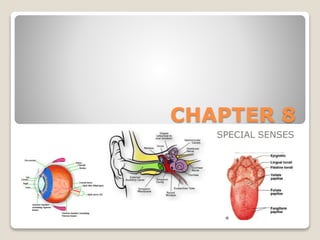
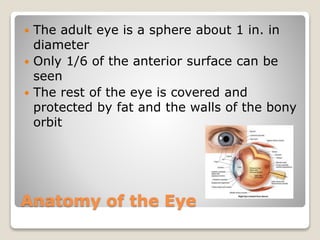
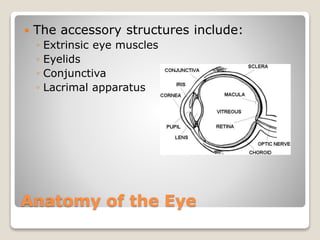
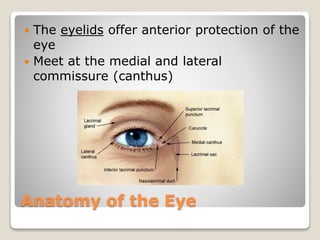
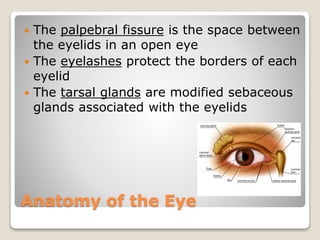
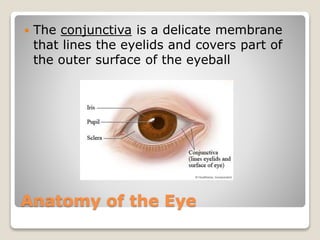
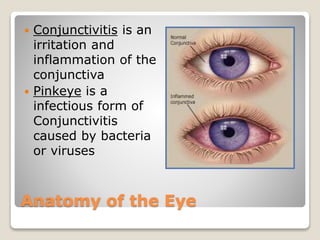
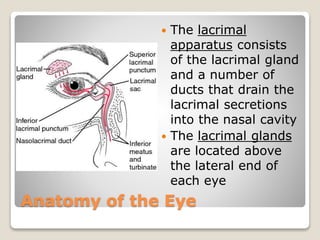
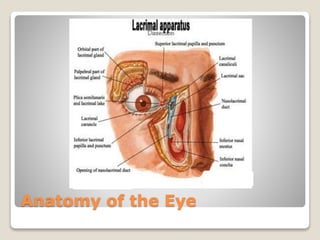
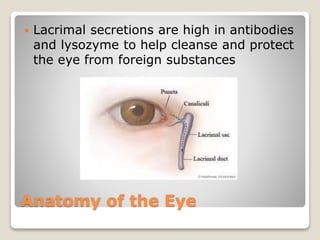
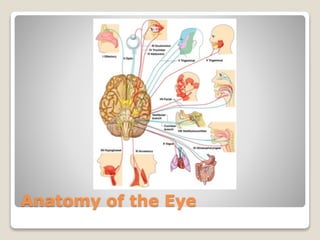
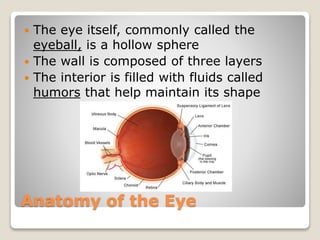
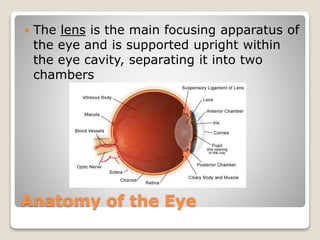
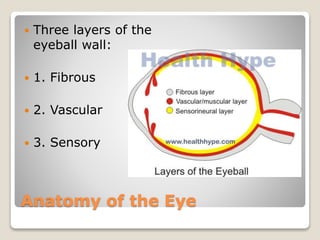
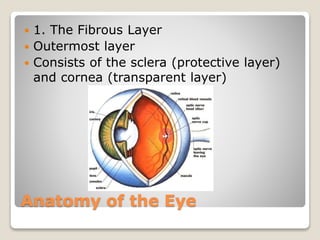
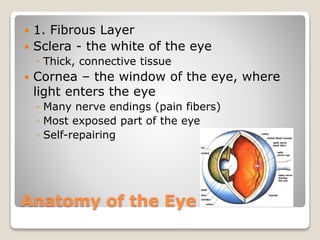
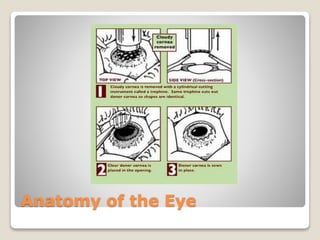
