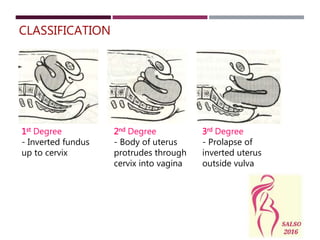
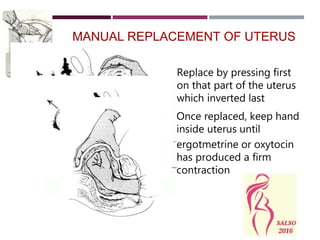
Uterine inversion occurs when the uterus turns inside out, most commonly during delivery from excessive cord traction or fundal pressure. It has an incidence of 1 in 2000 deliveries. Uterine inversion can be first, second, or third degree depending on how far the uterus prolapses. Symptoms include abdominal pain, postpartum hemorrhage, and shock. Treatment requires prompt recognition and replacement of the inverted uterus manually or with hydrostatic pressure before detaching the placenta, as well as treatment for shock. Prevention focuses on controlled cord traction and avoiding fundal pressure until after placental separation.