The document discusses pathological calcification, defining it as the deposition of calcium salts in tissues other than osteoid and enamel, and detailing its types: dystrophic, metastatic, and calcinosis cutis. Dystrophic calcification occurs in dead or degenerated tissues, while metastatic calcification happens in normal tissues due to increased serum calcium levels. The document includes details on morphology, etiopathogenesis, clinical features, and a clinical case example for further understanding.



![PATHOLOGICAL [HETEROTOPIC] CALCIFICATION
DEFINITION & TYPES
DEFINITION:
Deposition of Calcium salts in tissues other than osteoid &
enamel
TYPES [common]:
• DYSTROPHIC - deposition in dead & degenerated tissue
• METASTATIC– deposition in normal tissue
• CALCINOSIS CUTIS – deposition of calcium in skin](https://image.slidesharecdn.com/pa2-200808095051/75/PATHOLOGICAL-CALCIFICATION-4-2048.jpg)
![PATHOLOGICAL [HETEROTOPIC] CALCIFICATION
TYPES
TYPES [uncommon]
• In some cases it starts in a single cell, around which
concentric layers of calcium & minerals are deposited to give
lamellated sand like appearance – psammoma bodies
• In asbestosis, calcium & iron salts deposit along asbestos
spicules creating beaded dumbbell shapes](https://image.slidesharecdn.com/pa2-200808095051/75/PATHOLOGICAL-CALCIFICATION-5-2048.jpg)
![PATHOLOGICAL [HETEROTOPIC] CALCIFICATION
MORPHOLOGY
Irrespective of type of pathological calcification, the
morphology remains same
GROSS
• Presents as firm to hard whitish areas, which are gritty to
cut
MICROSCOPY
• Shows deep blue granular irregular material, may be
intra/extra cellular
SPECIAL STAIN – von Kossa – black color, alizarin red - red](https://image.slidesharecdn.com/pa2-200808095051/75/PATHOLOGICAL-CALCIFICATION-6-2048.jpg)

![DYSTROPHIC CALCIFICATION
PATHOGENESIS: INITIATION & PROPAGATION
• Intracellular accumulation of Ca in mitochondria of dead &
dying cells, as well as in membrane bound vesicles (acidic
phospholipids in mitochondria & vesicles attract Ca)
• Phosphatases lead to accumulation of phosphates
• Ca and phosphates interact to form crystals [increased by
osteopontin, collagen & Decreased by mineral inhibitors]
• Cellular membranes rupture & release the crystals outside
the cells (extra cellular)](https://image.slidesharecdn.com/pa2-200808095051/75/PATHOLOGICAL-CALCIFICATION-8-2048.jpg)




