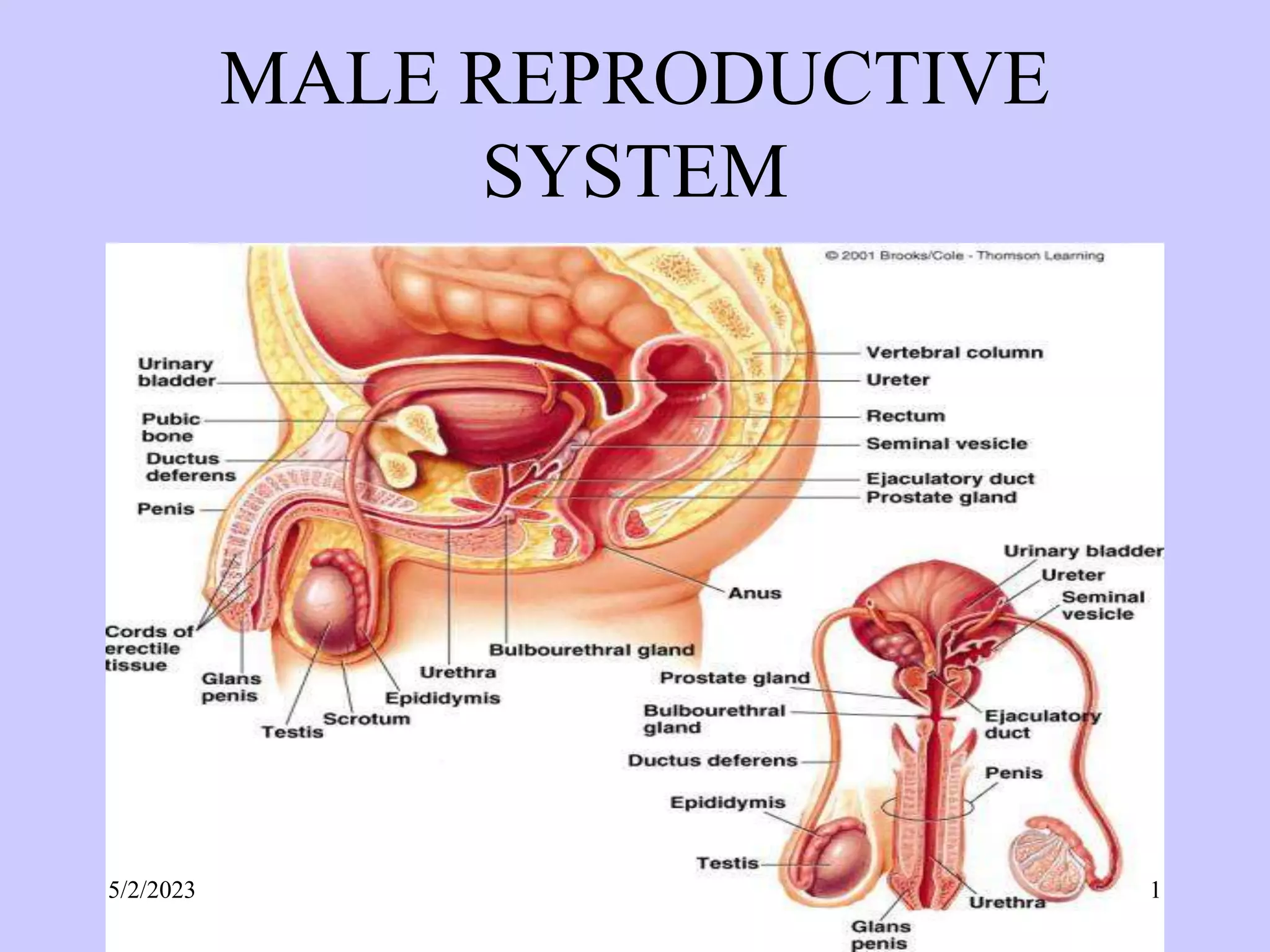
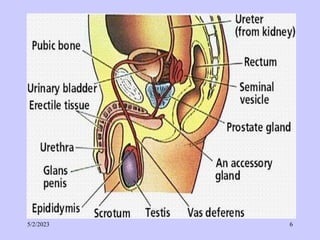
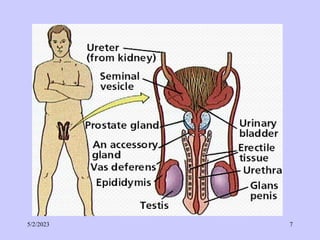
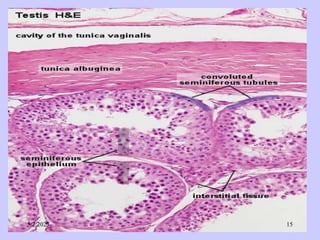
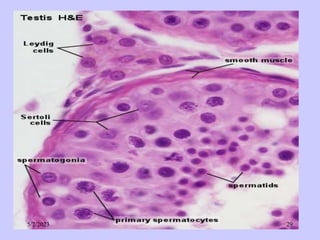
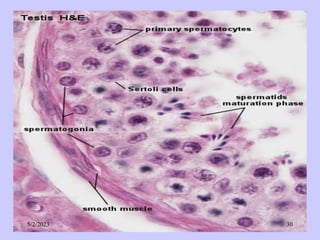
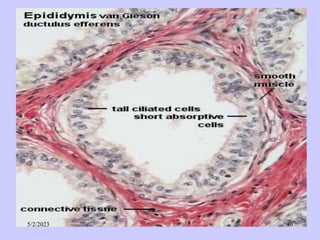
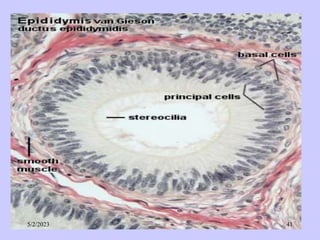
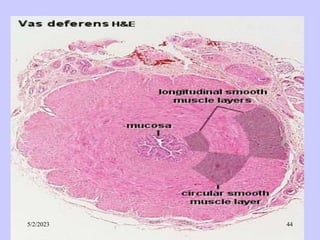
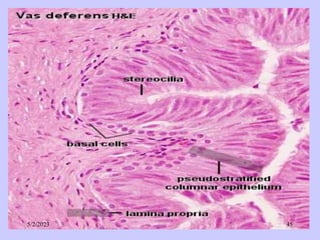
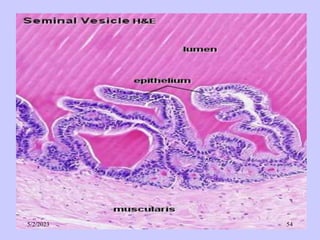
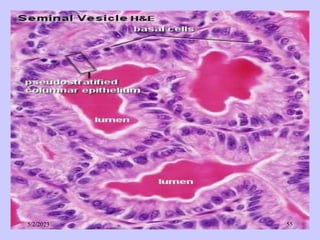
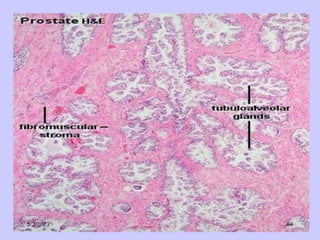
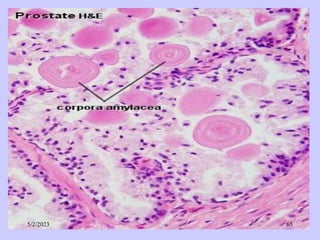
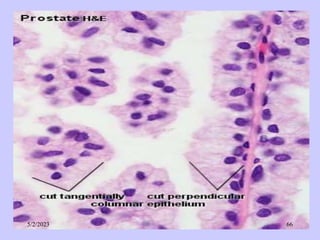
The document provides details about the male reproductive system. It describes the testes, duct system, and accessory sex glands. The testes produce sperm and hormones. Sperm develop through spermatogenesis within the seminiferous tubules of the testes. The duct system includes the rete testis, efferent ducts, epididymis, vas deferens, and ejaculatory duct. The accessory sex glands are the seminal vesicles, prostate gland, and bulbourethral glands. The seminal vesicles secrete fluids that provide energy for sperm.