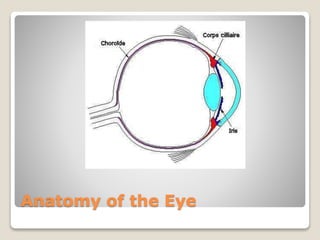
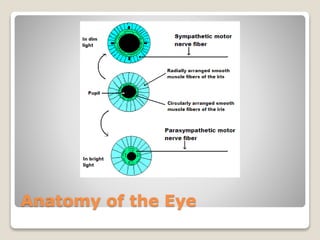
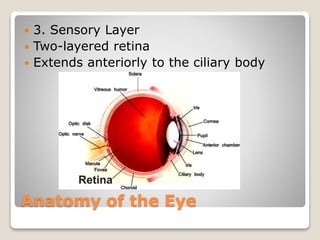
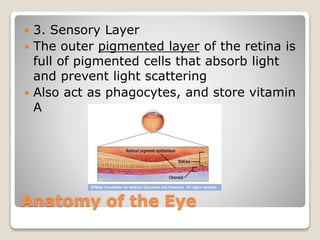
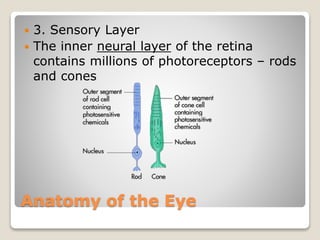
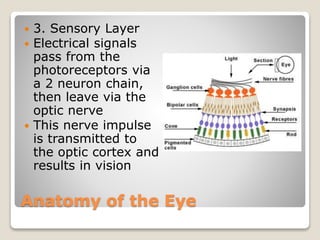
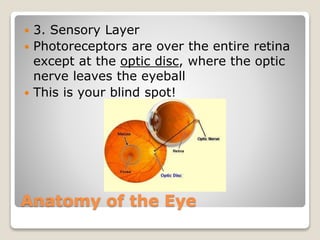
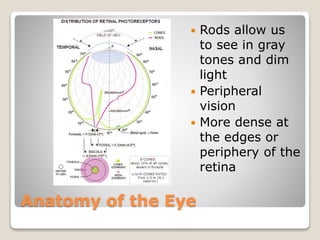
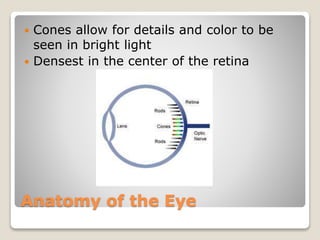
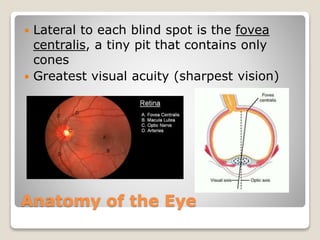
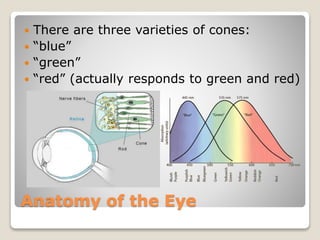
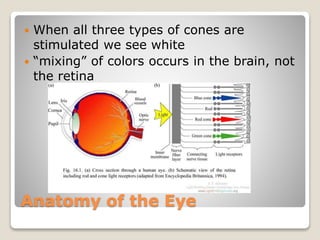
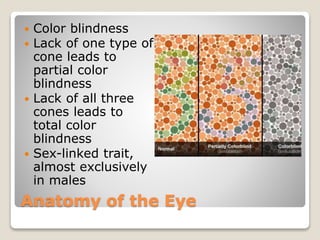
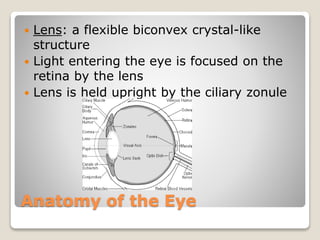
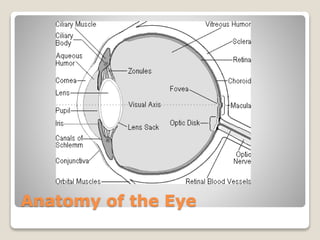
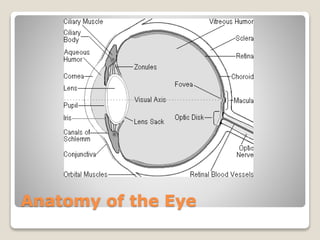
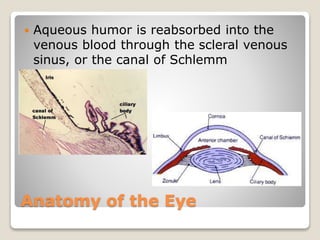
