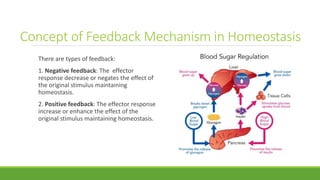
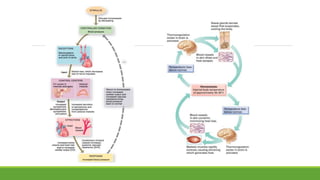
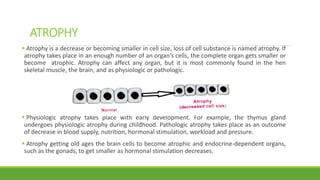
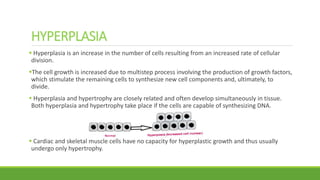
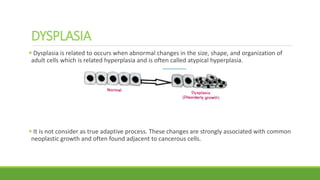
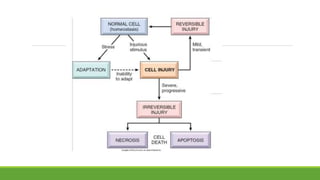
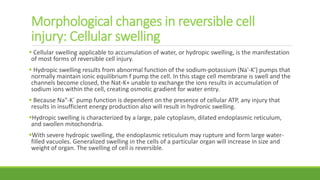
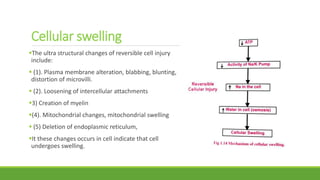
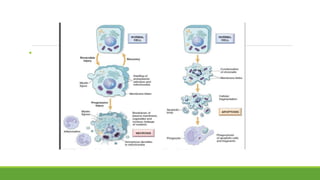
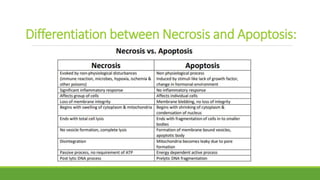
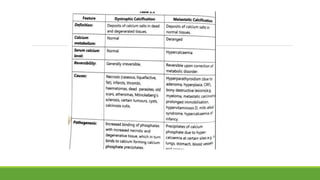
The document discusses cell injury and inflammation, focusing on the principles of pathophysiology, the mechanisms of cell injury, and adaptive cellular responses. It details various causes of cell injury, including hypoxia, physical stress, drugs, and microbial agents, as well as the processes of cellular adaptation such as atrophy, hypertrophy, hyperplasia, metaplasia, and dysplasia. Additionally, it explores the pathways of cell damage and recovery, emphasizing the importance of homeostasis and feedback mechanisms in maintaining cellular function.