![CALCINOSIS CUTIS
DEFINITION
Calcification occurring in skin [dermis] & subcutaneous tissue
ETIOLOGY
• Idiopathic [most cases]
• Sometimes due to dystrophic calcification associated with
immunological connective tissue diseases, eg, systemic
sclerosis [CREST syndrome]
• Infrequently as part of metastatic calcification](https://image.slidesharecdn.com/pa2-200808095051/75/PATHOLOGICAL-CALCIFICATION-13-2048.jpg)
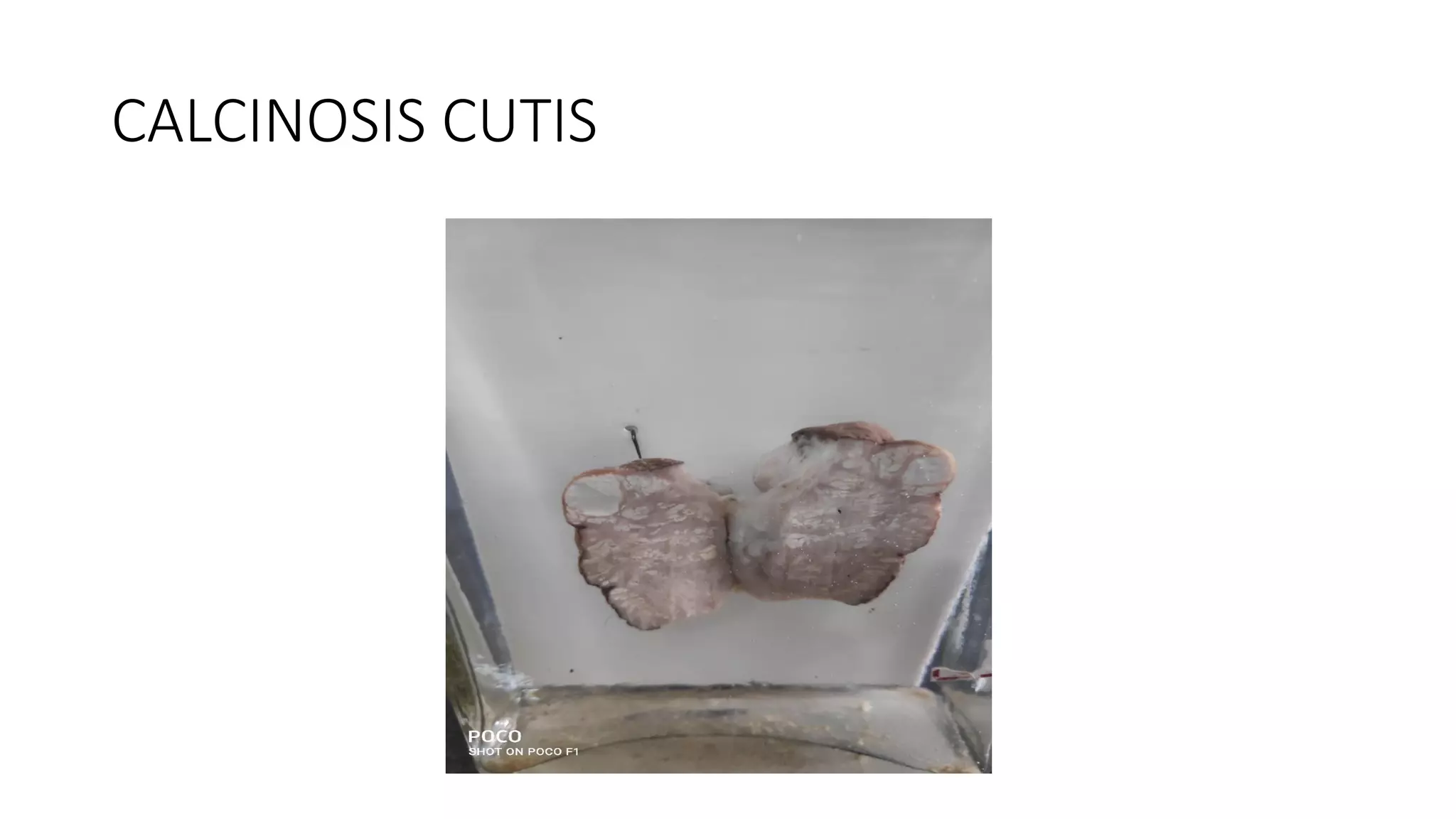
![CALCINOSIS CUTIS
GROSS:
• Most common in skin [dermis] & subcutaneous tissue of
scrotum and around iliac crests
• Skin appears nodular
• Seen as chalky white areas closely related to skin
• Cuts firm to hard with gritty sensation](https://image.slidesharecdn.com/pa2-200808095051/75/PATHOLOGICAL-CALCIFICATION-14-2048.jpg)




![CALCINOSIS CUTIS
CLINICAL FEATURES
• Initially asymptomatic hard nodules [ D/D neoplasia]
• Later may ulcerate, discharge chalky white contents
• Other symptoms may be present according to etiology](https://image.slidesharecdn.com/pa2-200808095051/75/PATHOLOGICAL-CALCIFICATION-20-2048.jpg)
