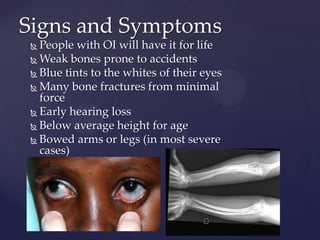
Osteogenesis imperfecta is a genetic disorder caused by a defect in the collagen gene that results in brittle bones that break easily from minor stress or trauma. There are four main types of OI that vary in severity from very mild to lethal in infancy. While there is no cure for OI, treatments focus on increasing bone strength through bisphosphonates and low-impact exercise, as well as surgery to repair broken bones. People with OI must manage their condition for life through precautions to avoid further fractures.