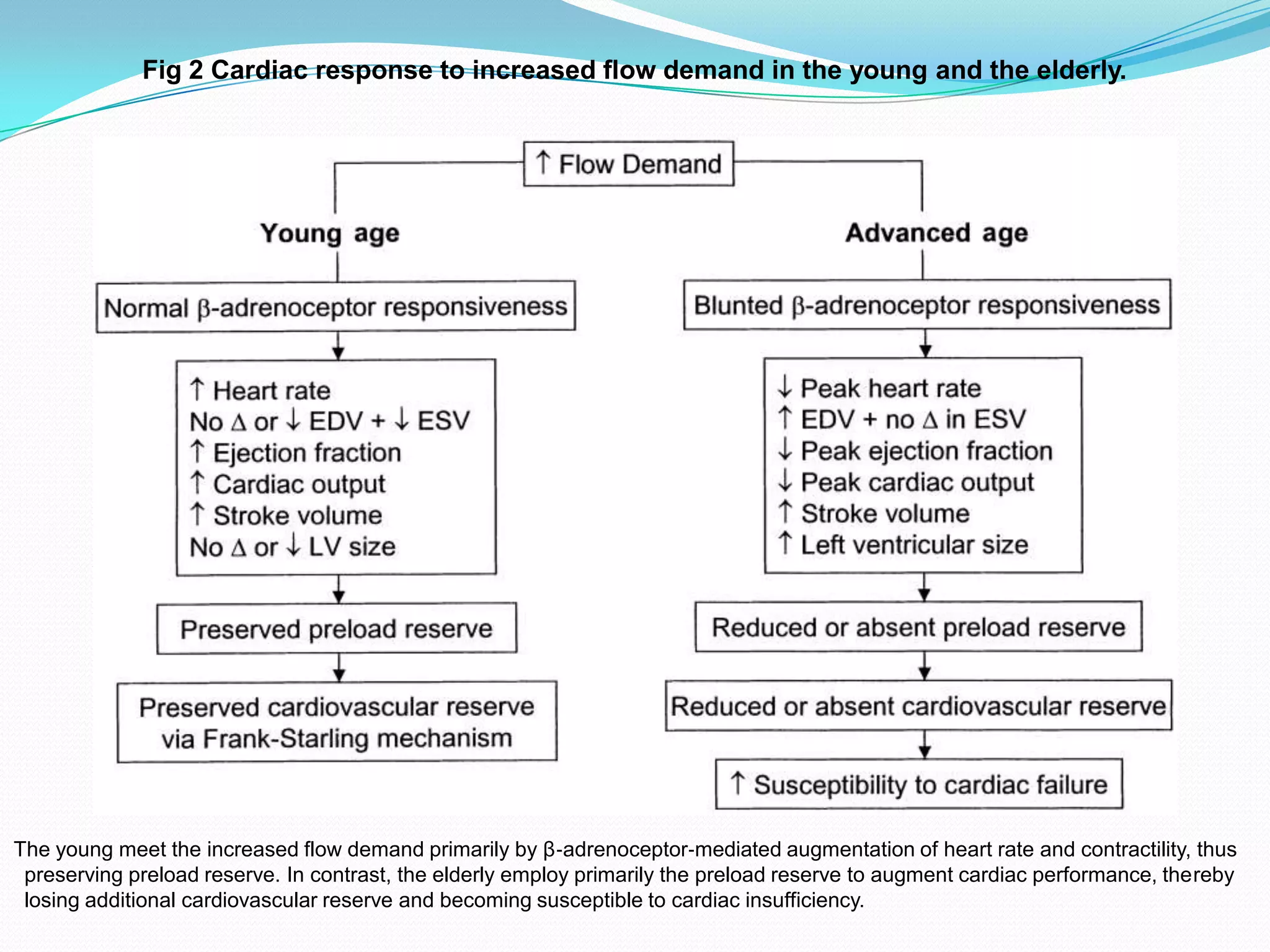
- The document discusses the physiological changes that occur with aging and their implications for anesthesia and surgery. Some key points:
1. Aging is associated with declines in organ function, functional capacity, and homeostatic mechanisms. Approximately 15-25% of surgical patients are aged 65 or older.
2. Common physiological changes with aging include declines in brain/nervous system function, cardiovascular function, respiratory function, renal/hepatic function, and altered pharmacokinetics.
3. These changes require special considerations for preoperative evaluation and perioperative management, including more judicious use of medications, fluid management, and temperature regulation. Regional anesthesia may provide some benefits over general anesthesia for elderly patients.