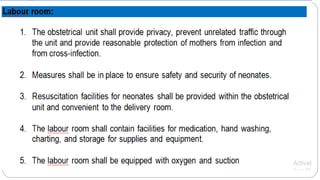
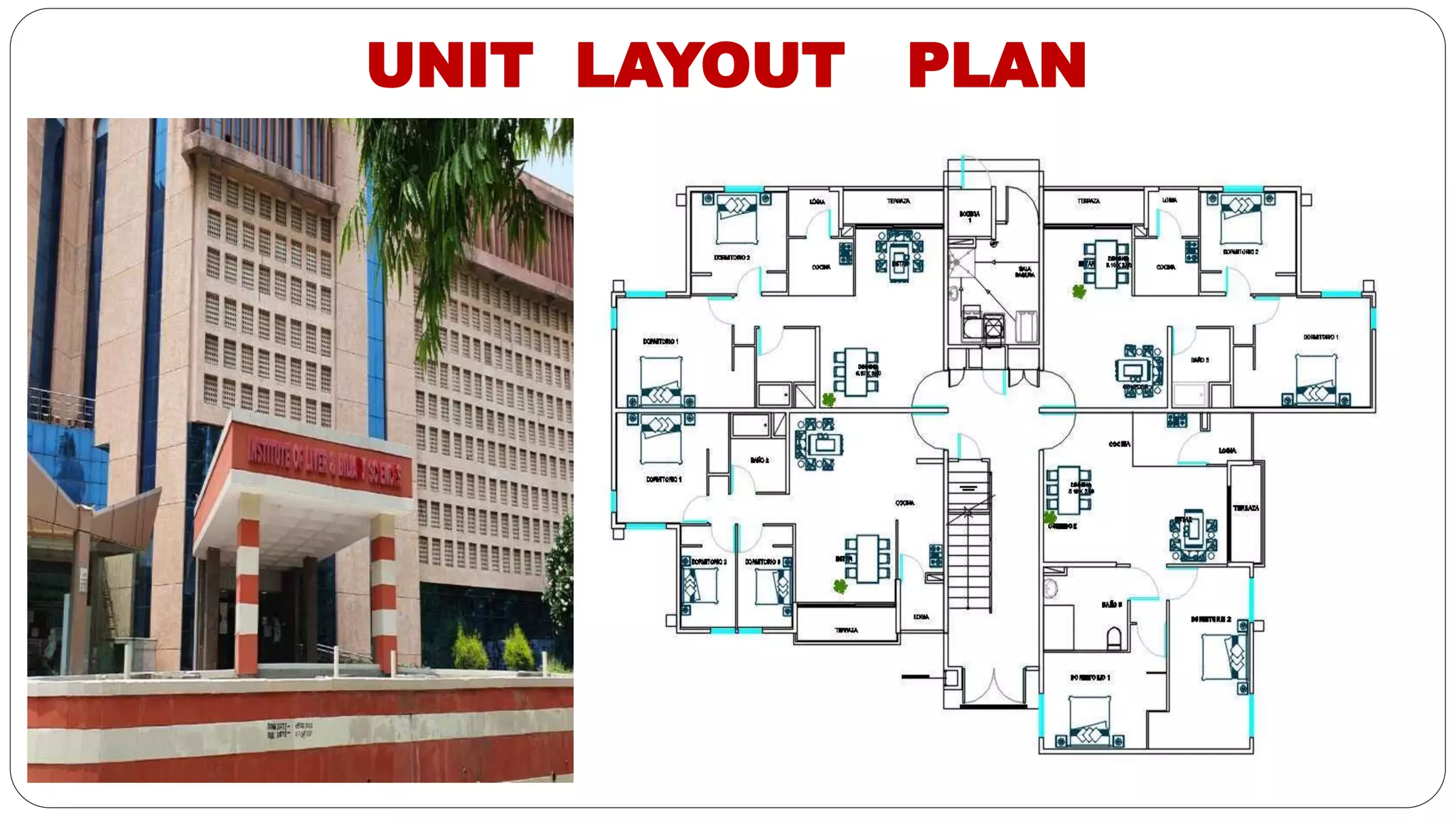
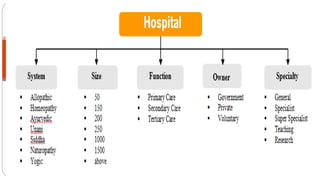
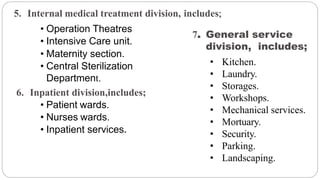
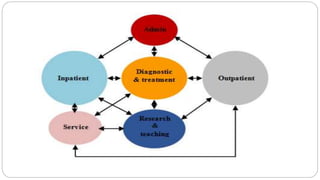
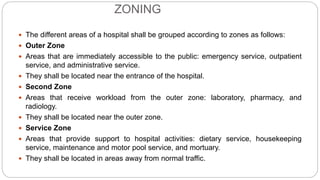
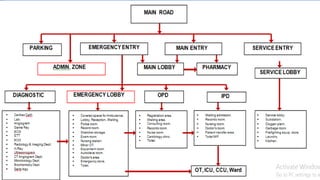
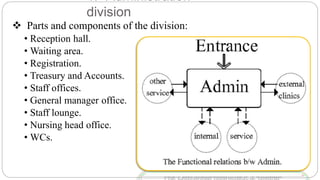
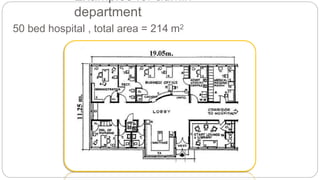
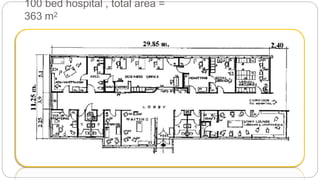
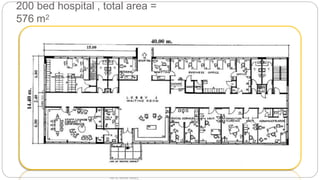
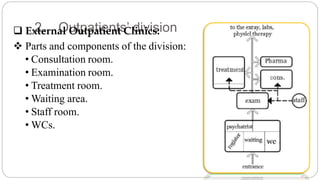
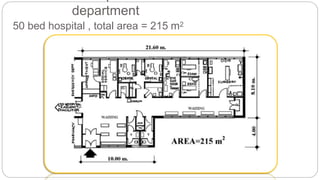
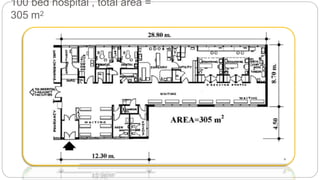
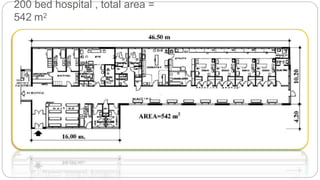
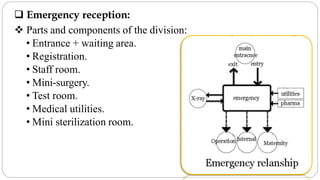
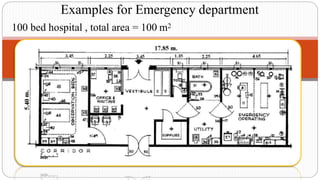
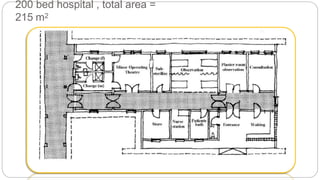
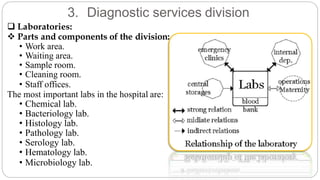
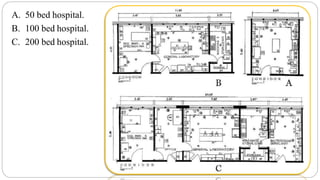
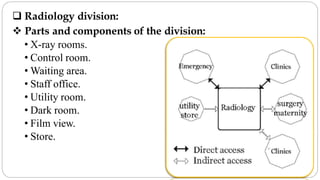
