This document provides an overview of pathology related to the female genital tract, including the vulva, vagina, cervix, and endometrium. It discusses infections, pre-malignant and malignant neoplasms of these structures. Some key points include that HPV is associated with most cervical cancers, endometrial carcinoma is most common in post-menopausal women due to unopposed estrogen, and endometrial hyperplasia is a risk factor for the development of endometrial cancer if not treated.

























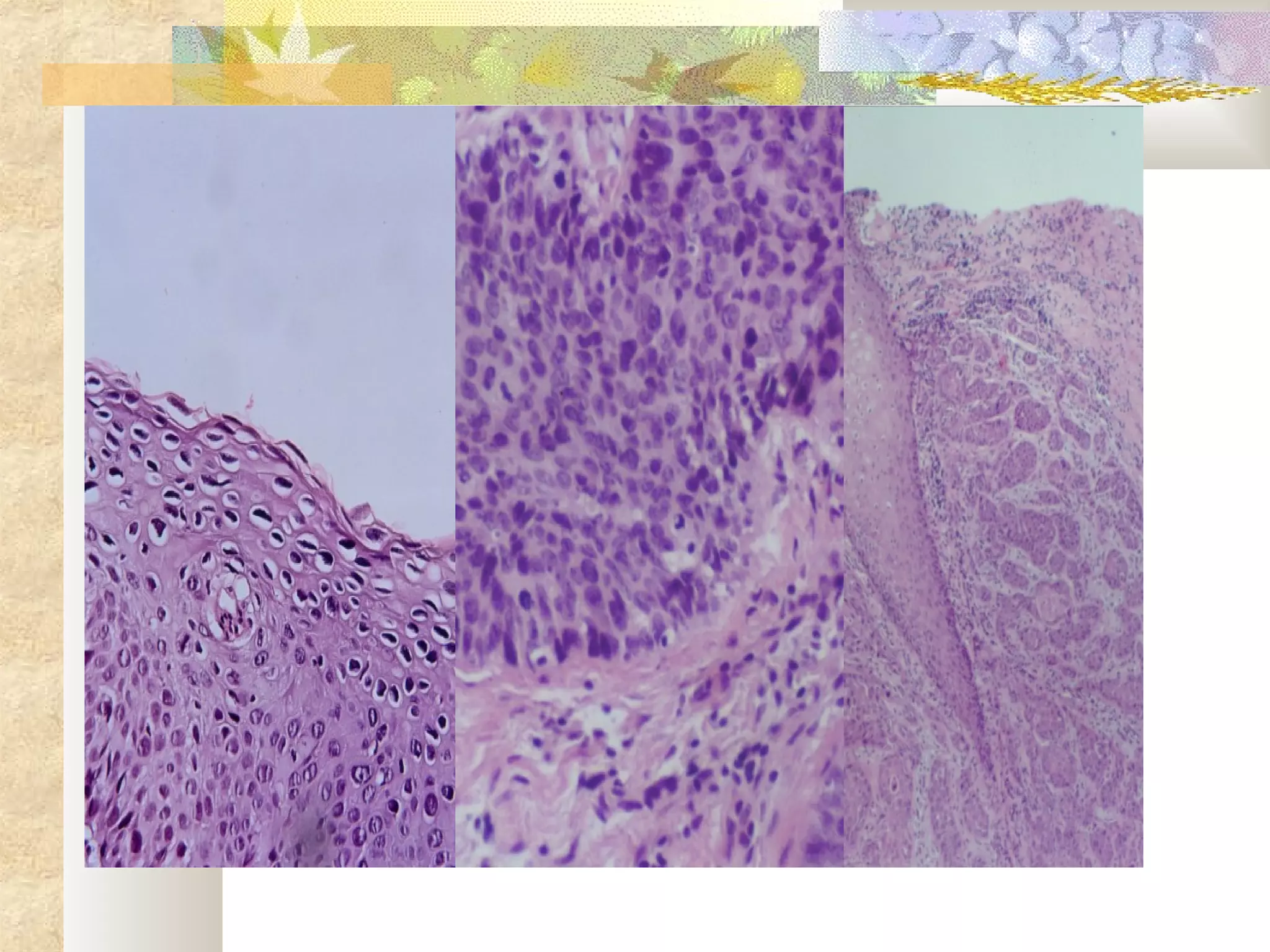
























![Cervical Intraepithelial Neoplasia (CIN)
and Carcinoma
Cytologic grading of precursor lesions
1) LOW GRADE SQUAMOUS
INTRAEPITHELIAL LESIONS
[CIN I and Condylomas (koilocytosis)]
2) HIGH GRADE SQUAMOUS
INTRAEPITHELIAL LESIONS
[CIN II, CIN III/CIS]](https://image.slidesharecdn.com/fgs-dr-150211020652-conversion-gate02/75/female-genital-system-52-2048.jpg)


























































































































































































