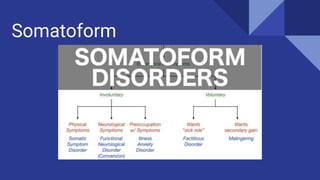
Somataform Disorders in AP Psych Curriculum
- 1. Somatoform
- 2. Symptoms Conversion Disorder ● Weakness or paralysis. ● Loss of balance or difficulty walking. ● Tremors or seizures. ● Vision problems. ● Hearing problems ● Difficulty speaking or inability to speak. ● Difficulty swallowing. Hypochondria ● Being preoccupied with having or getting a serious disease or health condition ● Having so much distress about possible illnesses that it's hard for you to function ● Repeatedly checking your body for signs of illness or disease ● Frequently making medical appointments for reassurance — or avoiding medical care for fear of being diagnosed with a serious illness ● Avoiding people, places or activities for fear of health risks Somatoform Disorder, Soma meaning body, is when the psychological problems start appearing in the form of bodily symptoms.
- 3. Effects on behavior and Commonality A person with a Somatoform disorder will find themselves experiencing physical and emotional distress. Hypochondria ● Repeatedly checking your body for signs of illness and disease. It can occur in children, adolescents, and adults and it usually begins at the age of 30. People assigned female at birth are 10 times more likely to develop then people assigned male at birth. Conversion ● Severe problems that prevent them from working and doing enjoyable activities.
- 4. The somatic signs of somatoform disorders are factual. They include psychological origins as a replacement for corporal causes. The symptoms frequently resemble symptoms of severe medical disorders. Whereas emotional influences cause psychosomatic illness. Ricky Bobby
- 5. Heritability You can get Somatoform disorder either environmentally or biologically. While genetics may play a role in the development of these disorders, environmental factors may play an even bigger role. ● Recent significant stress or emotional or physical trauma. ● Having a mental health condition, such as a mood or anxiety disorder, dissociative disorder or certain personality disorders. ● Having a family member with a neurological condition or symptoms. ● Having a history of physical or sexual abuse or neglect in childhood.
- 6. Case Study Mia is a 15 year old white female. She had flu like symptoms and 2 weeks later, started throwing up blood. She went to ER and was diagnosed with possible appendicitis and was sent home the next day. However, she still felt unwell and admitted herself into a hospital for a few weeks. While admitted, she received extensive workup including MRI, CT scan, gastrointestinal imaging, and a spinal tap, and all the results came back normal. Mia was discharged home with an unknown diagnosis and started on symptomatic medical management to help relieve some of the symptoms. Soon after she was discharged from the hospital, her legs started getting weak, and it was discussed that she may be having some neurological disorders and would need to be evaluated further. Presenting with symptoms of throwing up, unable to keep food down, leg numbness, and a constant migraine, Mia was readmitted at the hospital for another two weeks where even more extensive workup was done again, including CT and MRI scans of the brain. All results came back normal, and she was sent home without a true diagnosis and was treated for depression and anxiety. And then later on referred to a Neurologist.The neurologist uncovered that from the age of six to 12 years, Mia experienced two active addicted parents, and she received physical and mental abuse from her father. During that time, she was required to become the head of the household to ensure bills were being paid and that her parents were being taken care of. At the age of 12, her mom received de-addiction treatment for three to four months and has been clean and sober for the past five years. Between the ages of 12 and 13, her parents got divorced, and she moved with her mom.
- 7. Diagnoses based on the DSM-5
- 8. Treatments Psychodynamic: Psychodynamic theory suggests that somatic symptoms present as a response against unconscious emotional issues. According to psychodynamic theorists, provides protection from the anxiety or emotional symptoms and/or conflicts Cognitive: Believe that somatic disorders are a result of negative beliefs or exaggerated fears of physiological sensations. Generally more sensitive, This sensitivity, combined with their maladaptive thought patterns, may lead individuals to overanalyze and interpret their physiological symptoms in a negative light. Behavioral: behaviorists propose that somatic disorders are developed and maintained by reinforcers. More specifically, individuals experiencing significant somatic symptoms are often rewarded by gaining attention from other people Biological: Notably, compared with controls, conversion-disorder subjects showed increased dorsolateral prefrontal cortex activity, decreased hippocampus activity, enhanced connectivity between the amygdala and the supplementary motor area, and increased supplementary motor area and temporo-parietal activity.
- 9. Most effective Treatments - Antidepressant medication can help reduce symptoms associated with depression and pain that often occur with somatic symptom disorder. - Psychotherapy has proven most effective, AKA Cognitive based therapy (CBT) - Examine and adapt your beliefs and expectations about health and physical symptoms ● Learn how to reduce stress ● Learn how to cope with physical symptoms ● Reduce preoccupation with symptoms ● Reduce avoidance of situations and activities due to uncomfortable physical sensations ● Improve daily functioning at home, at work, in relationships and in social situations ● Address depression and other mental health disorders
- 10. More Ricky Bobby
Editor's Notes
- A community based study in Turkey determined that 23% of patients diagnosed with conversion disorder had some form of depressive disorder. Two case-control studies have reported a higher prevalence of depression and anxiety in cases diagnosed with SD compared to healthy controls.