MR зурагт бүсэлхийн хэсэгт жижиг арагшаа байрлалтай менингоцеле
- 12. Meningocele. T2 горимд - 6 сартай хүүхдэд урагшаа байрлалтай менингоцеле харагдана.
- 14. Chiaric-I malformation: Бага тархины тонзил хэсгийн ивэрхий - төрөлхийн эмгэг өөрчлөлт бөгөөд хүүхэд насанд шинж тэмдэг илэрдэггүй ба насанд хүрэгчдэд сколиоз болон syrinx өөрчлөлтүүдтэй хавсарвал толгой өвдөх зовиур илэрдэг. Tonsil хэсэг foramen magnum- с доош 5мм-с илүү хэмжээгээр ивэрвэл Chairi I гэж үзнэ. 5мм хүртэл ивэрсэн бол хоргүй Tonsil ectopia гэж үзнэ. MRI: Peg-like буюу ивэрсэн хэсэг соёо шүд мэт харагддаг. Мөн бага тархины ховилууд V – хэлбэртэй буюу sergeant stripes sign харагдана. Тус эмгэг 3-н үе шаттай. I: Шинж тэмдэггүй үе II: Тархины багана хэсэг дарагдах III: syrinx
- 17. Chiari Type 1 Malformation.
- 19. Chiari-II malformation: Бага тархины тонзил хэсгийн ивэрхийтэй хавсарч бүсэлхийн myelomeningocele. Зөвхөн тонзил хэсэг дангаар бус бага тархи бүхэлдээ доошилж шахагддаг. Low-lying torcular herophili -н байрлал доошлох, tectal beaking тектум үзүүртэй мэт хэлбэртэй болох, гидроцефали, кливум ясны дутуу хөгжил зэрэг нь сонгомол шинжүүд юм.
- 20. Fetal T2-weighted MR images. A, Chiari II malformation ( arrows ) on sagittal image. B, Lumbosacral myelocele with low-placed spinal cord ( arrow ) on axial image. C, Dysraphic defect plus placode ( arrow) on axial image.
- 21. Chiari II malformation ( arrows in A ) and lumbosacral myelomeningocele ( arrow in B ) on sagittal T2-weighted fetal MR images.
- 22. Chiari Type 11 Malformation.
- 23. Type II Chiari malformation in a 14-month-old child. Sagittal T1-weighted images demonstrating hydrocephalus (A) with a small posterior fossa and downward herniation of the cerebellum and medulla (B).
- 24. Chiari-III malformation: Оccipital encephalocele буюу дагзны хэсэгт том хэмжээтэй ивэрхий үүсдэг. Syringomyelia болон hydrocephalus тод илэрнэ. Chiari- IV malformation: Хамгийн хүнд хэлбэр нь бөгөөд амьдрах боломжгүй.
- 25. Type 3 Chiari malformation.
- 26. Chiari III.
- 27. Type IV Chiari malformation.
- 28. Type IV Chiari malformation.
- 29. Арьсан Дор Үүсгэвэргүй Хаалттай Spinal Dysraphisms Энэ ангилалд: intradural lipoma, filar lipoma, tight filum terminale, persistent terminal ventricle болон dermal sinus зэрэг өөрчлөлтүүд орно. Эдгээр өөрчлөлтүүд багана нурууны доод хэсэгт ихэвчлэн тохиолддог.
- 32. Нуруу нугасны липома—Үндсэн 2 хэсэг болгон ангилах бөгөөд нугасны хөндийн интрадурал болон нугасны төгсгөлийн липома гэж хувааж үздэг. Байрлалын хувьд насанд хүрэгчдэд ихэвчлэн цээжний түвшинд, хүүхдэд хүзүүний нугалмын түвшинд байрлана. MRI: Интрадурал липомууд нь тод жигд зах хүрээтэй бөгөөд нугасны эдэд нөлөөлдөггүй ба шинжилгээнд T1: hyperintense T2: hypointense T1 C+ (Gd): no enhancement Өөх дарангуйлсан горимд: hypointense
- 33. Neurenteric cyst in 3-year-old girl. A and B, Sagittal T2-weighted (A) and axial T1-weighted (B) MR images show bilobed neurenteric cyst (arrows) extending from central canal into posterior mediastinum. C, Three-dimensional CT reconstruction image shows osseous opening (arrow) through which neurenteric cyst passes. This opening is called the Kovalevsky canal.
- 34. Нугалмын арын хэсгийн бүрэн бус нийлэх эмгэг- Spina bifida нь spinous process/ lamina бүрэн нийлж чадаагүй эмгэг өөрчлөлт юм. Байрлал С1-TH1 хэсэгт байрладаг. A dermal sinus нь арьсны гадаргуутай хучуур эсийн бүтэц бүхий сувгаар нугасны хөндийтэй холбогдсон эмгэг өөрчлөлт бөгөөд цээж, болон хүзүүний хэсэгт ховор тохиолддог.