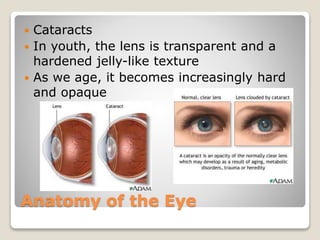
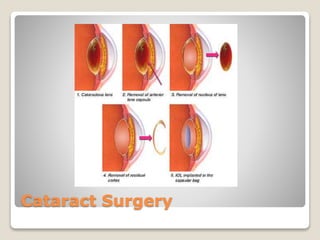
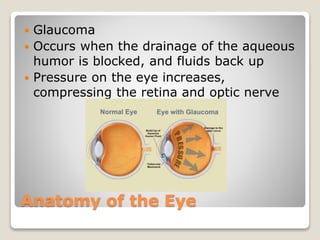
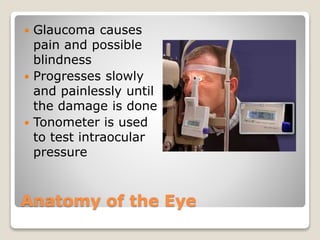
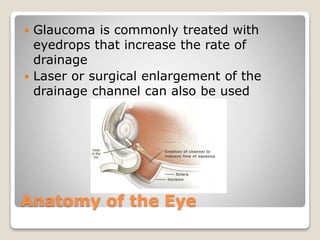
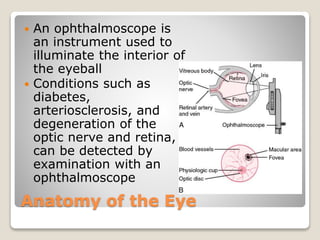
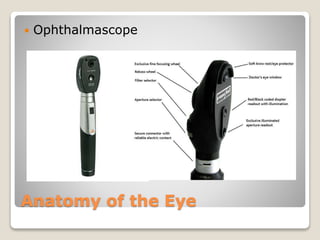
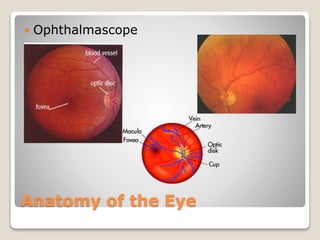
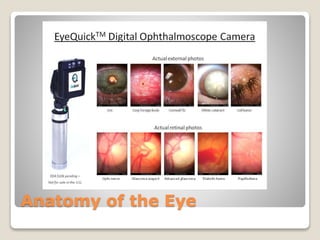
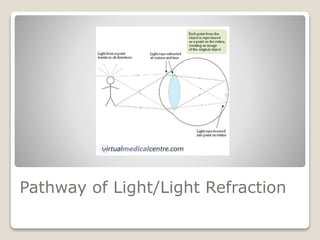
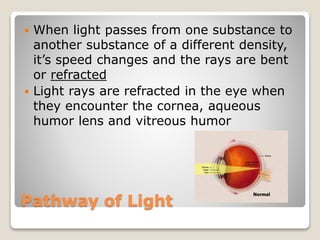
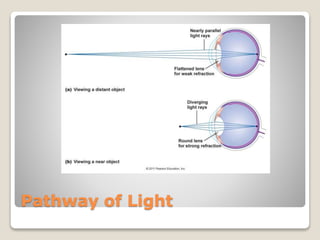
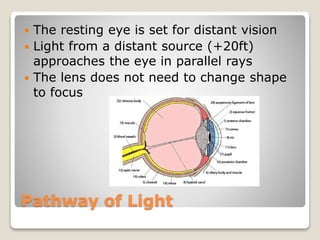
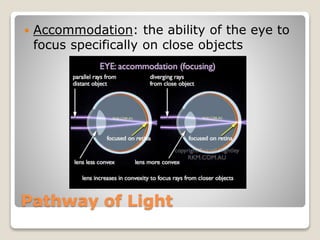
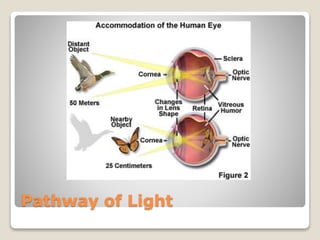
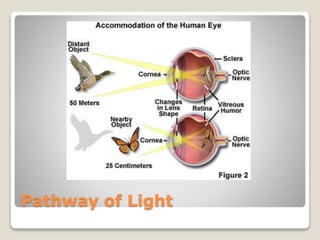
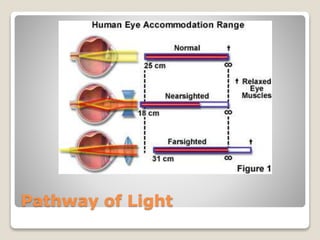
