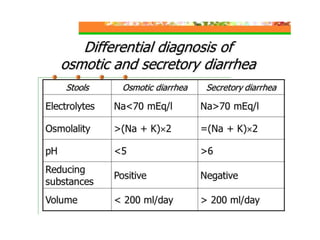
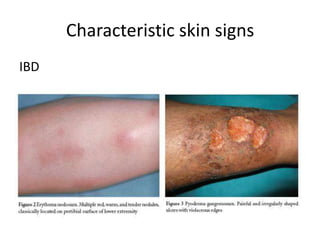
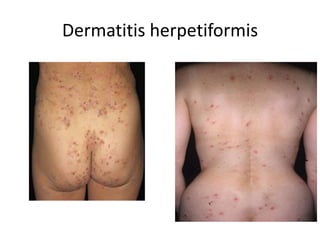
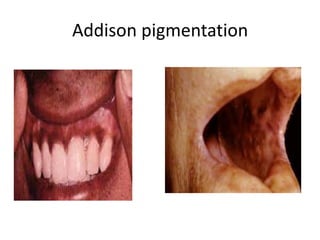
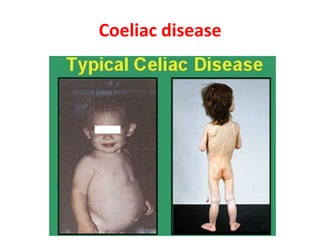
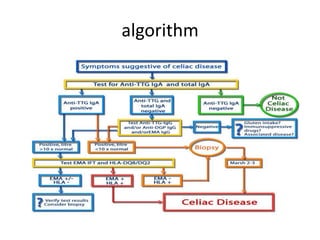
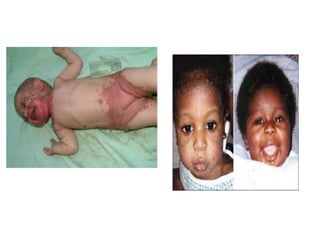
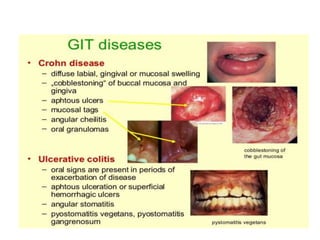
This document discusses chronic diarrhea in children, including definitions, causes, diagnosis, and treatment. It defines chronic diarrhea as diarrhea lasting 2-3 weeks or more. Common causes in infants include post-infectious lactase deficiency, celiac disease, cow's milk allergy, toddler's diarrhea, and infections like giardiasis. Diagnosis involves taking a thorough history and physical exam, with investigations tailored to the child's age and suspected causes, such as stool exams and tests for carbohydrate malabsorption.