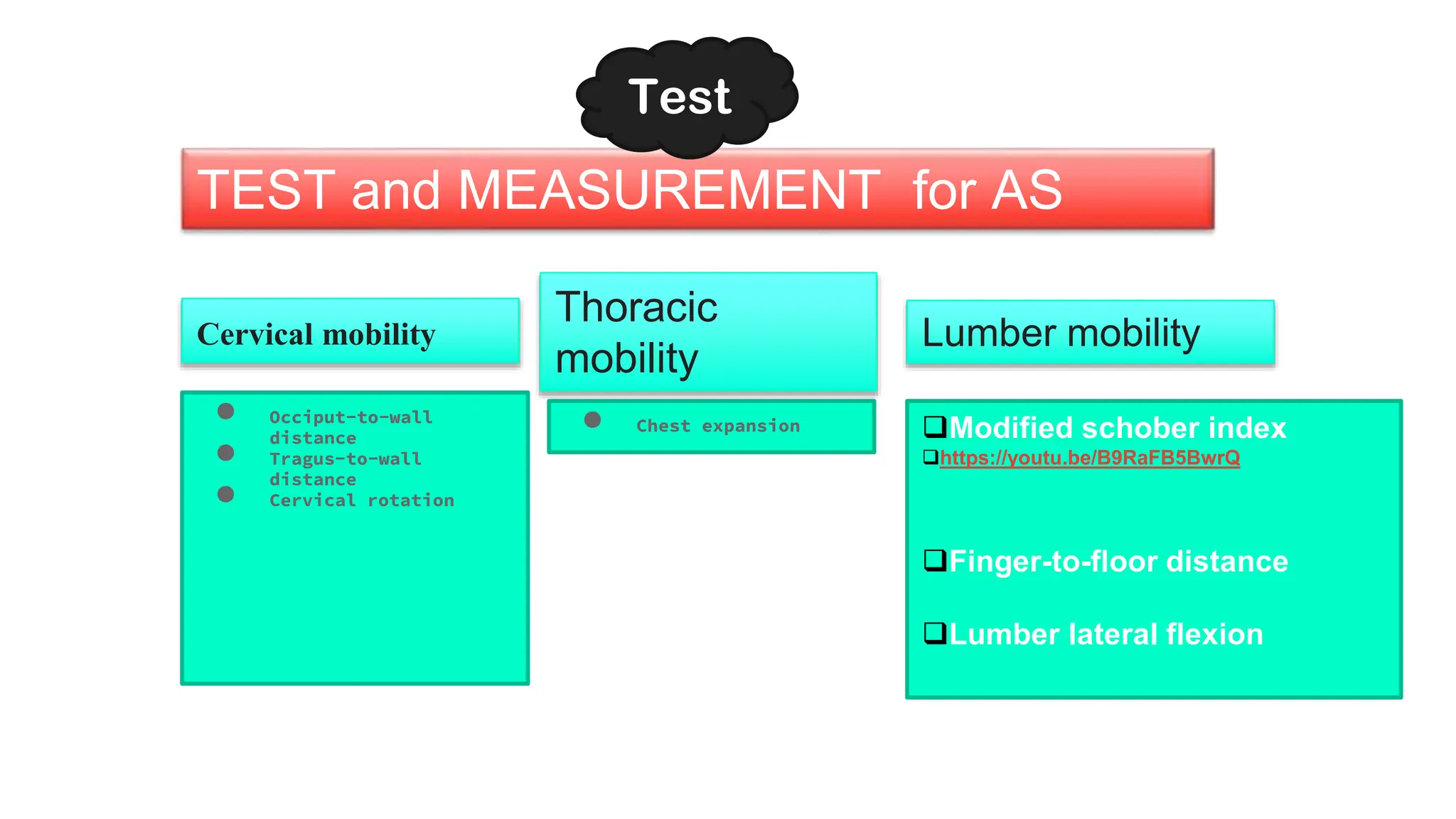