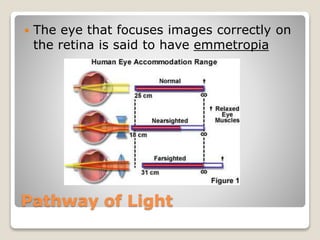
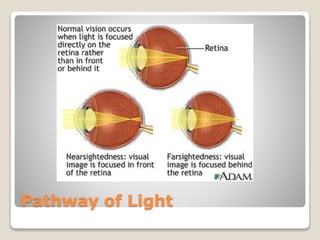
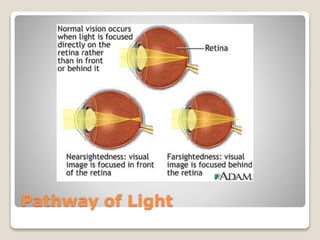
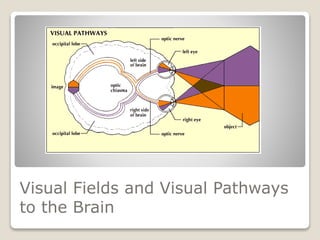
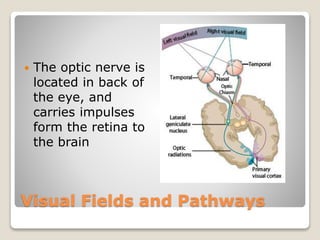
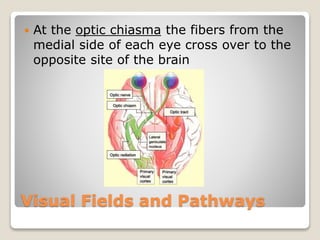
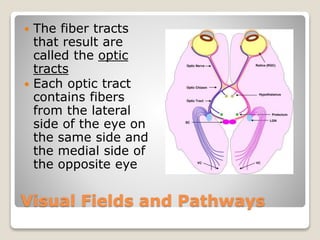
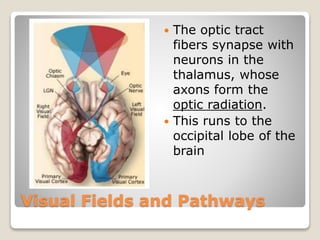
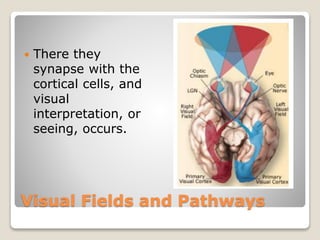
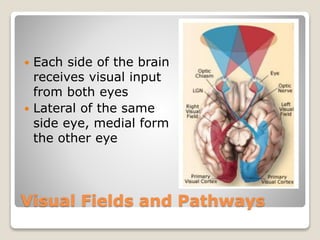
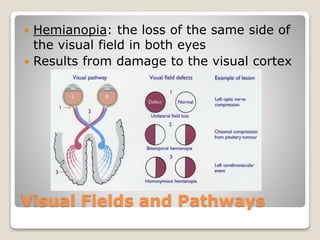
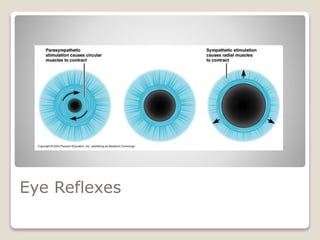
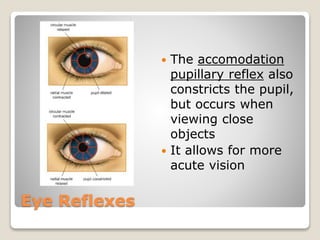
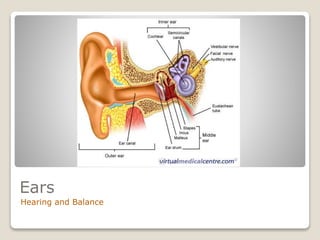
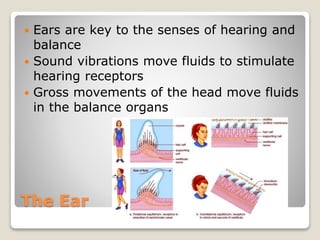
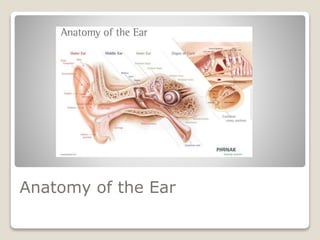
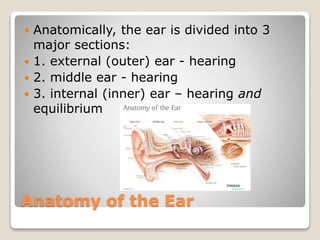
