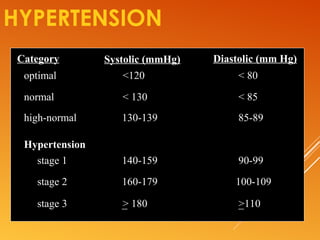
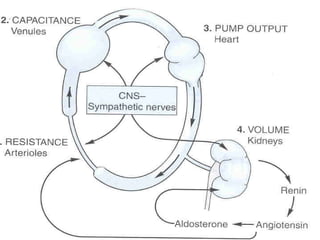
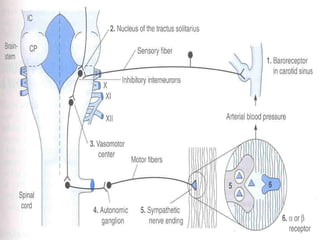
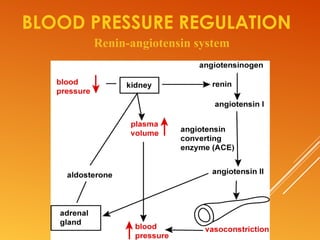
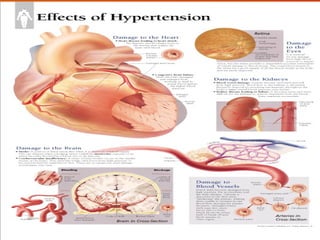
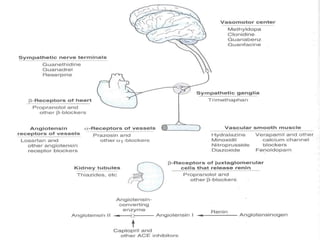
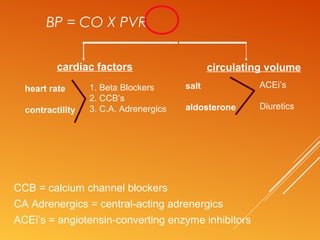
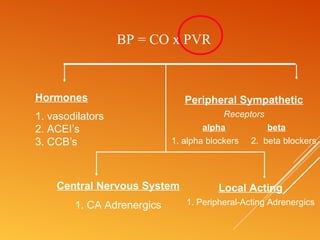
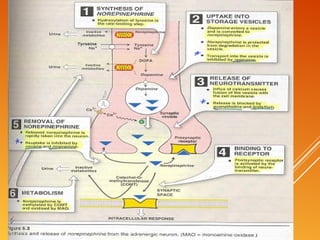
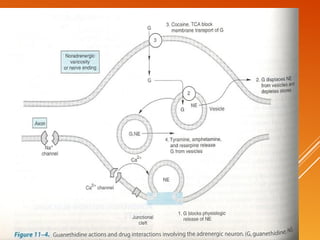
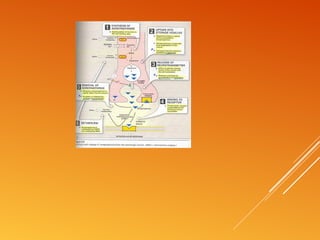
This document discusses drug treatment for hypertension. It begins by defining hypertension and classifying it by severity based on systolic and diastolic blood pressure readings. The causes of primary and secondary hypertension are explained. Blood pressure regulation involves the renin-angiotensin system and is controlled by both short-term mechanisms like the autonomic nervous system and long-term mechanisms like fluid volume regulation. The major classes of antihypertensive drugs are described including diuretics, beta-blockers, ACE inhibitors, calcium channel blockers, and others. Lowering blood pressure reduces risks of heart disease, stroke, kidney failure and other complications. Treatment involves lifestyle modifications and drug therapy tailored to a patient's risk level.