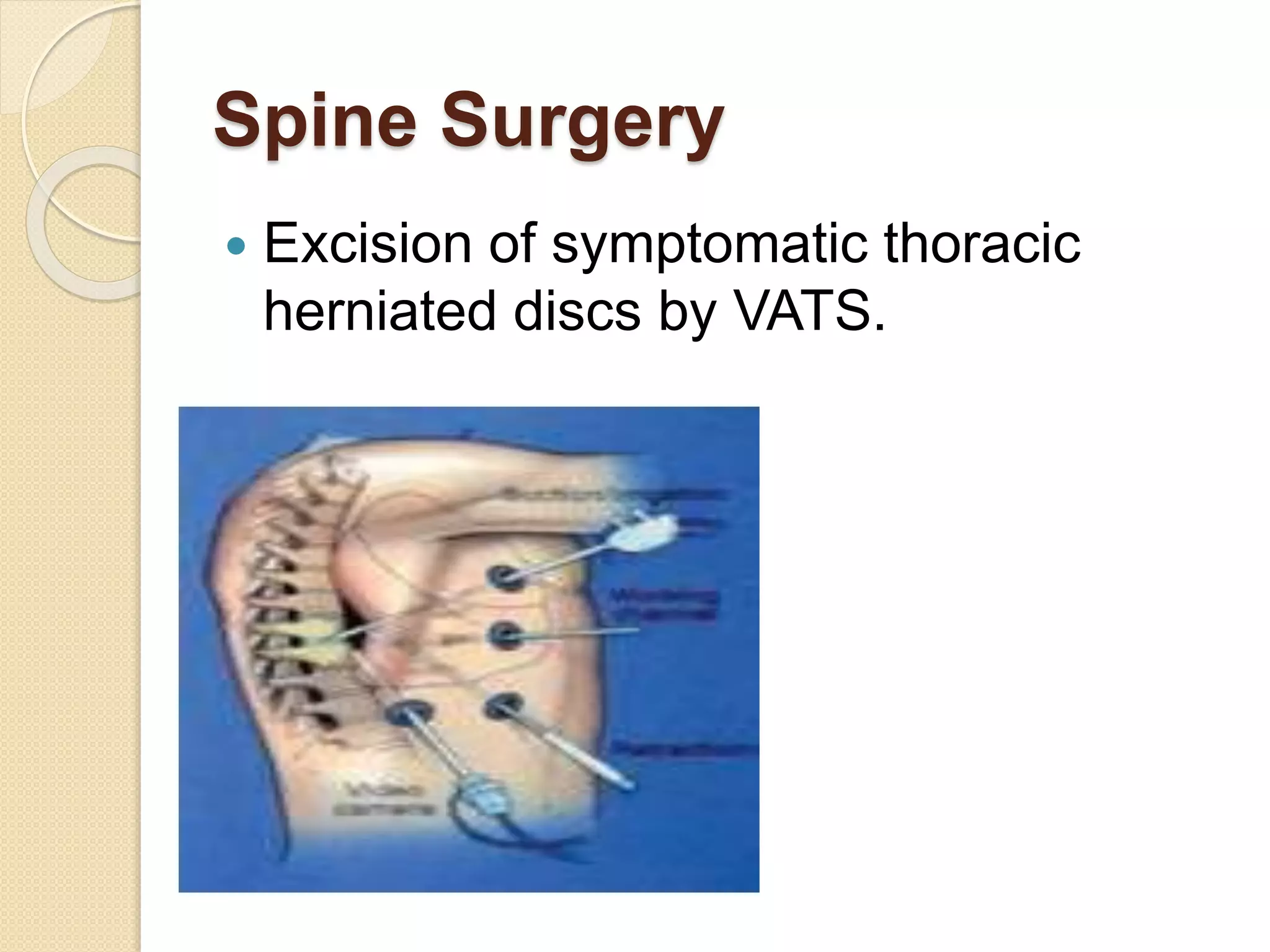
Video Assisted Thoracic Surgery (VATS) is a minimally invasive surgical procedure used to diagnose and treat illnesses of the lungs and chest cavity. It involves making small incisions between the ribs and inserting surgical instruments and an endoscope to allow internal visualization. VATS is used for diagnostic biopsies, treatment of conditions like empyema, bullous lung disease, and resection of lung nodules and tumors. It has advantages over traditional open thoracotomy such as less pain, blood loss, and faster recovery time. The document outlines the history, techniques, and many applications of VATS for pulmonary, pleural, mediastinal, and other chest diseases and procedures.