- 35. Dermal sinus. A and B, Sagittal schematic (A) and sagittal T2-weighted MR image (B) in 9- year-old girl show intradural dermoid (stars) with tract extending from central canal to skin surface (black arrows). Note tenting of dural sac at origin of dermal sinus (white arrows). C, Axial T2-weighted MR image from same patient as in B shows posterior location of hyperintense dermoid (arrow).
- 36. Thoracic dermal sinus ( black arrows ) and dermoid cyst ( white arrows ) on sagittal T1-weighted ( A ), sagittal T2- weighted ( B ), and axial T1-weighted ( C ) MR images.
- 37. Thoracic dermal sinus ( posterior black and white arrows in A, and B ) and cyst with enhancing abscess ( anterior white arrows in B ) with cord edema on sagittal T2-weighted ( A ) and gadolinium-enhanced T1- weighted ( B ) MR images.
- 38. Disorders of midline notochordal integration: Diastematomyelia—Нугасны хөндий болон түүний бүтцийг гол шугамаар босоо шугамаар 2 хэсэгт хуваагдсан өөрчлөлт юм. Хуваагдсан 2 хэсэг тэгш хэмтэй байдаг. Мөн дотор нь – хэсэг болгон ангилна. 1-р хэлбэр нь хувааж буй таславч нь ясан бүтэцтэй байдаг ба субарханойд зай нугасны хэсгийг бүрэн тусгаарладаг. 2-р хэлбэр нь 2 нугасны хэсэг нэг хөндийд тодорхойлогддог.
- 39. Type 1 diastematomyelia. A–C, Sagittal T2-weighted MR (A), axial T2-weighted MR (B), and axial CT with bone algorithm (C) images in 6-year-old boy show two dural tubes separated by osseous bridge (arrows), which is characteristic for type 1 diastematomyelia.
- 40. Lumbar diastematomyelia and split cord with two hemicords ( short arrows in A and B ), two dural sacs, and a bony septum ( long arrows in B and C ) on axial T2-weighted MR images ( A and B ) and an axial CT scan ( C ).
- 41. Type 2 diastematomyelia. A–C, Sagittal T1-weighted (A), coronal T1-weighted (B), and axial T2-weighted (C) MR images in 9-year-old girl show splitting of distal cord into two hemicords (white arrows, B and C) within single dural tube, which is characteristic for type 2 diastematomyelia. Incidental filum lipoma (black arrows, A and B) is present as well.
- 42. Lumbar diastematomyelia with tethered hemicords ( long arrows ), no septum, and a lipoma ( short arrow ) on sagittal T1-weighted ( A ) and axial T2-weighted ( B ) MR images.
- 43. Нугалмын их биеийн гажигууд
- 44. Нугалмын их биеийн хэвийн хөгжлийн үе шат болон тэдгээрийн үед үүсэх эмгэгүүд
- 45. Asomia буюу L2 нурууны арын хэсэг огт байхгүй. Left hemivertebra- T11 нуруу зөвхөн зүүн талдаа хагас харагдана..
- 46. Butterfly vertebra - эрвээхэй нуруу.
- 48. Block vertebra. L3-L4 хэсэгт нугалмууд бүрэн салаагүй (block vertebra).
- 49. Dorsal hemivertebra – Нугалмын их биеийн урд хэсэг тодорхойлогдохгүй. Сoronal clefts буюу нугалмын их биед завсар үүссэн
- 50. Hemi-vertebrae & Segmented Vertebrae.
- 51. Нугалмын хэсэгчилсэн дутуу хөгжлүүд: сумаар butterfly vertebra, hemivertebra, tripedicular vertebra, өргөсч холдсон butterfly vertebra.
- 52. Limbus vertebra. Бүсэлхийн 4-р нугалмын урд дээд гадаргууд үзүүр хэсэг салангад мэт харагдана .
- 53. limbus vertebra.
- 54. Хүзүүний нугалам дээр ихэвчлэн урд доод гадаргууд илэрдэг ба Teardrop хугарлаас ялган оношлох шаардлагатай. Энэ зурагт Teardrop хугарал харагдаж байна.
- 55. 40 настай эмэгтэй зүүн талдаа гуяруу дагаж өвддөг гэнэ. Зурагт L5 нугалмын зүүн хажуу сэртэн баруунаас том ба ахар сүүл болон сүүжний ястай үелсэн өөрчлөлттэй байна. Sacralisation of L5 vertebra.
- 56. Spondylodysplasias: Spondylodysplasia нь багана нурууны идиопатик сколиоз, төрөлхийн сколиоз, кифоз, Scheuermann –ны өвчин мөн бусад дисплази өөрчлөлтүүд Neurofibromatosis. Achondroplasia. Mucopolysaccharidoses. Down syndrome. Spondyloepiphyseal dysplasia. Craniocervical anomalies. Klippel-Feil syndrome. Spinal vascular anomalies.
