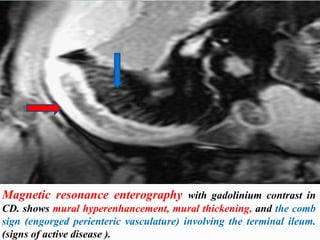
This document summarizes inflammatory bowel disease (IBD), including ulcerative colitis and Crohn's disease. It covers the definition, epidemiology, etiology, pathology, diagnosis, and treatment. Diagnosis involves clinical evaluation, laboratory tests, endoscopy, and radiological imaging. Disease activity is assessed using several clinical indices. Treatment focuses on inducing remission of active IBD.