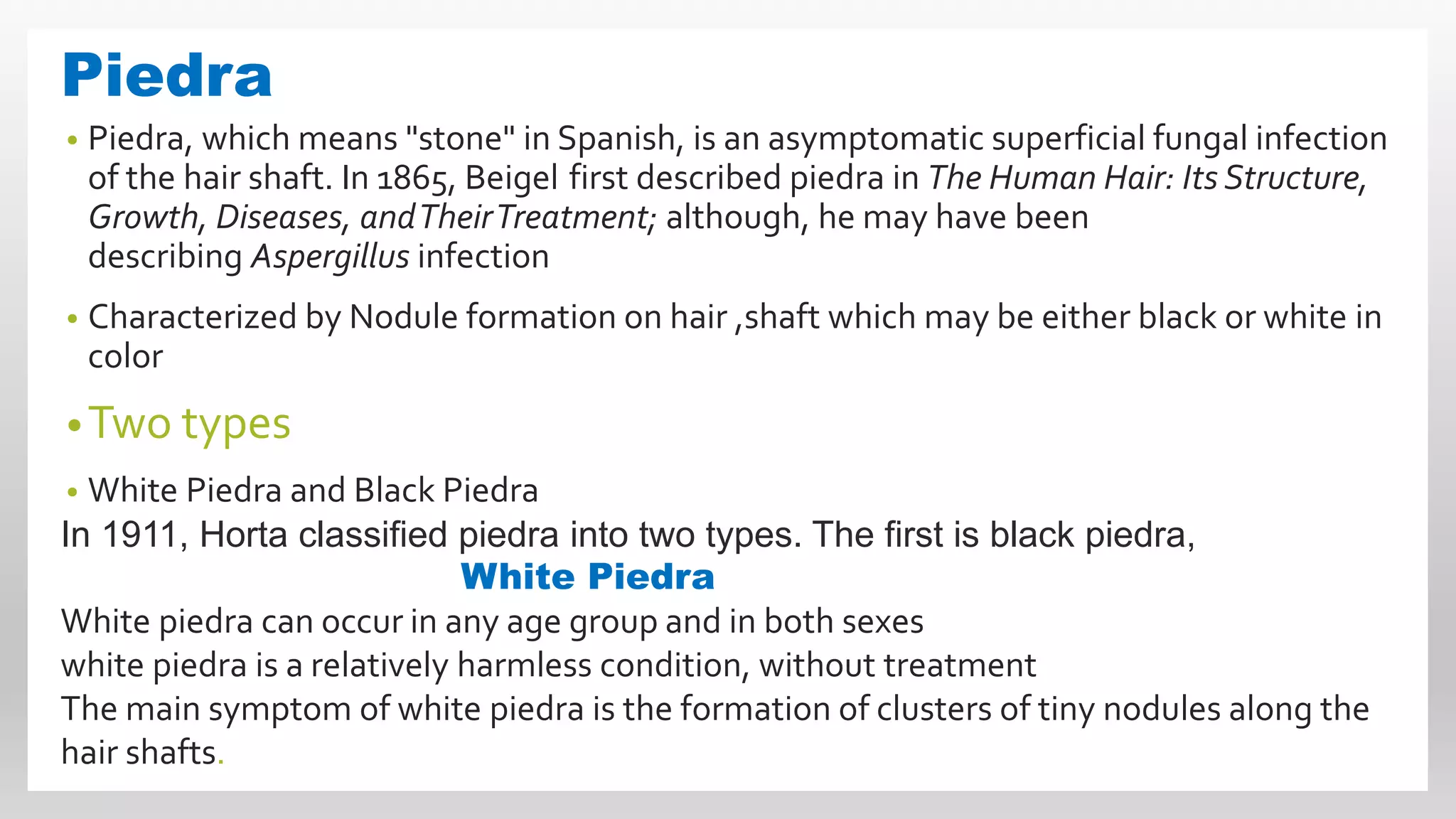
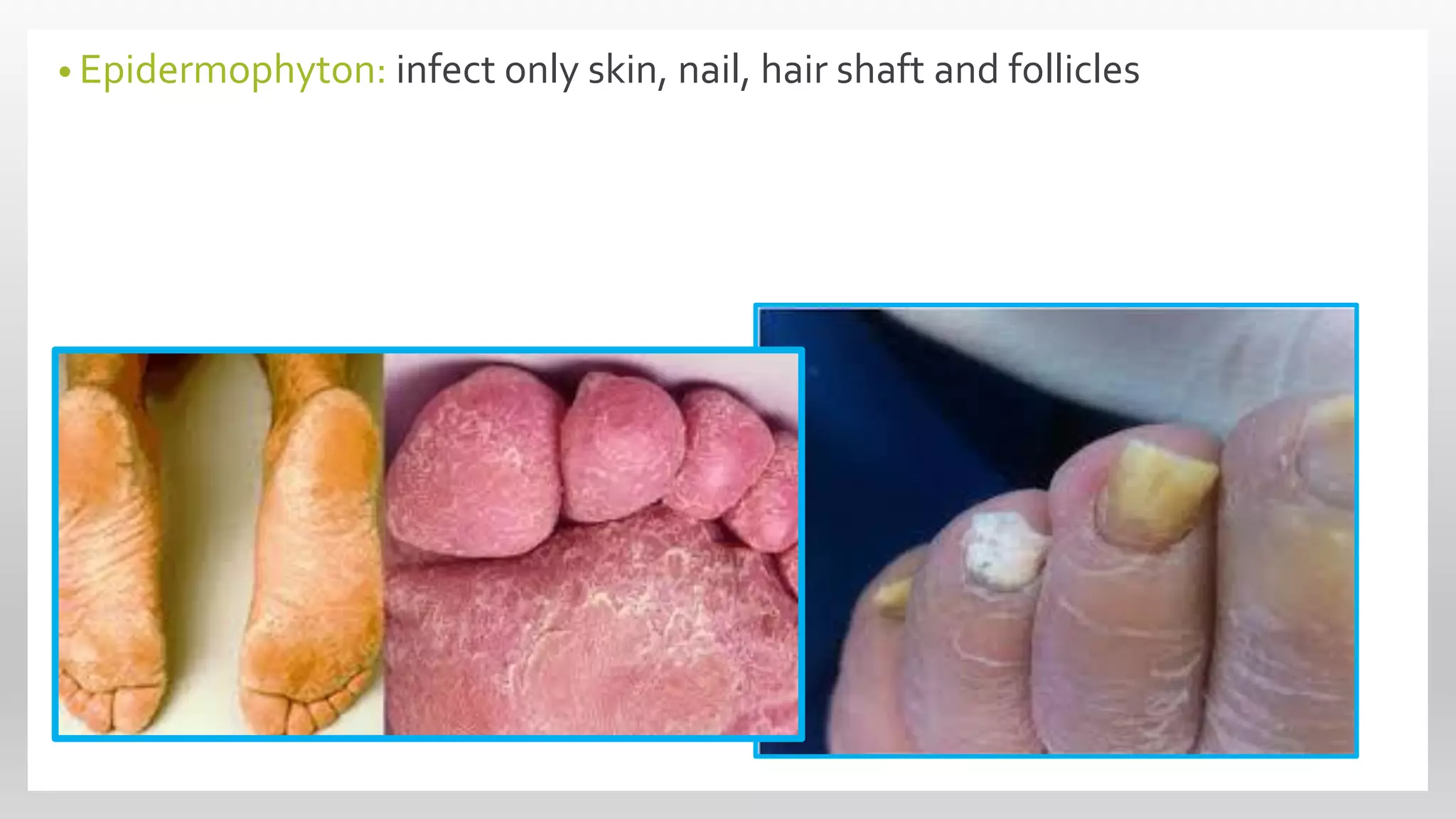
This document discusses superficial mycoses, a type of fungal disease, detailing various classifications including ascomycota, basidiomycota, and dermatophytes. It describes specific conditions like tinea versicolor, tinea nigra, and piedra, including their causes, symptoms, and the fungi responsible for them. Additionally, it provides information on dermatophytes and their subcategories, which can infect skin, hair, and nails through direct contact.