Embed presentation
Download as PDF, PPTX
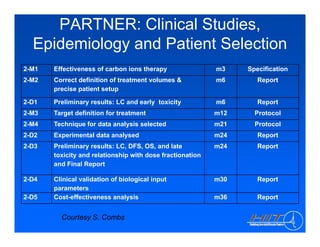
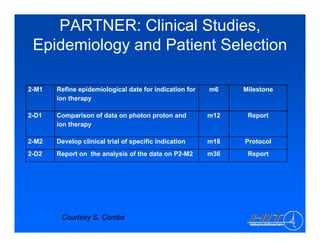

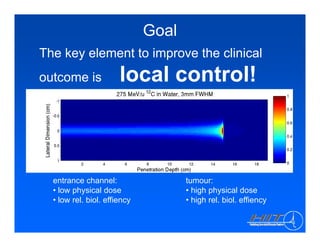

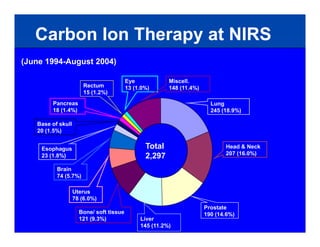

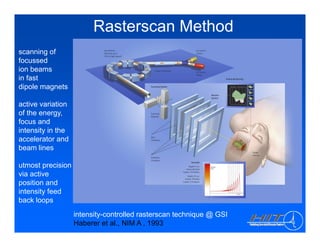

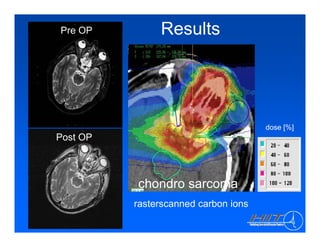
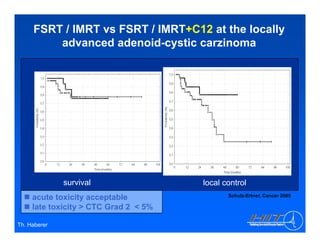
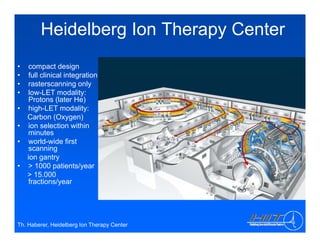


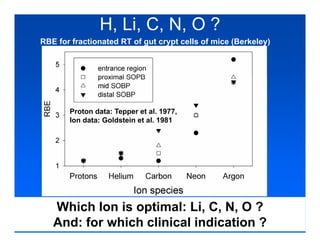


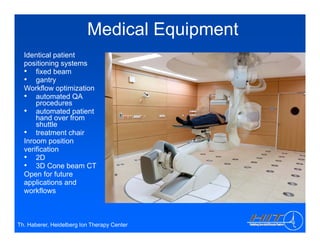








The document discusses ion beam therapy and the Heidelberg Ion Therapy Center. Some key points: 1) The Heidelberg Ion Therapy Center will provide carbon and proton ion beam therapy using raster scanning technology for precise dose delivery. 2) Clinical studies are underway to evaluate the effectiveness of carbon ion therapy for various cancers and determine optimal treatment protocols. 3) The center is scheduled to treat its first patient in early 2009 and will have the capacity to treat over 1,000 patients per year.






























