Ghostdogg productions present ~ alphabet pattern strabismus online version
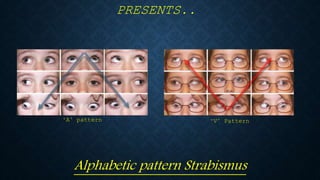
- 1. PRESENTS.. Alphabetic pattern Strabismus ‘A’ pattern ‘V’ Pattern
- 2. DEDICATED TO... • Dr. Burton J. Kushner, MD. • Your interest in this subject of Binocular vision & Strabismus is what has kept me interested and enjoying doing what I do... A. J. Hamilton
- 3. HISTORY OF AV PATTERN STRABISMUS • Originally described as “an abnormal variation in the angle of horizontal strabismus in vertical gaze” by Alexander Duane in 1897. • Later labelled as “Horizontal strabismus with associated vertical elements” from 1896-1956. • First official series of papers with emphasis on the measurement of horizontal deviation in vertical gaze was penned by Uretts-Zavalia in 1948, in his papers “Abducción en la elevación” and “Paralisis bilateral congenita del musculo oblicuo inferior”. Attention was also made to the point that overaction and subsequently underaction of the oblique muscles were in fact associated with increased and decreased convergence or divergence. • By the late 1950’s, the syndrome was officially given the title of ‘A’ or ‘V’ Pattern strabismus, by Dr. D. G. Albert and F. D. Costenbader in 1955 and 1957 respectively, owing to both ‘A’ and ‘V’ patterns being the most commonly noticed forms. The name was then shortened to ‘A-V Pattern Strabismus’ as it stands today. • The syndrome as a whole falls under the Strabismus sub-group of ‘Complex strabismus’ or ‘comitant horizontal/vertical deviations in Strabismus’
- 4. INCIDENCE OF AV PATTERN STRABISMUS • 15-25% of cases of pediatric strabismus occur with A/V Pattern Strabismus as a subsidiary symptom associated with most common forms of Strabismus: Brown’s Syndrome, Duane’s retraction Syndrome, or any association with any form of over/underaction of the Superior/Inferior obliques • A/V Pattern Strabismus is the most common form of Infantile Strabismus. • While ‘A’ Pattern is perhaps the most common, ‘V’ Pattern in either esotropia or exotropia is quite prevalent in both pediatric and adult strabismus categories. • Other rarer forms such as ‘X’ pattern, Lambda pattern, and ‘Y’ pattern strabismus have also been documented and seen; Lambda pattern being a sub-group of ‘A’ pattern, while ‘Y’ pattern is more closely associated with ‘V’ pattern. ‘X’ pattern to date remains a group of its own, since so little is still unknown of this sub-type. • These special forms of incomitance in vertical gaze consist of nothing more than modifications of the classic A or V patterns; therefore,they should not be regarded as separate entities.
- 5. COMMON FORMS OF AV PATTERN STRABISMUS
- 6. ‘A’ PATTERN STRABISMUS ‘A’ PATTERN ESOTROPIA • An A pattern is present when a horizontal deviation shows a more convergent (less divergent) alignment in upgaze compared with downgaze. • An ‘A’ pattern is considered significant if the difference between upgaze and downgaze is ≥10 Δ. • Patients with ‘A’ pattern esotropia will show on clinical presentation: • An increase of the esotropia in midline upgazes, and a decrease of the esotropia on midline downgazes • The eyes will be mostly straight in Primary gaze and direct downgaze • Patients will adopt a chin-up head posture to compensate for single binocular vision. • An ‘A’ Pattern is often associated with: • Primary superior oblique overaction • Inferior oblique underaction/palsy with subsequent superior oblique overaction. • Inferior rectus underaction
- 7. ‘A’ PATTERN ESOTROPIA This 6-year-old girl presents with a evident ‘A’ pattern Esotropia associated with a right superior oblique overaction, visible as an overshoot of the right eye on adduction. Noticeable is the child’s assumed chin-up head tilt to the left to compensate for single binocular vision in primary gaze. Also evident is the convergence of the eyes on direct upgaze, hence an ‘A’ pattern.