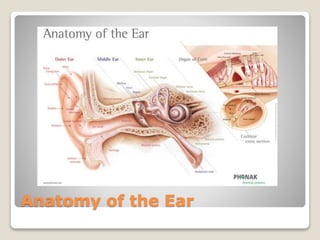
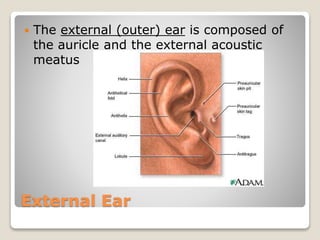
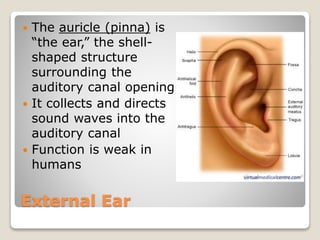
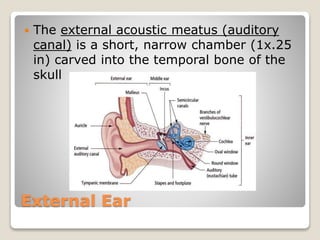
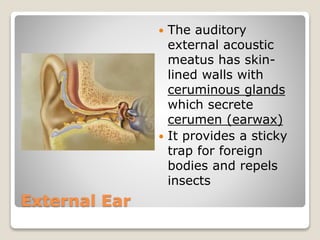
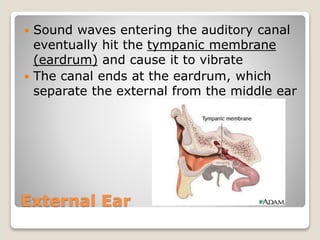
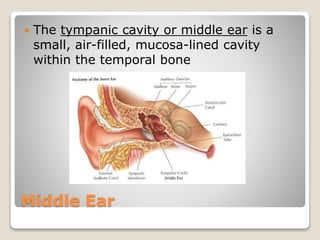
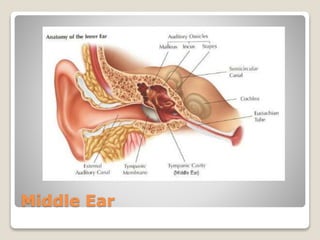
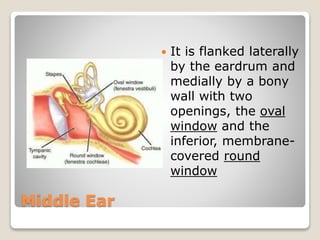
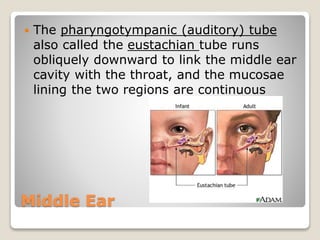
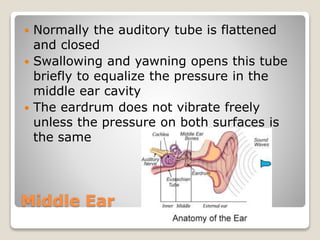
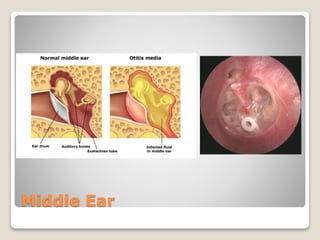
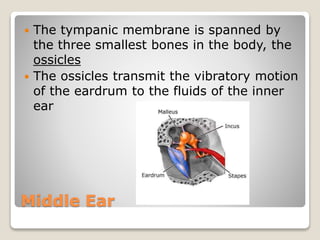
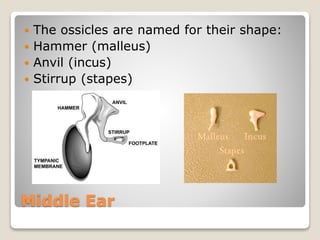
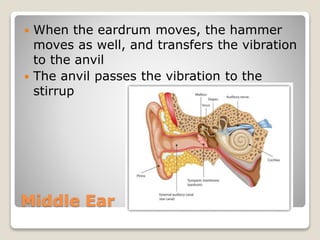
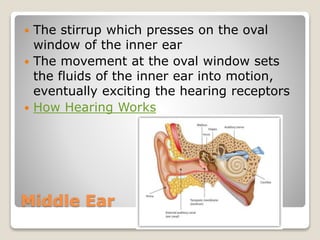
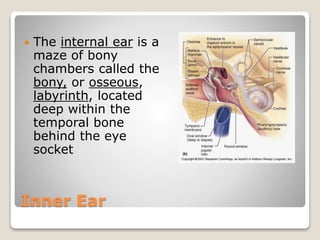
