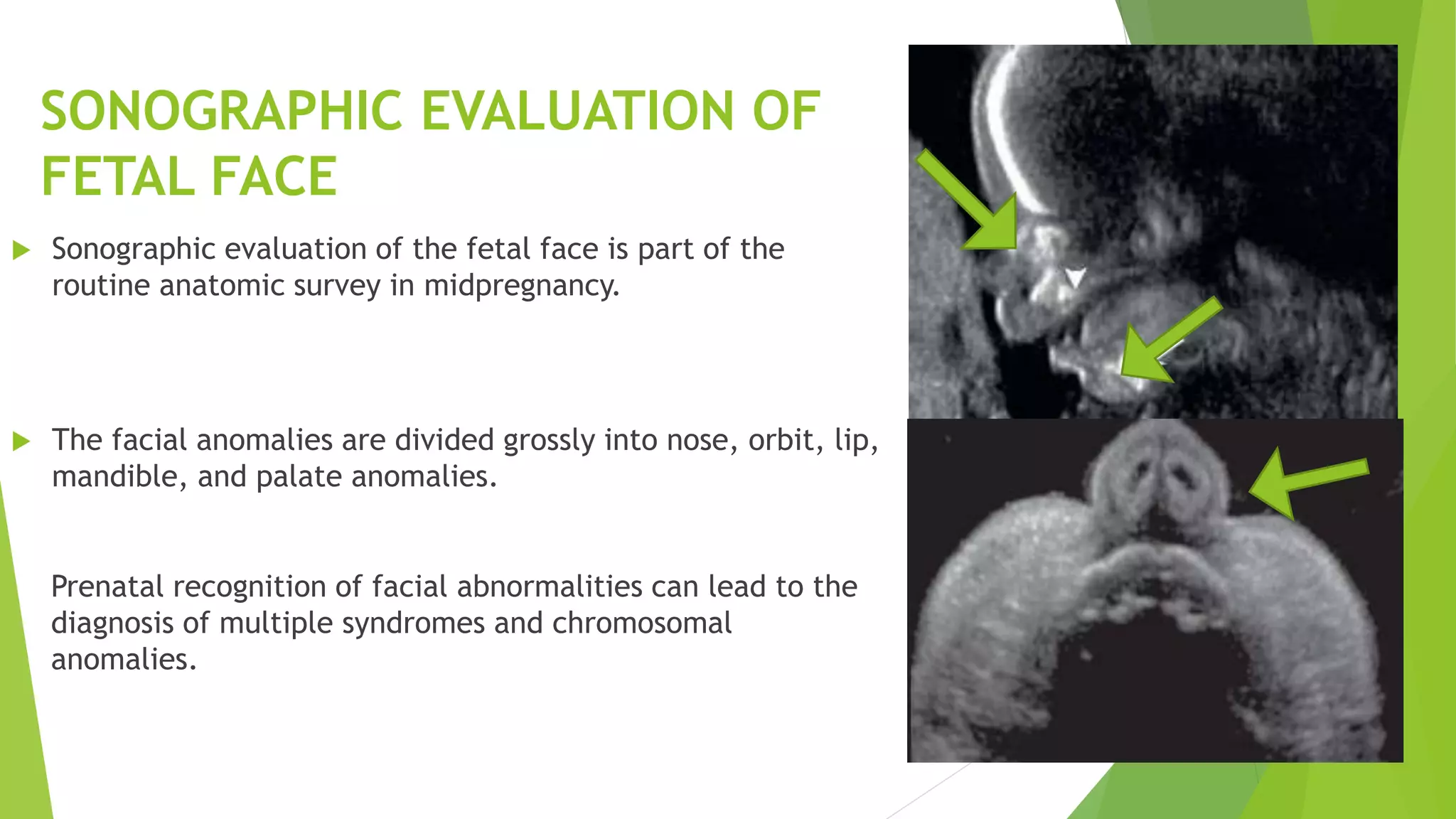
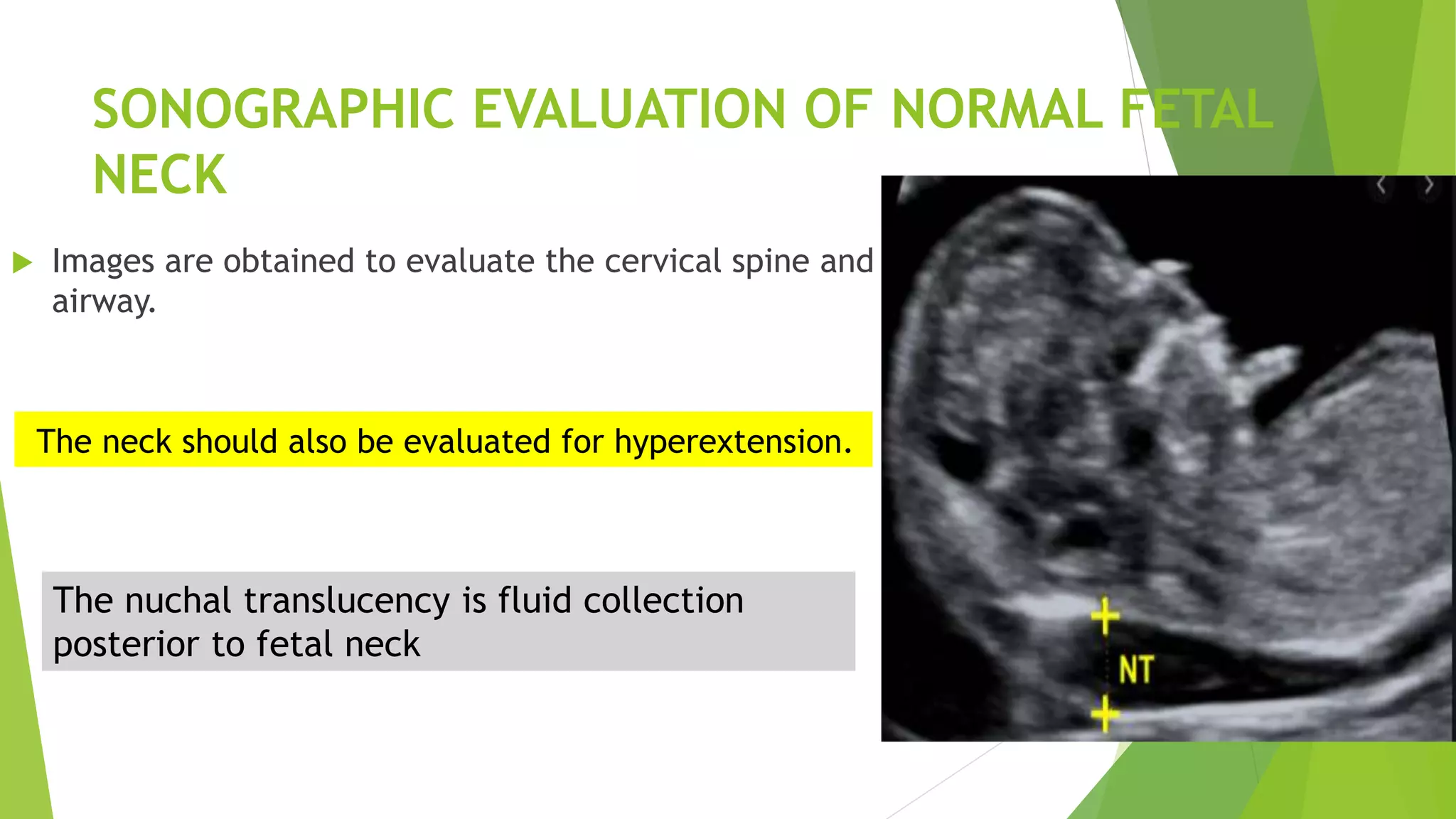
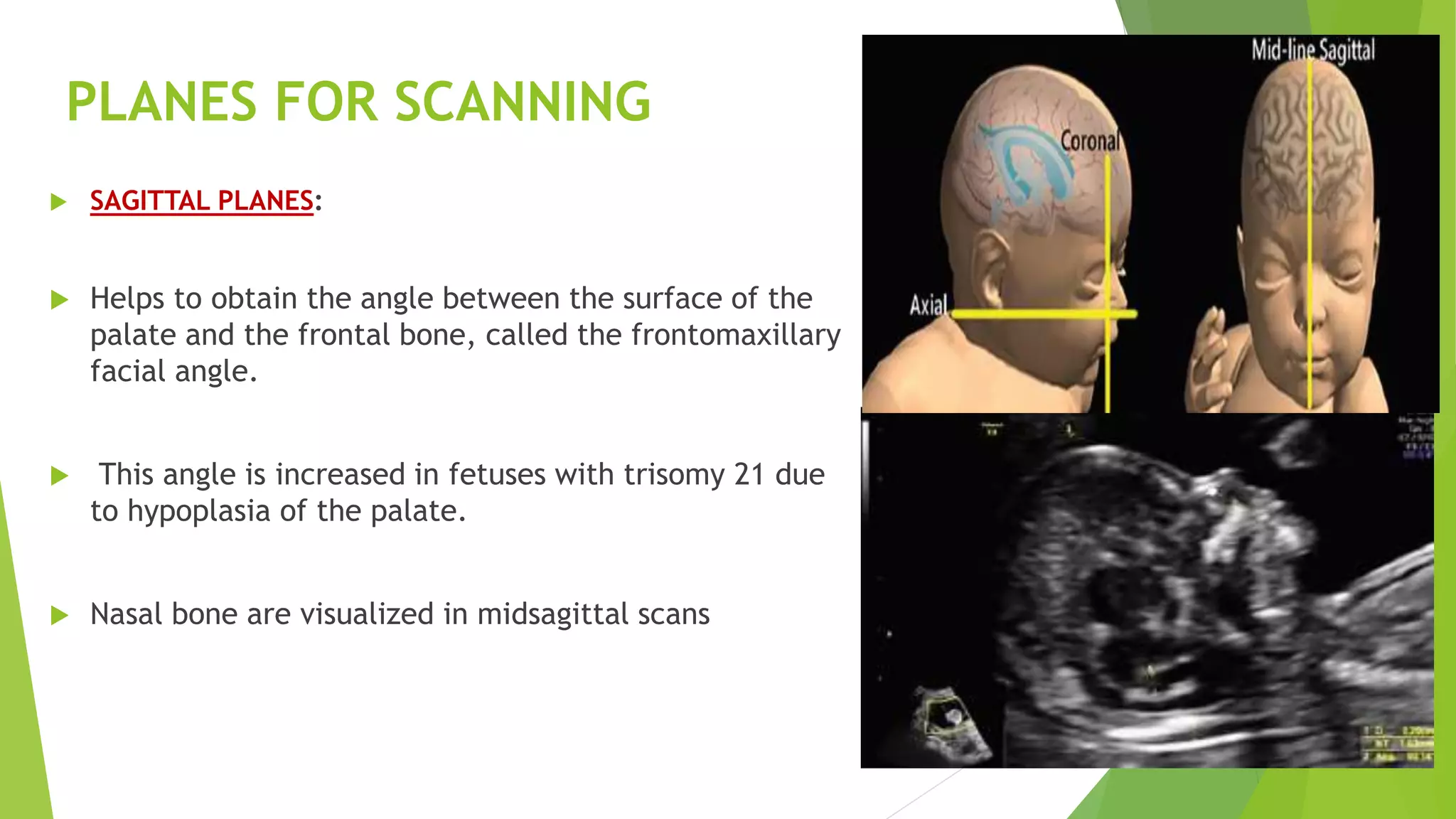
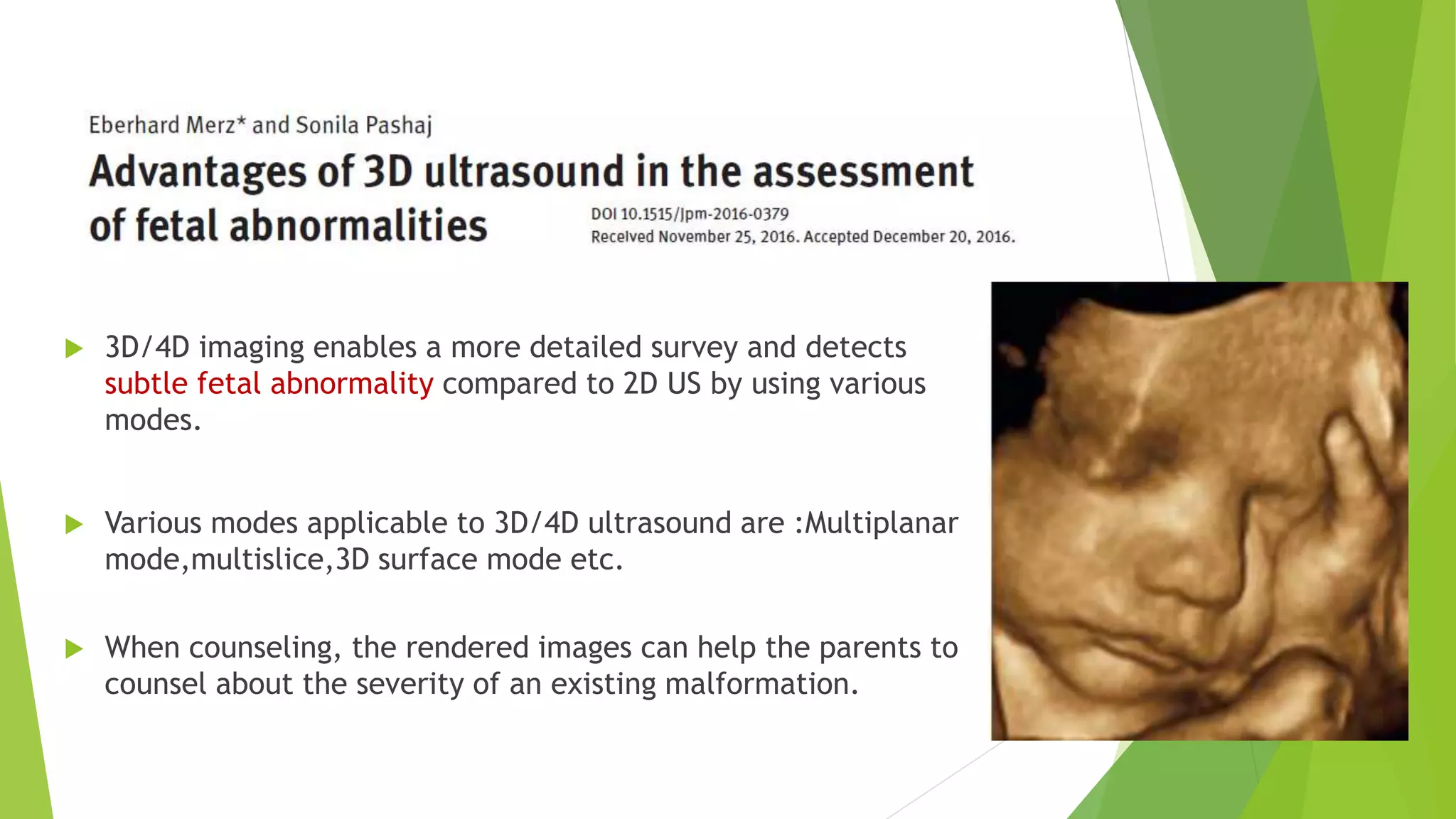
