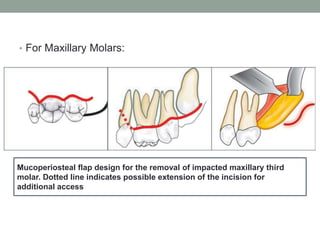
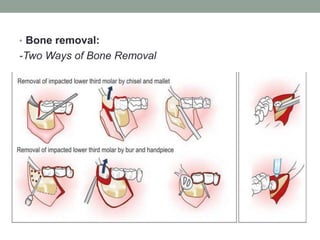
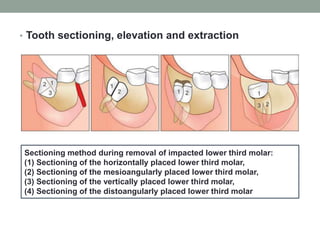
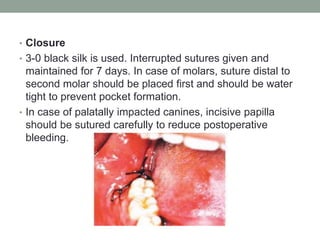
The document provides an in-depth overview of impacted teeth, including definitions, frequency, theories of impaction, etiology, indications and contraindications for removal, classifications, and management strategies for impacted canines. It details various classifications of impaction, such as Winter's classification and Pell and Gregory's classification, and discusses the radiological examinations used for diagnosis. Surgical management protocols for impacted teeth are also outlined, emphasizing the importance of careful planning and consideration of individual patient circumstances.





![2. Nodine’s Phylogenic theory (Nodine 1943) [More-
functional masticatory force – better the
development of the jaw]:
• Nature tries to eliminate the disused organs. This causes
elimination of the unused teeth which causes congenital
absence of third molars. It is also known that in about
10% of the Caucasian race, third molars are lacking, as
the mandible and maxilla decreased in size leaving
insufficient room for third molars i.e., used makes the
organ develop better, disuse causes slow regression of
the organ. Due to changing nutritional habits, our
civilisation have practically eliminated needs for large
powerful jaws, thus, over centuries the mandible and
maxilla decreased in size leaving insufficient room for
third molars.](https://image.slidesharecdn.com/impactedteeth-200722052657/85/Impacted-teeth-7-320.jpg)