- 8. ‘A’ PATTERN STRABISMUS ‘A’ PATTERN EXOTROPIA • In cases of an ‘A’ pattern exotropia, the deviation of the eyes is more pronounced as the eyes move more towards midline downgaze rather than midline upgaze. • There is an evident divergence of the eyes in direct downgaze, with the eyes ‘splaying outwards’. • Like in ‘A’ pattern esotropia, a patient’s eyes in primary and upgaze will often look straight, and work together closely to normal. ‘A’ pattern exotropia is much more prevalent in midline downgazes, rather than upgaze. This misalignment is often not noticed by parent’s whose children have this form of strabismus. • Similar again to an ‘A’ pattern esotropia, patients will often assume an abnormal head posture, except that it will be a chin-down, head turn, again allowing the patient to achieve single binocular vision in primary gaze.
- 9. Mongoloid feature - On upgaze, the eyes converge inward -In Primary position eyes are slightly exotropic - On downgaze, the eyes diverge outward “A” PATTERN EXOTROPIA:
- 10. ‘A’ PATTERN EXOTROPIA This 20-year-old girl shows a visible ‘A’ pattern exotropia associated with overaction of her right superior oblique, most evident in down and left, and down and right gazes. In primary gaze she adopts a chin-down head turn away from the affected eye, in order for both her eyes to fuse in single binocular gaze. In direct downgaze there is a visible ‘outward splaying’ of both eyes. The exotropic deviation is minimal to normal in all upgazes.
- 11. ‘V’ PATTERN STRABISMUS ‘V’ PATTERN ESOTROPIA • First described by Alexander Duane in 1897 when he described a patient with bilateral superior oblique palsy • Patients with a ‘V’ pattern esotropia, as similar to ‘A’ pattern, will show a definite increase of horizontal deviation more so in downgaze, with a corresponding decrease of the deviation in upgaze. • The inferior oblique is an abductor also, and secondary or primary overaction of that muscle will result in a relatively less convergent or more divergent position in upward gaze, producing a V pattern.
- 12. Anti-mongoloid feature - Upgaze eyes diverge outwards - Primary position eyes are evidently esotropic -Downgaze eyes converge inwards “V” PATTERN ESOTROPIA:
- 13. ‘V’ PATTERN ESOTROPIA This 6 ½ year old boy shows a very apparent ‘V’ pattern esotropia, made evident by the extreme chin-down head posture, which he has adopted in order to fuse in primary position. Evident also is the apparent ‘upshoot’ of his left eye on adduction, and apparent ‘overshoot’ on elevation in adduction, causing both his eyes to ‘splay outwards’, also evident on direct upgaze. This is a result of an evident overation of his left inferior oblique. On direct downgaze, his eyes seem to work in tandem almost normally.
- 14. ‘V’ PATTERN STRABISMUS ‘V’ PATTERN EXOTROPIA • In cases of a ‘V’ pattern exotropia, the deviation of the eyes is more pronounced as the eyes move more towards midline upgaze rather than midline downgaze. • There is an evident divergence of the eyes in direct upgaze, with both eyes “splaying outwards”. • Overaction of the Inferior oblique can be quite apparent in an evident “upshoot” of the globe on adduction. • Similar again to an ‘A’ pattern esotropia, patients will often adopt an abnormal head posture, except that it will be a chin-up head turn. This allows the patient to achieve single binocular vision in primary gaze. Parents of children with a ‘V’ pattern will often notice that their child will occasionally ‘tilt’ their head upwards, to bring their eyes to an downward position in order to achieve binocular vision in primary gaze.
