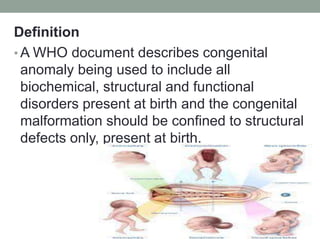
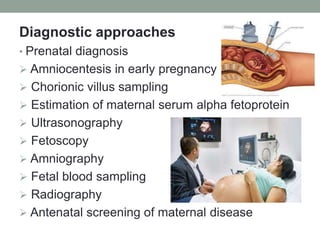
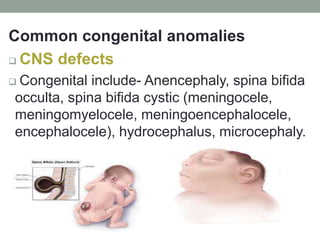
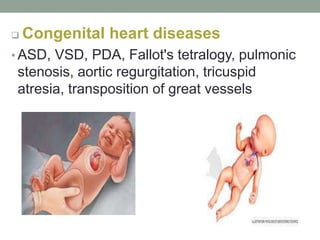
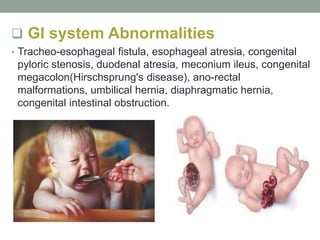
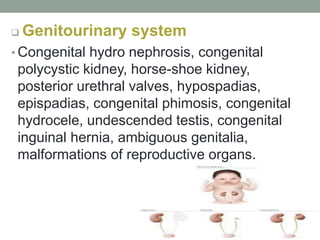
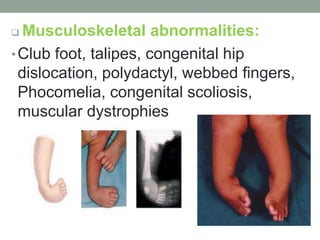
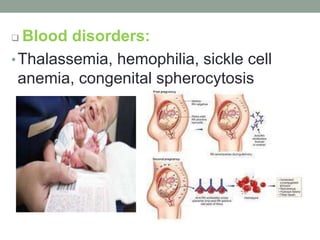
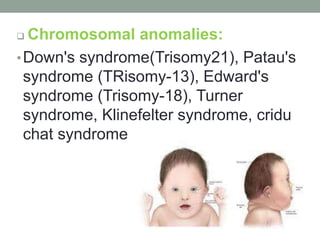
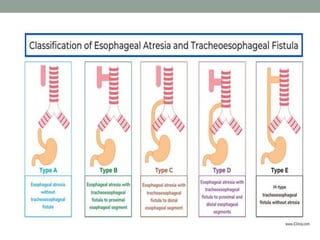
Congenital anomalies are defects present at birth that are caused by genetic and environmental factors. Some anomalies are obvious at birth like cleft lip, while others manifest later. Major anomalies require surgery, while minor ones have no functional implications. The most common anomalies in India are central nervous system and musculoskeletal abnormalities. Risk factors include advanced maternal age, consanguinity, and malnutrition. Nurses play an important role in educating families on prevention, screening, and caring for children with congenital anomalies.