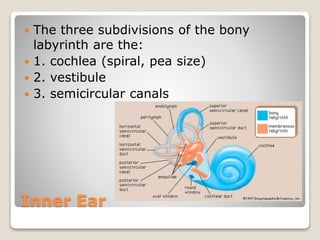
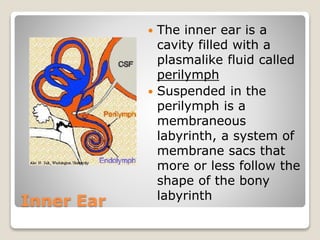
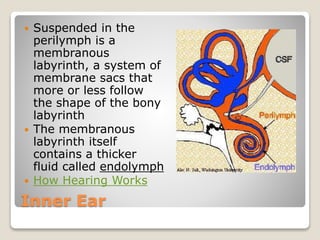
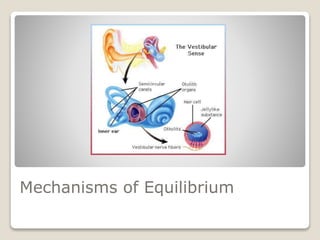
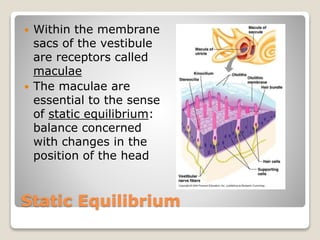
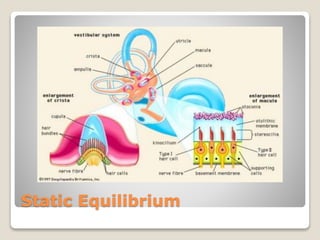
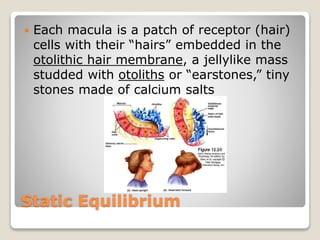
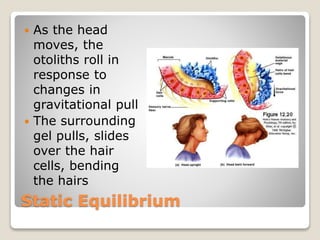
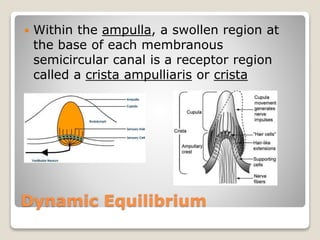
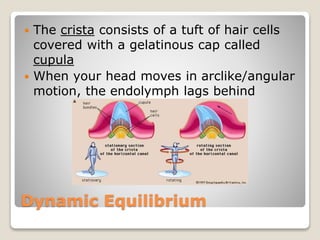
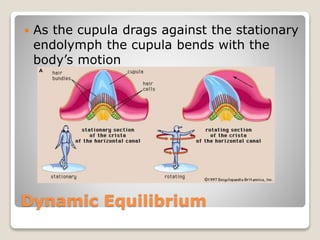
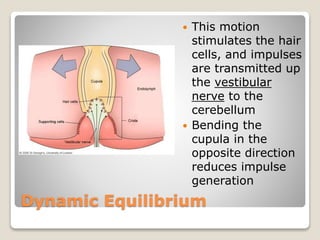
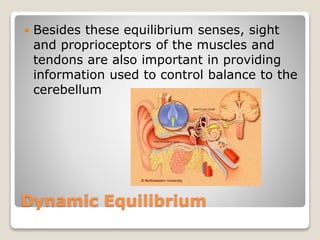
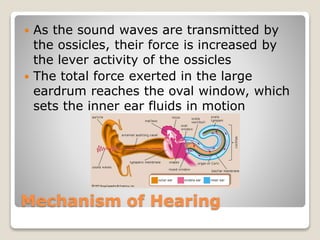
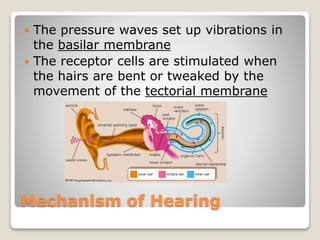
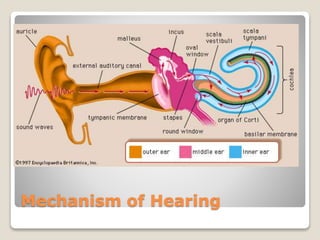
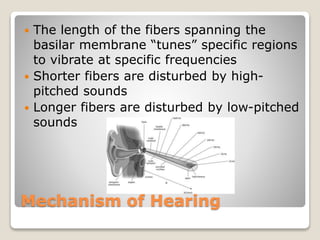