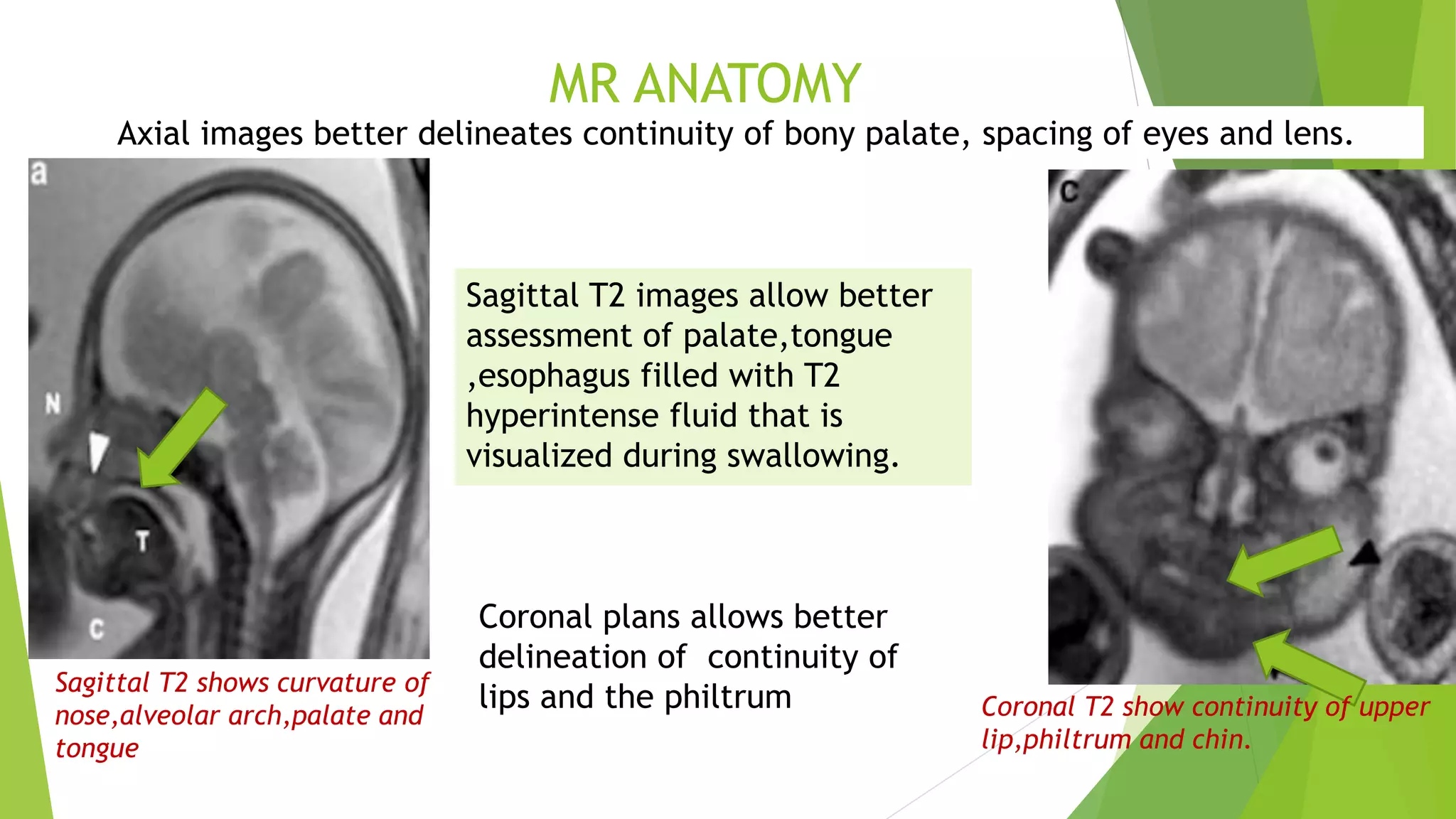
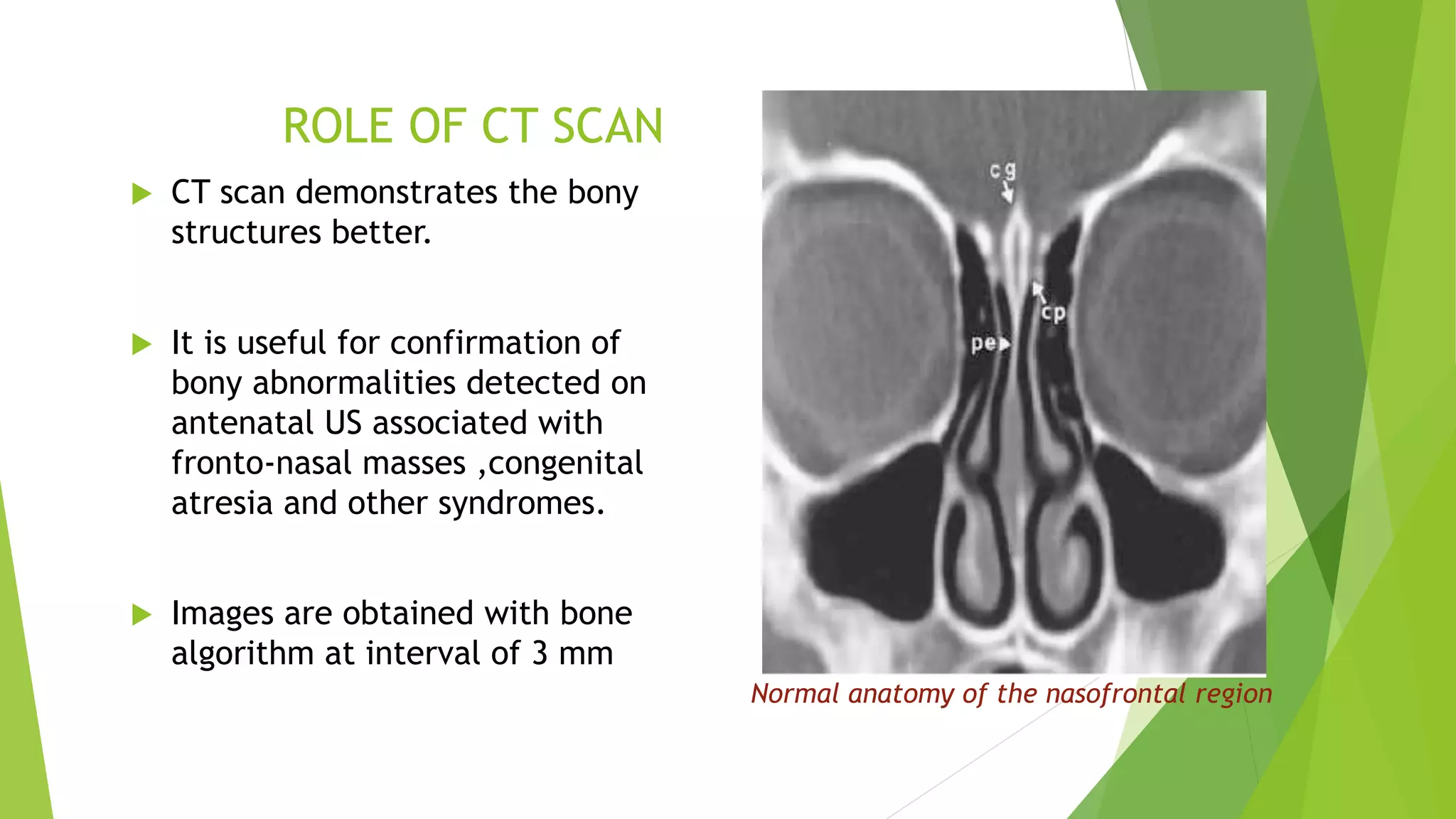
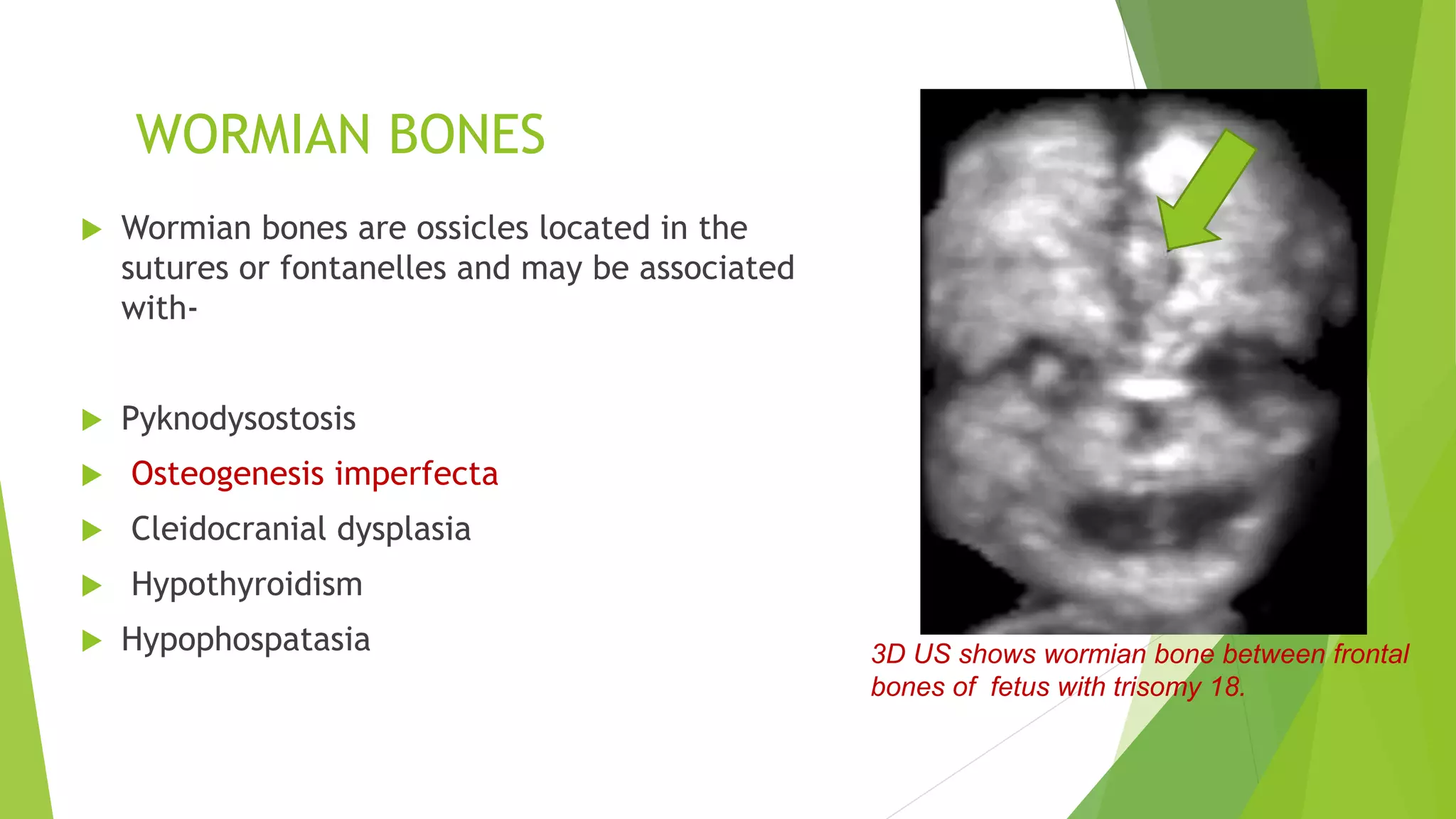