- 15. ‘V’ PATTERN EXOTROPIA This 7-year-old girl presents with an evident ‘V’ pattern esotropia, clearly shown by the chin-up head posture which she has adopted in order to obtain single binocular vision in primary gaze. Evident is the significant overaction of her left inferior oblique in the form of a gross overshoot of her left eye in adduction and elevation in adduction. Also significant is the quite evident “outwards splaying’ of both her eyes in direct upgaze. Note the horizontal deviation is significantly less noticeable in downgazes, and more so in upgazes, hence a ‘V’ pattern.
- 16. RARER FORMS OF AV PATTERN STRABISMUS
- 17. ‘A’ PATTERN “LAMBDA” STRABISMUS This young girl shows a definitive λ pattern, a variant of an ‘A’ pattern exotropia, associated with a bilateral superior oblique overaction. As with an ‘A’ pattern exotropia, she adopts a chin-down head posture in primary. Note that the divergence is only manifested most in downgaze to her right. The divergence is evident by the ‘outward splaying’ of both her eyes on downgaze right, and direct downgaze. As with an ‘A’ pattern exotropia, there is a definite convergence of her eyes on direct upgaze.
- 18. ‘X’ PATTERN STRABISMUS • Patients with ‘X’ pattern often present with a visible exotropia that is only present or evident in direct upward and downward gaze. • They often have little to no horizontal deviation on either adduction, or abduction, with only minimal deviation in primary position. • Most patients will not adopt an abnormal head posture, but will ‘raise’ or ‘dip’ their head, depending on which direction they are needing to visualize, be it upgaze or downgaze, in order to bring both eyes into single binocular vision.
- 19. ‘X’ PATTERN STRABISMUS This boy presents with an ‘X’ pattern strabismus, made evident by that there is a definite divergence of both eyes, shown by the hallmark ‘outward splaying’ of both eyes on both upgaze and downgaze. This is heightened by the fact that he ‘dips’ his head down to bring his eyes “up” on upgaze, and ‘raises’ his head to bring his eyes ‘Downwards” on downgaze. What makes this pattern difficult to distinguish is that there is little horizontal deviation on either adduction or abduction, and that he doesn’t adopt any abnormal head posture in primary.
- 20. ‘Y’ PATTERN STRABISMUS • Like ‘X’ pattern, patients with this form of AV pattern strabismus will only display the deviation of the eye in all gazes above midline gaze. • There is little to no deviation in either primary position or direct downgaze. • This pattern is often hard to distinguish from a bilateral Inferior oblique overaction, but has been documented in the form of ‘Pseudo Y pattern associated with Inferior Oblique overaction’. • The most adopted theory as to the cause for a ‘Y’ pattern is an abberant innervation of the Lateral Rectus in up gaze.
- 21. ‘Y’ PATTERN ANTI ELEVATION SYNDROME • Occurs as a complication of the inferior oblique anterior transposition. This procedure changes the Inferior oblique from being an elevator, which restricts elevation in adduction. • Typically, there is marked fundus extortion associated with this sub-pattern of ‘Y’ pattern strabismus. • Treatment for this usually involves a retroplacement of the anteriorly placed Inferior oblique, thus reverting it to a standard recession.
- 22. ‘Y’ PATTERN ANTI-ELEVATION SYNDROME This teenage boy shows an Anti-elevation pattern following bilateral IO anterior transposition. On looking to his left, what looks like an overelevation of his right eye in abduction, is actually a secondary deviation due to fixation duress. His right (adducted) eye is ‘stuck’ in an elevated and adducted position, due to the IO now having become an anti- elevator., thus restricting its normal rotation
- 23. PSEUDO-INFERIOR OBLIQUE OVERACTION ASSOCIATED WITH ‘Y’ PATTERN STRABISMUS • Described by Dr. Burton J Kushner, Pseudo-inferior oblique overaction occurs in an unusual manner in which patients with this strabismus pattern will demonstrate the general features of a ‘Y’ pattern, but with the addition of an over elevation of the adducting eye in the field of the inferior oblique muscle, resulting in a ‘Y’ pattern with a large evident exotropia in all up gazes. • When compared to a true inferior oblique overaction it is very difficult to distinguish on presentation. It is only by noting the rapid ‘overshoot’ of the adducting eye as it reaches maximum elevation from direct adduction. This rapid overshoot of the adducting eye is best seen in still frames taken from a film of the patient as they look from direct adduction to direct elevation. • A hypertropia only develops after the eyes have passed beyond midline gaze. This hypertropia then reverts to a gross abduction of the adducting eye once it has reached maximum elevation in adduction.
