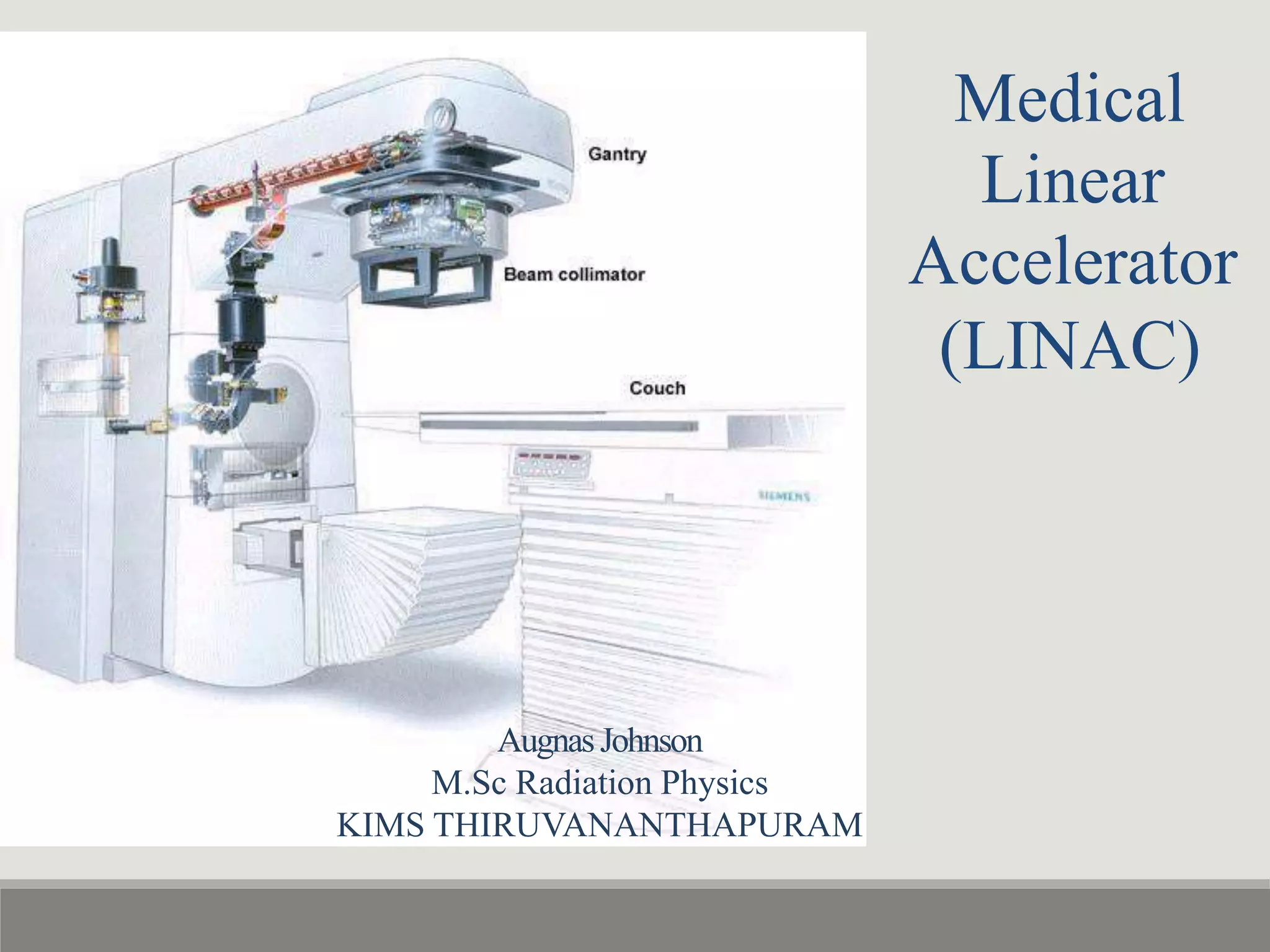
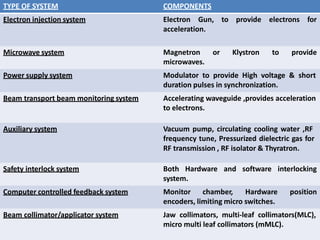
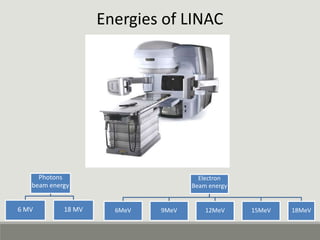
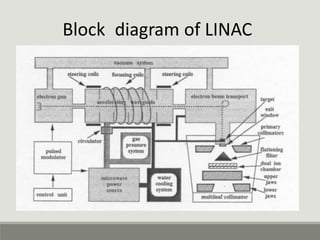
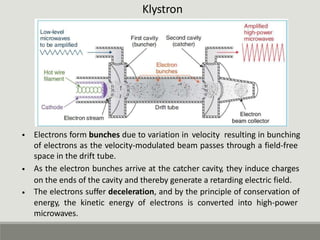
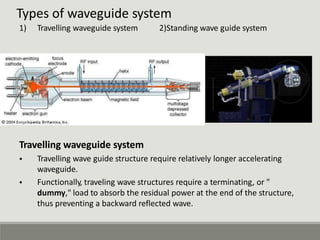
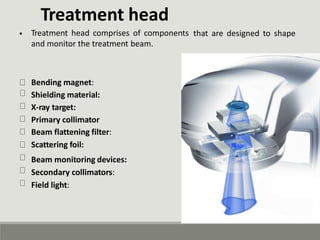
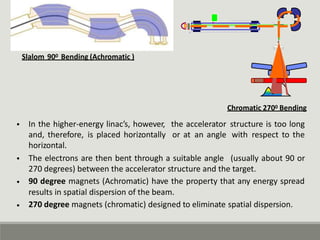
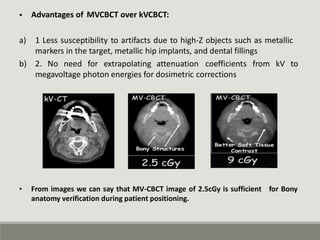
The document summarizes a medical linear accelerator (LINAC). It describes how a LINAC works by using high-frequency electromagnetic waves to accelerate electrons and produce x-rays. It then discusses the history and development of LINACs from the first installation in 1952 to modern machines. Key components of a LINAC are also outlined, including the electron gun, magnetron/klystron, waveguide, and treatment head.