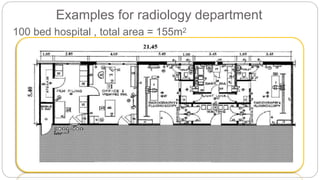
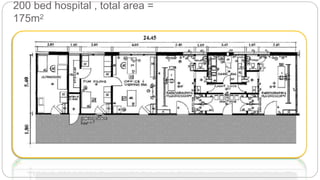
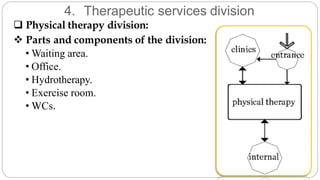
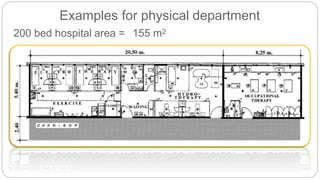
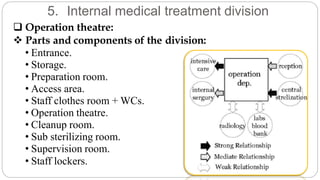
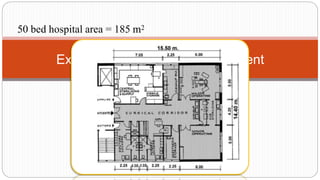
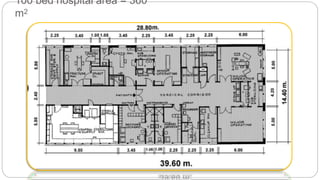
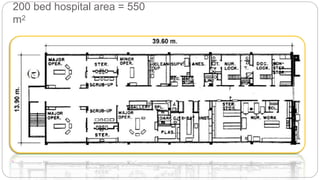
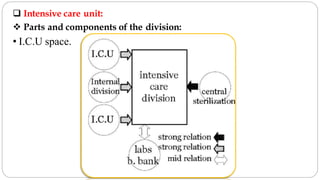
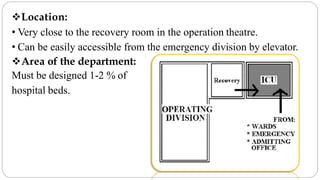
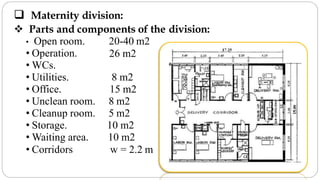
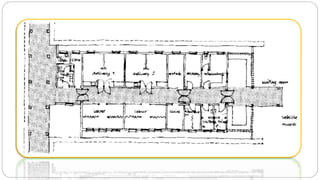
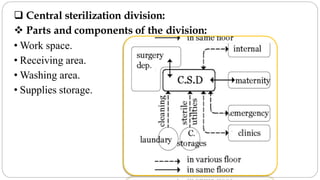
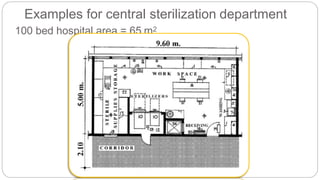
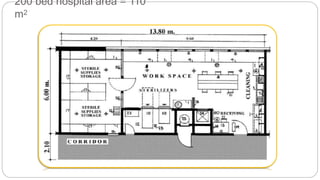
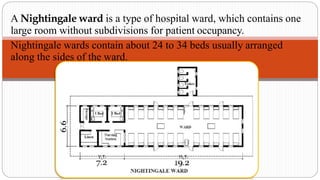
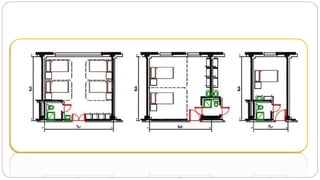
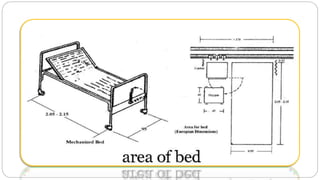
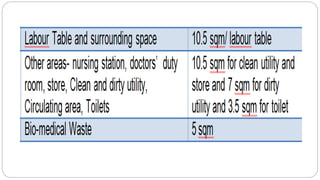
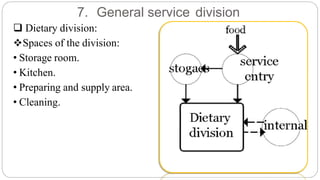
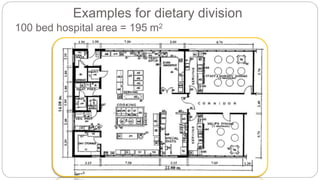
