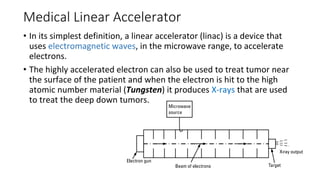
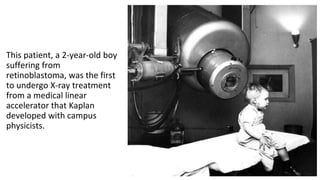
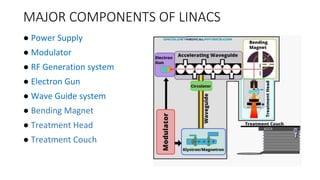
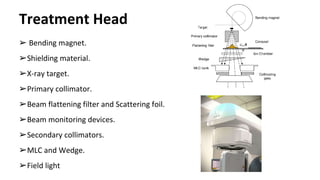
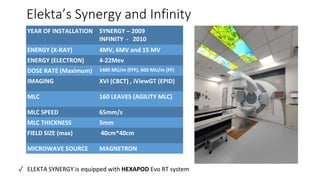
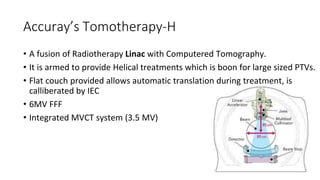
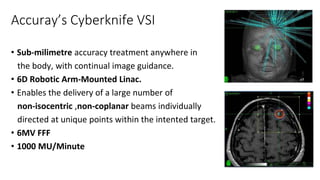
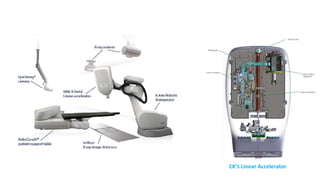
A linear accelerator (linac) is a device that uses electromagnetic waves to accelerate electrons, which are then used to produce x-rays for radiation therapy. The key components of a linac include an electron gun to generate electrons, a waveguide to accelerate the electrons using microwaves from a klystron or magnetron, and a treatment head where the electrons strike a target to produce x-rays. Linacs are used in radiation therapy to treat cancer patients due to their ability to precisely deliver targeted x-ray doses. Modern linacs also incorporate technologies like IMRT and IGRT to further improve treatment accuracy and sparing of healthy tissues.