- 24. PSEUDO ‘Y’ PATTERN STRABISMUS A) This teenage girl shows a pseudo-inferior oblique overaction with ‘Y’ pattern exotropia. When viewed in the field of the inferior obliques, it is indistinguishable from a true inferior oblique overaction. In primary and midline gazes there is no overaction of the inferior oblique. B) It is only by breaking down the frame rate to 0.1 second intervals from direct adduction to upgaze in adduction, can one see that there is no ‘outward splaying” of the eyes until she has reached maximum elevation in adduction. B
- 25. GRADING OF OBLIQUE MUSCLE OVERACTION • Grading of oblique muscle overaction in practice is more of measuring the amount by visual interpretation rather than exact science. Most surgeons use a grading scale of 1+ to 4+ overaction. For inferior oblique grading, 1+ overaction means only slight overaction or over elevation in adduction. Grade 4+ means the most overelevation possible. Grades 2+ and 3+ overaction are the two gradations between those extremes.
- 26. GRADING SEVERITY OF OBLIQUE OVERACTIONS
- 27. CAUSES OF AV PATTERN STRABISMUS In Strabismic documentation and presentation, there are three main groups of causes of AV Pattern Strabismus. These are: • Oblique muscle dysfunction • Orbital abnormality, and • Abduction with a large exodeviation
- 28. MANAGEMENT AND TREATMENT OF AV PATTERN STRABISMUS • Of the four main forms of Alphabet pattern strabismus (‘A’, ‘V’, ‘X’ & ‘Y’) each have certain methods of treatment. Some correlate with others while some require more extensive corrective measures.
- 29. AV PATTERN STRABISMUS WITH ORBITAL ABNORMALITY This young boy has Crouzon’s disease with an evident ‘V’ pattern associated with a craniofacial abnormality. Note the ‘upshoot’ and ‘downshoot’ of both eyes as he looks to both his left, in abduction, and right, in adduction. The arrow mark above his left eye is the surgeon’s mark indicating a left ‘V’ pattern exotropia.
- 30. Pre Treatment Evaluation Detailed History Assessment of BCVA – Cycloplegic Refraction and correction – Measurement of angle of deviation in all the 9 positions of gaze for near and far, with and without optical correction Uniocular and binocular motility with particular attention to the oblique muscle dysfunction MANAGEMENT
- 31. TREATMENT • Factors for treatment of A V pattern strabismus are as follows: • When binocular vision is disturbed, as in A exotropia and V esotropia, and the treatment is surgery. • An increase in deviation in downgaze (with A exotropia and V esotropia) may cause discomfort during reading or in near work. • Patients with large A or V patterns usually also have significant corresponding oblique muscle dysfunctions.