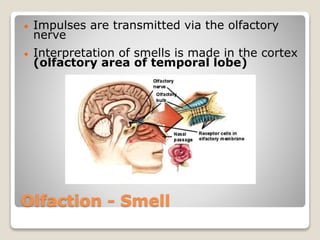
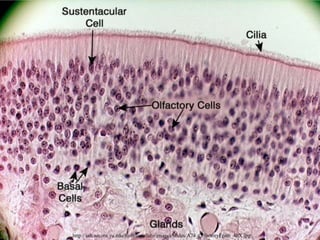
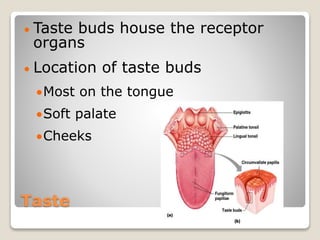
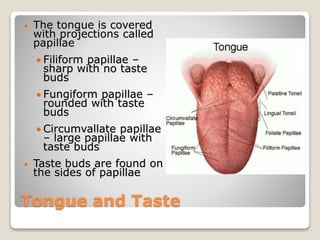
The document describes the anatomy and physiology of the human eye. It details the structures of the eye including the fibrous layer with the sclera and cornea, the vascular layer with the choroid, ciliary body and iris, and the sensory layer with rods and cones in the retina. It explains how light enters the eye and is refracted by the cornea, aqueous humor, lens, and vitreous humor, forming an inverted image on the retina. The document also discusses common vision conditions like cataracts, glaucoma, color blindness, accommodation, and myopia.