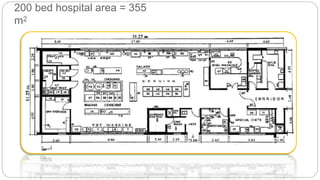
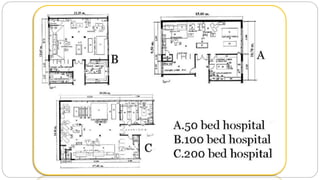
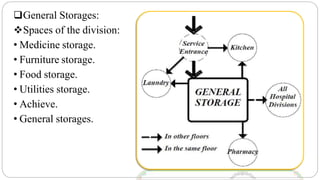
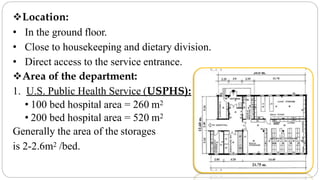
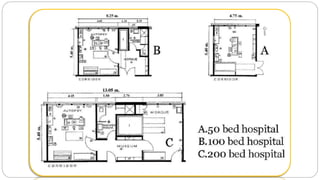
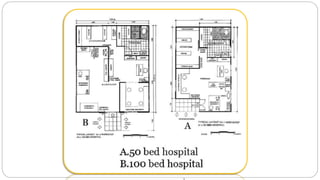
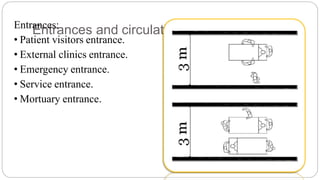
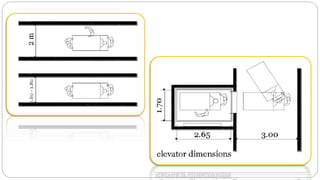
This document outlines the layout plan and design considerations for a hospital unit. It discusses the key divisions of a hospital including administration, outpatient care, diagnostic services, inpatient wards, and general services. For each division, it identifies the main components and provides guidance on location and typical space requirements based on hospital size. Zoning principles and types of circulation within the hospital are also covered. Design factors such as flexibility, accessibility, and future expansion are emphasized.