- 32. TREATMENT • Bilateral superior oblique weakening can collapse large A patterns up 30−40 PD or more. Bilateral IO weakening is not expected to collapse as large a pattern. • Bilateral inferior oblique weakening can collapse large V patterns when significant IO overaction is present. • In patients with V pattern and IOOA in association with congenital esotropia complex, consideration should be given to performing IO anterior transposition, even if DVD is not obvious. • The A and V patterns can be diminished by horizontal offsets of the vertical rectus muscles. temporal
- 33. TREATMENT TRANSPORTATION OF THE INFERIOR RECTI • Transposition of the inferior recti will expand the closed end of the V pattern by weakening the adduction vector of the inferior recti in downgaze. Transposing the SRs nasally will help close the open end of the V pattern in an exotropic patient and transposing the IRs nasally will help close an A-pattern exotropia. M a l e
- 34. TRANSPOSITION OF THE RECTI TO CORRECT AV PATTERN STRABISMUS • This boy initially presented with a ‘V’ pattern exotropia which is evident by the exotropia of his left eye in primary, and the ‘outward splaying’ of both eyes in direct upgaze. In the second 9-nine gaze diagnostic versions, we see him again following a bilateral lateral rectus recession. Now his eyes are straight in primary position, and there is no evidence of any horizontal deviation in upgaze.
- 35. IN SUMMARY • Treatment of AV Patterns is relatively summed up in this crucial treatment goal: Weaken the Overacting oblique muscles to alleviate the horizontal deviation!!! • IF, there is no oblique dysfunction, treatment can consist of bilateral or unilateral surgery on transpositioning of the horizontal recti muscles. • Regarded as the most recognizable form of Infantile strabismus. • Evidence of any type of horizontal deviation is particularly demonstrated in either direct upgaze, or direct downgaze. • ‘A’ & ‘V’ pattern strabismus accounts for 15-25% of most horizontal strabismus anomalies to date.
- 37. REFERENCES Online references: • The Strabismus Minute: http://www.cybersight.org • Strabismus Summary series: http://www.geocities.ws/sapatney/webavst.htm • McGill University Pediatric & Adult Strabismus: http://www2.medicine.mcgill.ca/strabismus/atlas/patients/atlasNav/atlas.php • A Pattern Esotropia & Exotropia/V pattern Esotropia & Exotropia: https://emedicine.medscape.com/article/1199714-overview & https://emedicine.medscape.com/article/1199825-overview • Pattern Strabismus - Grand Round lectures by Dr. Robert O. Hoffman, John A. Moran Eye care centre, Utah: https://www.youtube.com/watch?v=APjGJ_soPG4
- 38. REFERENCES CON’T Paper references: • Duane A. Isolated paralysis of the ocular muscles. Arch Ophthalmol,1897; 26: 317–34. • Albert DG. Personal Communication. In Parks MM. Annual review: Strabismus. Arch Ophthalmol 1957; 58: 136–60. • Costenbader FD. The “A” and “V” patterns in strabismus. Trans Am Acad Ophthalmol Otolaryngol, 1964; 68: 354–86. • Sharat, S. Parija, S. A-V Pattern Strabismus- A Simplified Approach. Orissa Journal of Ophthalmol 2010; 40-43. • Kushner BJ. Pseudo inferior oblique overaction associated with ‘Y’ and ‘V’ patterns. Ophthalmology 1991; 98: 1500–5.
- 39. REFERENCES CON’T Textbook references: • Rosenbaum, Arthur L., Santiago, Alvina P. Clinical Strabismus management. Principles and Surgical techniques., The Curtis Centre, Philadelphia, Philadelphia, Pennsylvania. W.B. Saunders ,1999. • von Noorden, Gunter K. MD, Campos, Emilio C. Binocular Vision and Motility – Theory and management of Strabismus, 6th edition. Baylor College of Medicine, Houston, Texas, Mosby 2002 • Ellis, George S. At the Crossings – Pediatric Ophthalmology and Strabismus, New Orleans Academy of Ophthalmology, 2004. • Taylor, David MD, Hoyt, Creig S. Pediatric Ophthalmology and Strabismus 4th edition. Elsevier Saunders 2005 • Coats, David K., Olitsky, Scott E. Strabismus Surgery and it’s complications, Springer 2007 • Kanski, Jack J., Bowling, Brad. Clinical Ophthalmology – A Systematic approach, 7th edition. ExpertConsult, Elsevier Saunders, 2011 • Kushner, Burton J. Strabismus – Practical pearls you won’t find in Textbooks. Springer 2017.