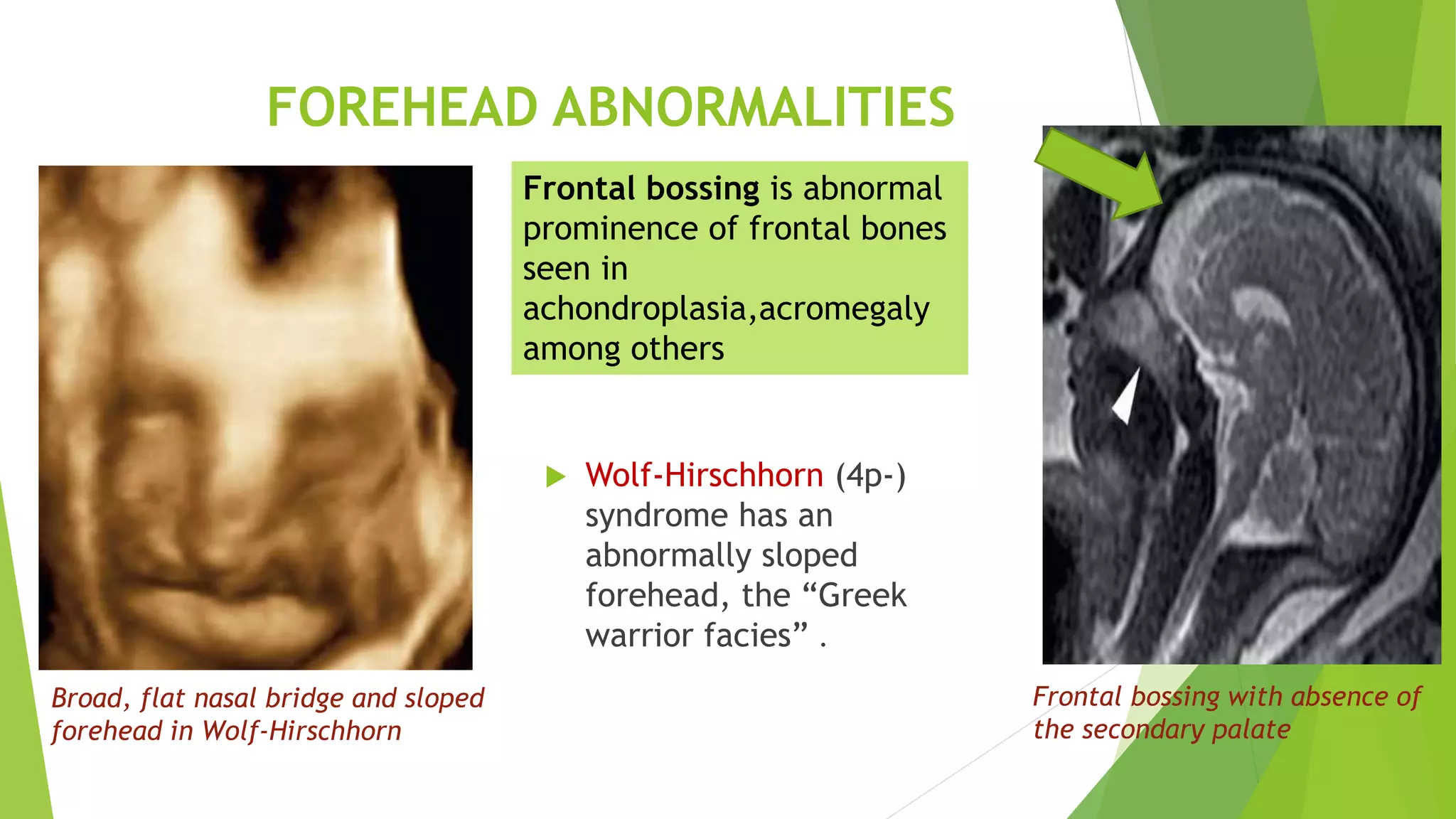
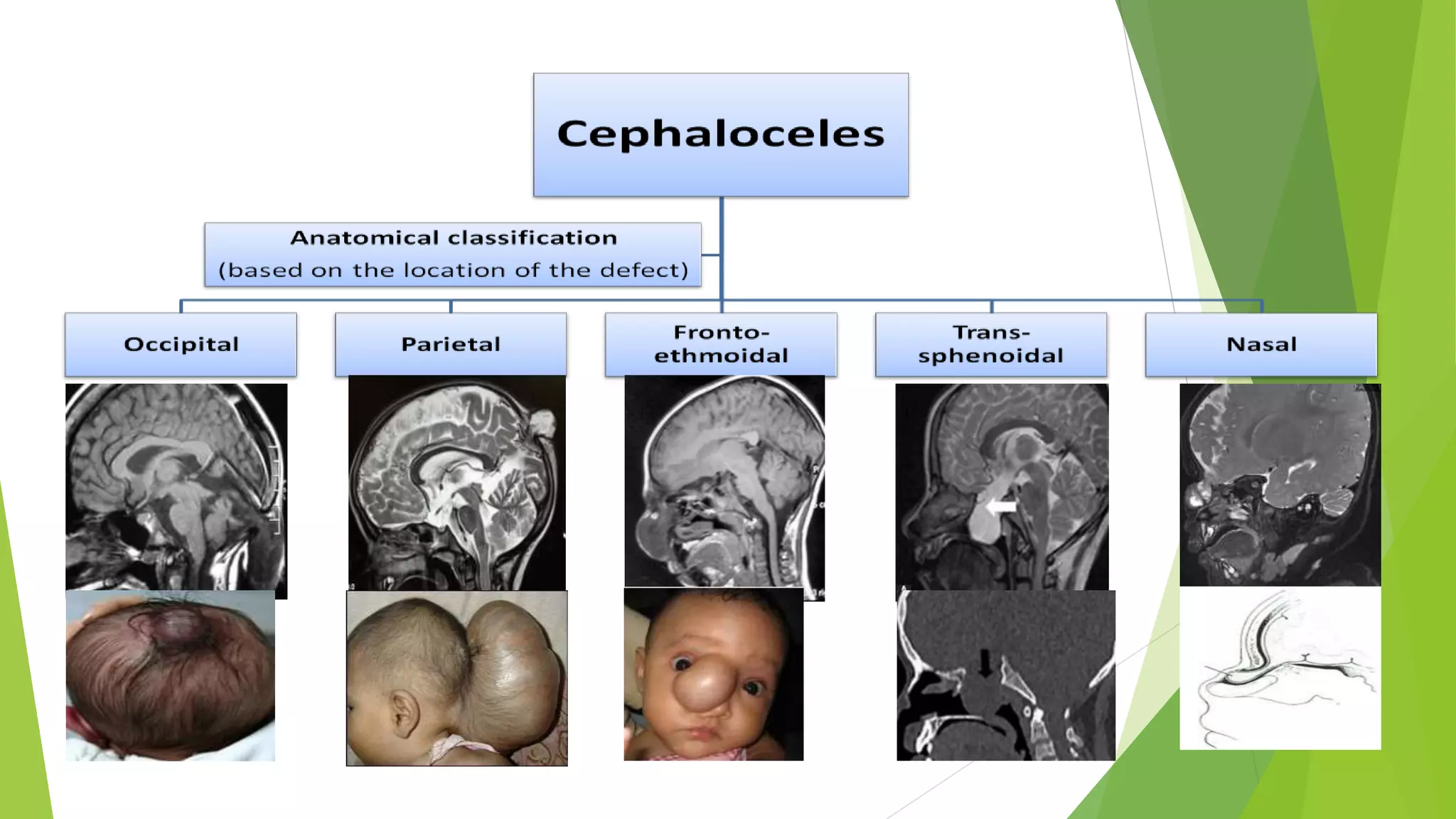
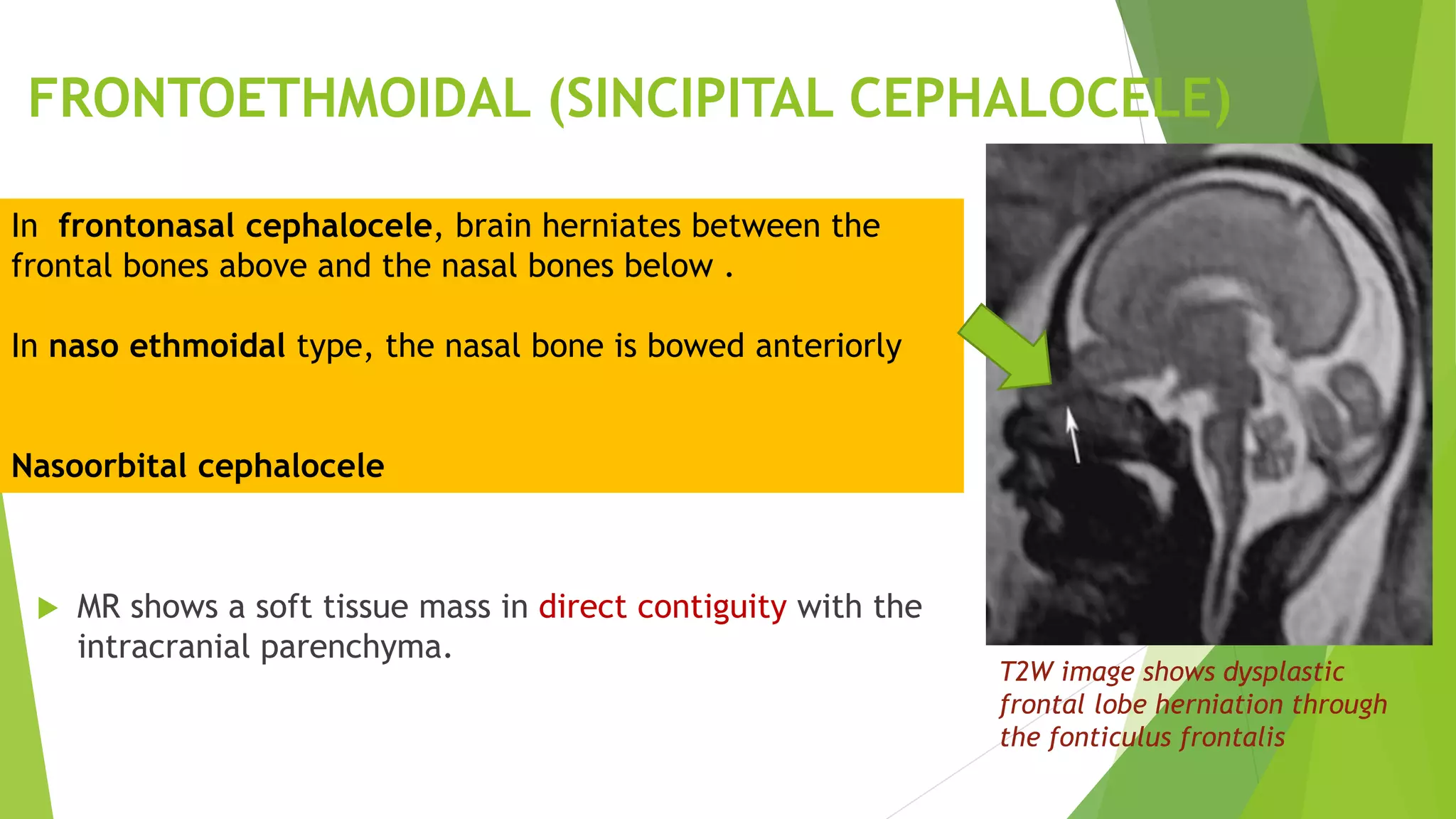
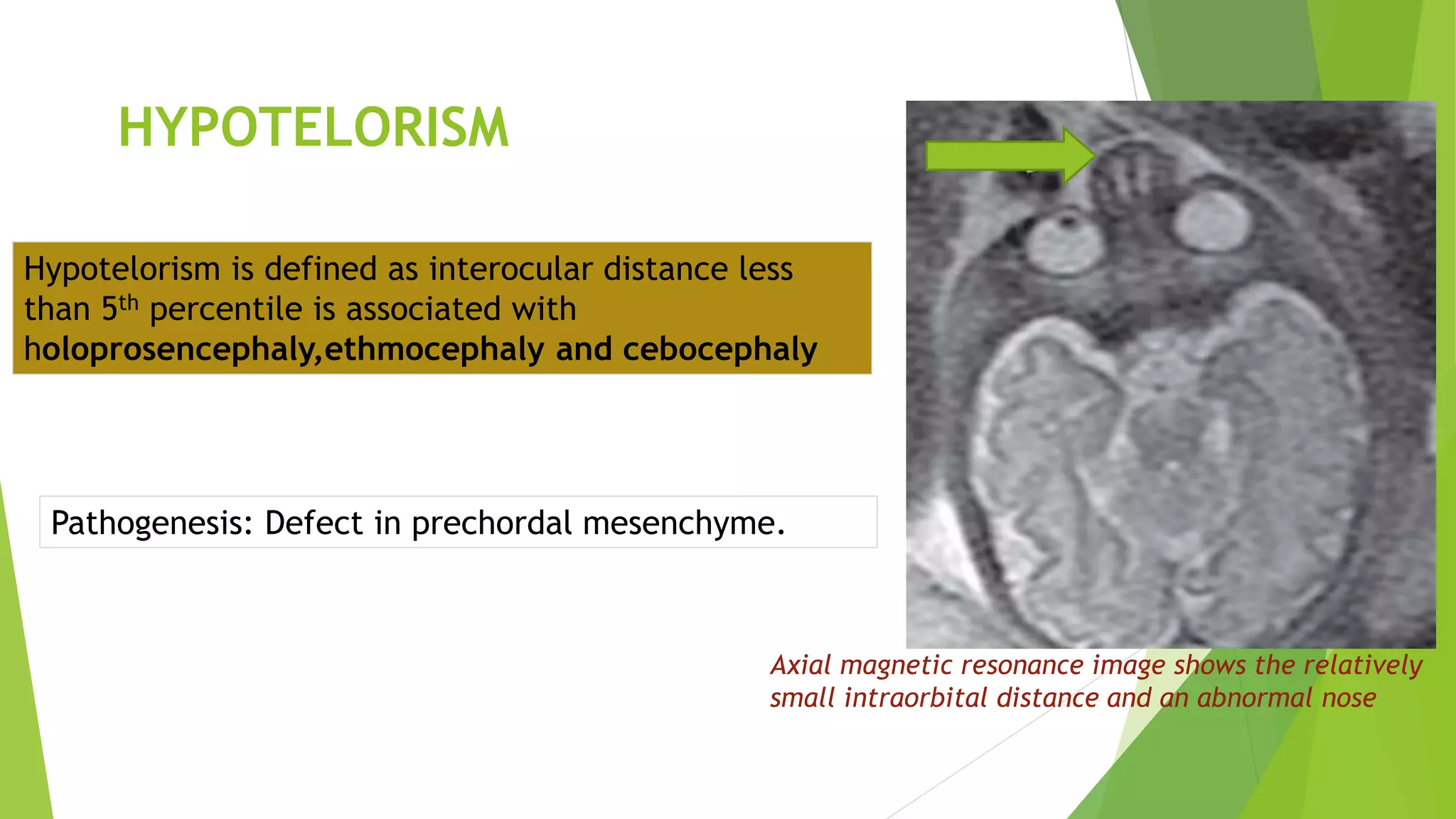