- 57. Idiopathic Scoliosis Бага насны хүүхдүүдэд хамгийн түгээмэл тохиолддог. Өсвөр насны 10-с дээш насны хүүхдүүдэд ялангуяа охидод илүү ториолддог. Ихэвчлэн баруун тийш дугуйрсан муруйлт өөрчлөлт сээрний, бүсэлхийн хэсэгт үүсдэг ба 2 дах муруйлт нь эсрэг чиглэлд үүсч болдог. Эмгэг муруйлтын хүндрэл нь зүрх болон уушги дарагдаж шахагдах, муруйлттай хэсэгт өвдөлт илрэх, гоо зүйн хувьд галбир алдагдах, дегенератив өөрчлөлтүүд үүсч болно. Congenital scoliosis and kyphosis - төрөлхийн өөрчлөлтүүд нь Нугалам хоорондын үений болон нугаламын өөрийн хэлбэржих үед дутуу хөгжил үүссэнээс block vertebrae, hemivertebra, эсвэл butterfly vertebra үүссэнээс шалтгаалж эмгэг муруйлт үүснэ.
- 59. 1, 2 зурагт , hemivertebrae өөрчлөлтөөс үүссэн сколиоз болон hydrosyringomyelia өөрчлөлт coronal T2-weighted MR зурагт харагдана. Дараагийн зурагт Hemivertebrae өөрчлөлтүүдээс үүссэн олон хэсэгт сколиоз үүссэн байна.
- 60. Scheuermann Disease Оsteochondrodysplasia, Scheuermann –ны өвчин нь өсвөр насны хүүхдийн эмгэг бөхтөрийн голлох шалтгаан юм. Энэ өвчин нь тасралтгүй явагдаж сээрниц кифоз нэмэгдэж, бүсэлхийн лордоз нэмэгдэх ба цээжний нугалам хоорондын зай нарийсч, нугалмуудын их биеэр намсах, Шморлийн зангилаа өөрчлөлтүүд нэмэгддэг. Scheuermann disease – Цээжний нугалам хоорондын зай олон нугаламын түвшинд нарийссан ба Шморлийн зангилаа өөрчлөлтүүд тодорхойлогдоно.
- 61. Гавал болон багана нуруу холбогдох хэсгийн төрөлхийн эмгэгүүд
- 62. Occipitalization of the atlas • Occipitalization of the Atlas – Atlas assimilation – Аман хүзүүний аль нэг хэсэг гавлын хэсэгтэй холбогдох – Аtlanto-occipital fusion – Аман хүзүүний арын сэртэн дагзны хэсэгтэй холбогдох
- 63. Эмнэл зүйн онцлог • Гурвал шинж буюу богино хүзүү, дагзны үсний төгсгөл доошилох, хүзүүний хөдөлгөөн хязгаарлагдах шинжүүд илэрнэ • Шилэн хүзүүгээр өвдөнө. • C1–C2 ба C2–C3 хэсэгт дегенератив өөрчлөлт давамгай үүсдэг • 30-с дээш нас ахих үед зовиур шаналгаа нэмэгддэг.
- 64. Atlas assimilation a. Аман хүзүү урд хэсгээр холбогдсон (zone 1 assimilation). b. Гадна хажуу хэсгээрээ холбогдсон (zone 2 assimilation). с. Аман хүзүү арын хэсгээрээ холбогдсон (zone 3) assimilation.
- 65. Аtlanto-occipital fusion – Аман хүзүүний арын сэртэн дагзны хэсэгтэй холбогдсон
- 70. Vertebralization of the Atlas • Аман хүзүү хатан хүзүүтэй холбогдох эмгэг юм. • Аман хүзүү 2 ш тодорхойлогдох ба бүтэн 2ш байх нь маш ховор аль 1 хэсэг нь заавал дутуу тодорхойлогдоно. • Аман хүзүү урд талаараа гавлын хэсэгтэй(occipitalization), хойд талаараа хатан хүзүүтэй холбогдох (vertebralization) тохиолдол байдаг. • Хөндлөн холбоос дутуу хөгжсөнөөс аман хүзүү хатан хүзүүтэй холбогддог. • The odontoid process уртасч хэлбэр бүтцийн өөрчлөлт үүсдэг.
- 72. Klippel-Feil Anomaly and Syndrome: The Klippel-Feil anomaly нь хүзүүниы ганц эсвэл хэд хэдэн нугалам хоорондын зай арилж хоорондоо нийлдэг эмгэг юм. Гурвал шинж буюу богино хүзүү, дагзны үсний төгсгөл доошилох, хүзүүний хөдөлгөөн хязгаарлагдах шинжүүдээр Klippel-Feil эмгэгийг илрүүлнэ. Sprengel-ийн деформаци буюу (omovertebral bone) багана нурууг дал ястай холбодог нэмэлт яс тодорхойлогдож болно.
- 74. Thank You.
