This document discusses a rare case of an anomalous right superior vena cava (RSVC) draining directly into the left atrium. The key points are:
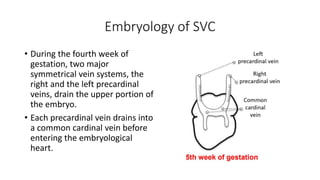
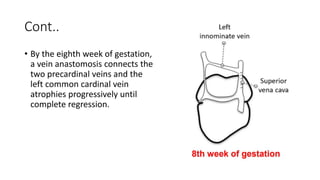
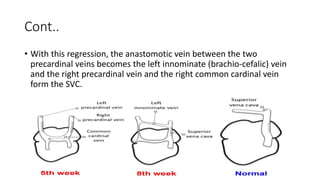
1. Embryological development explains how the RSVC could anomalously connect to the left atrium.
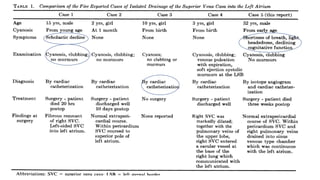
2. A 34-year-old woman presented with hypoxemia and was found to have this rare condition.
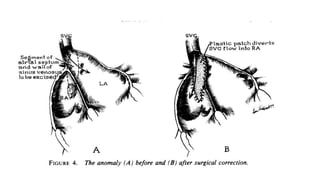
3. Surgical correction was performed to reroute the RSVC into the right atrium, resolving the hypoxemia.