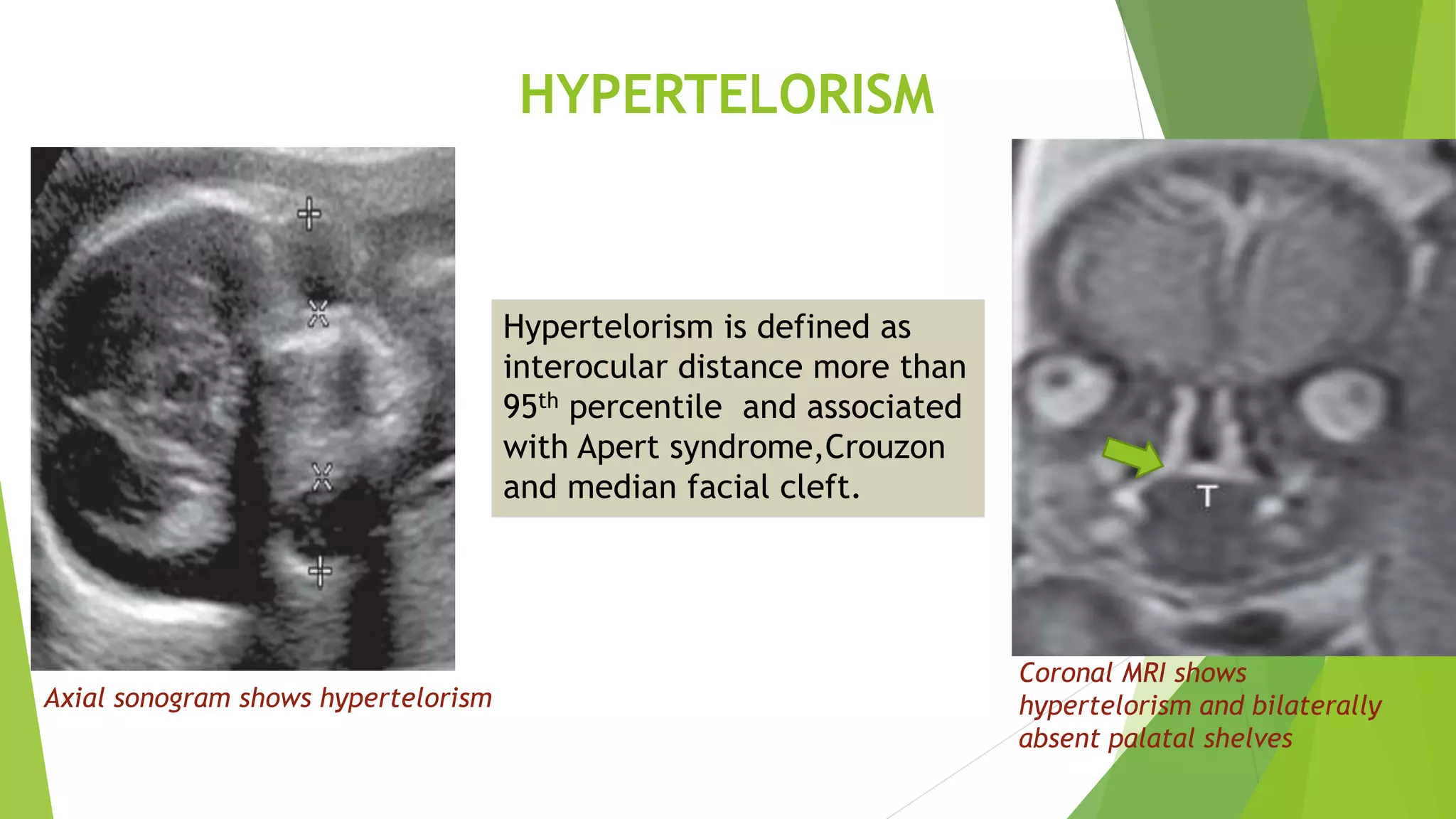
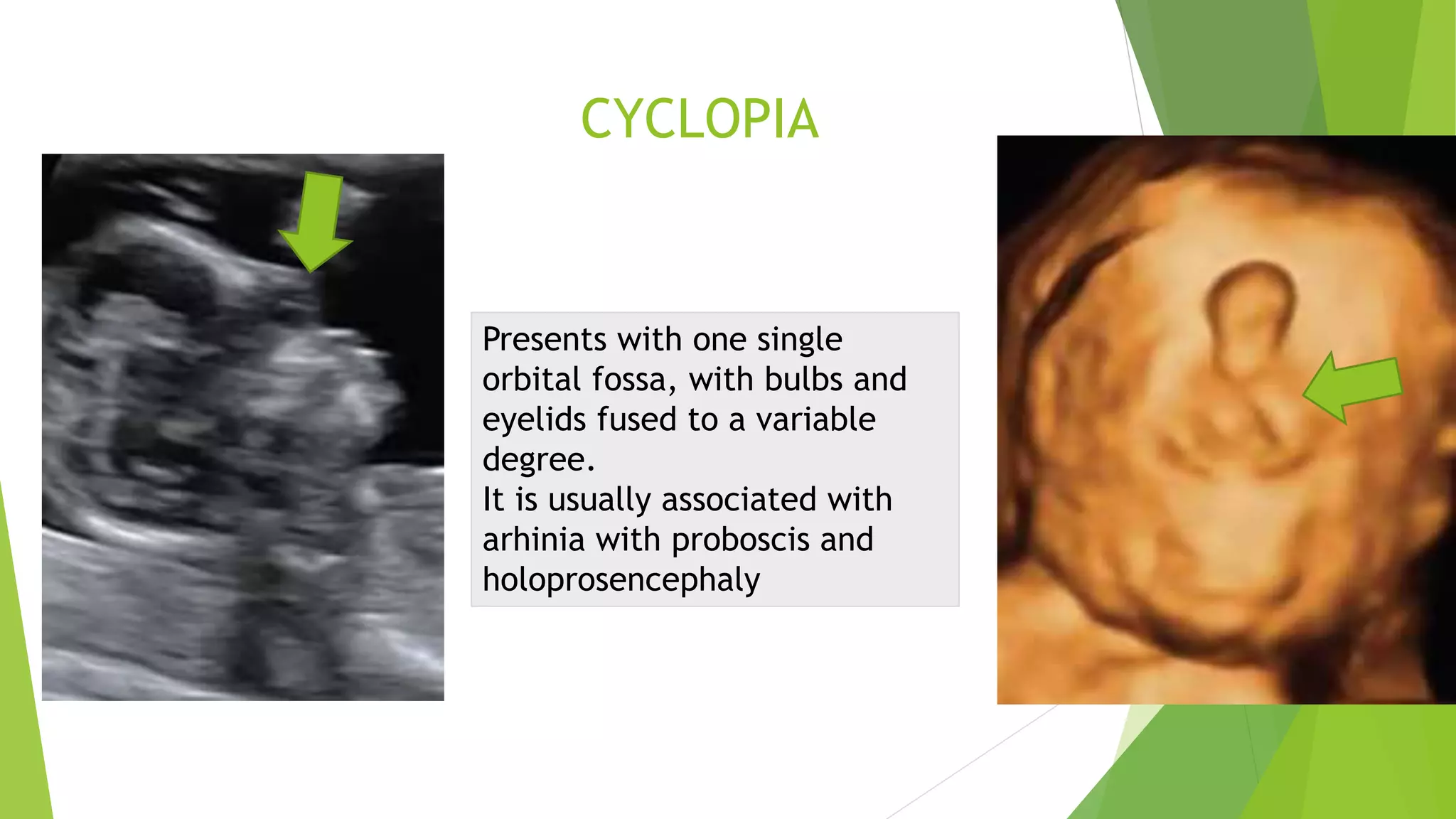
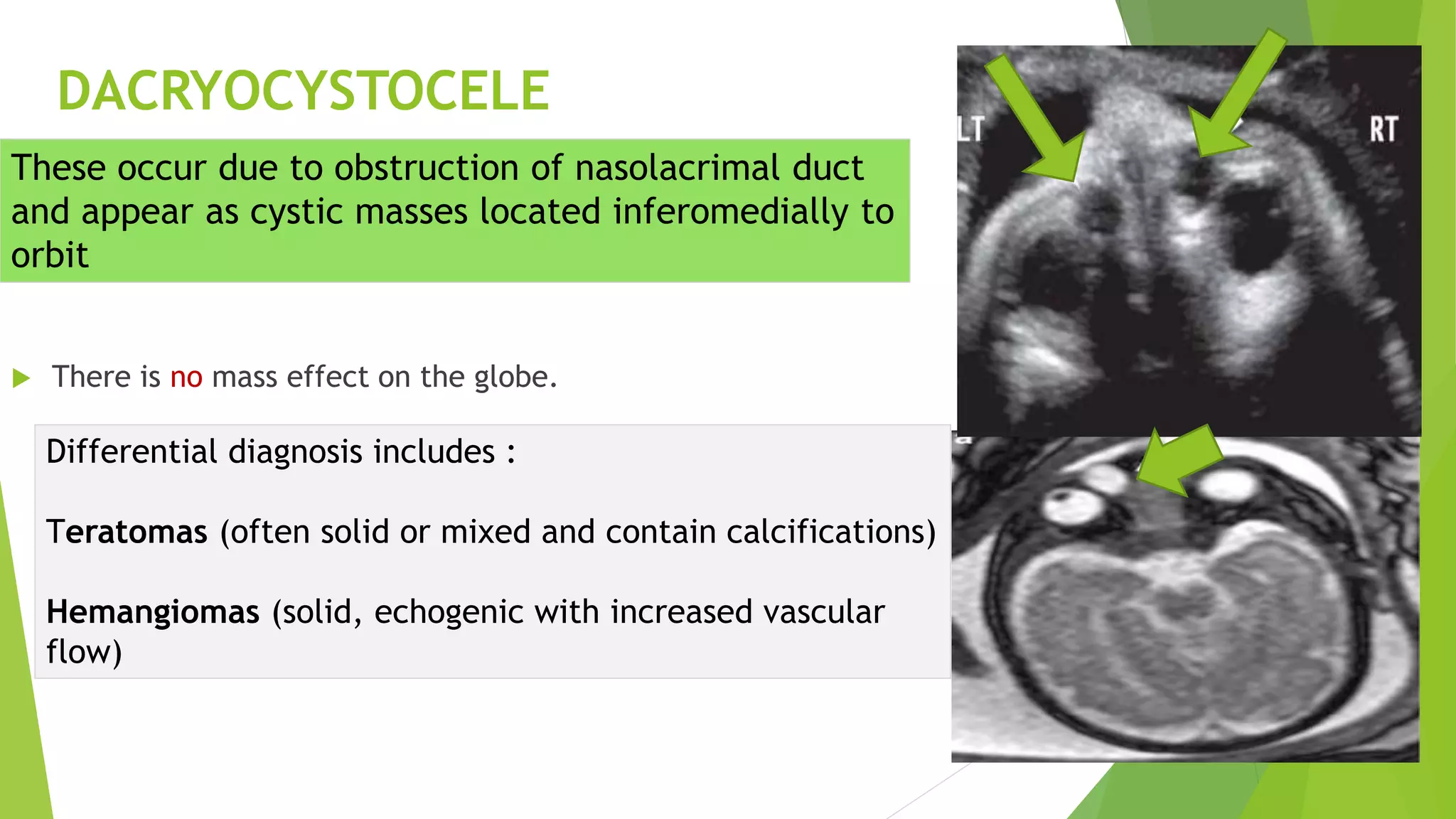
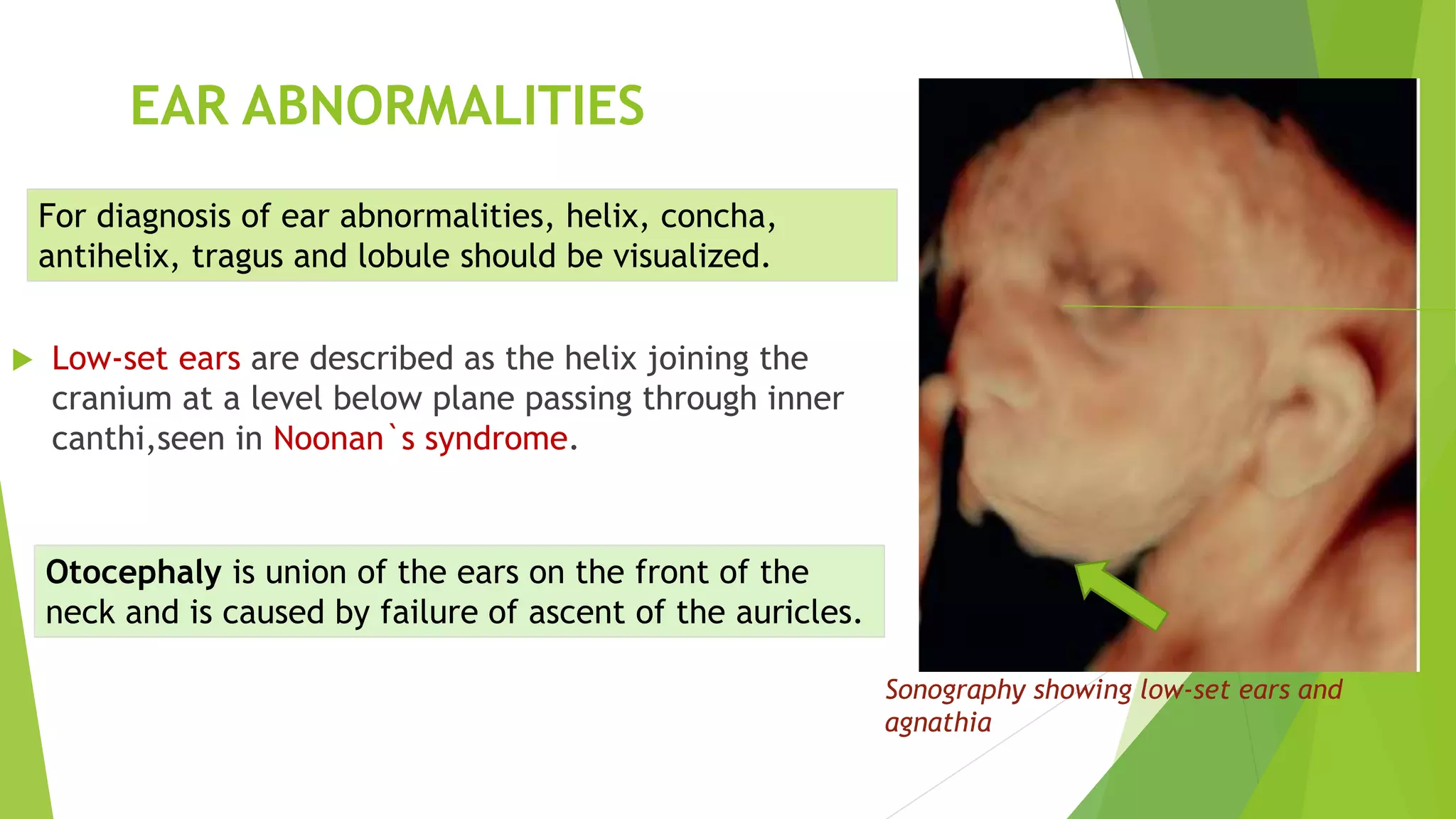
The document discusses congenital anomalies of the head, neck, and face, emphasizing the embryology and developmental processes involved in their formation. It provides insights into various scanning modalities, including ultrasound and MRI, for detecting these abnormalities, while detailing specific conditions like craniosynostosis and facial clefts. Additionally, the document covers diagnostic protocols and imaging techniques useful in evaluating fetal anatomy and identifying potential syndromes associated with these anomalies.