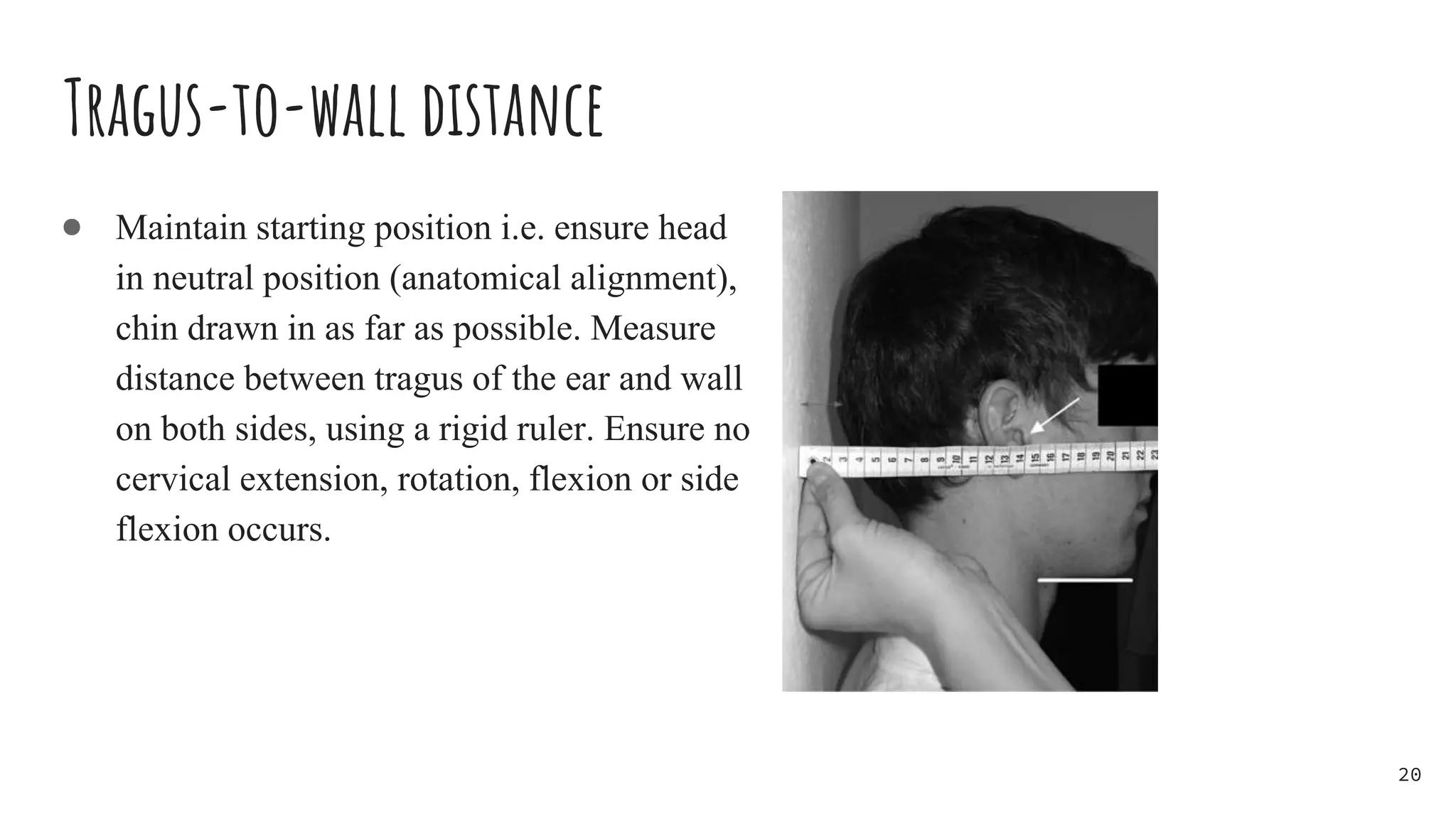
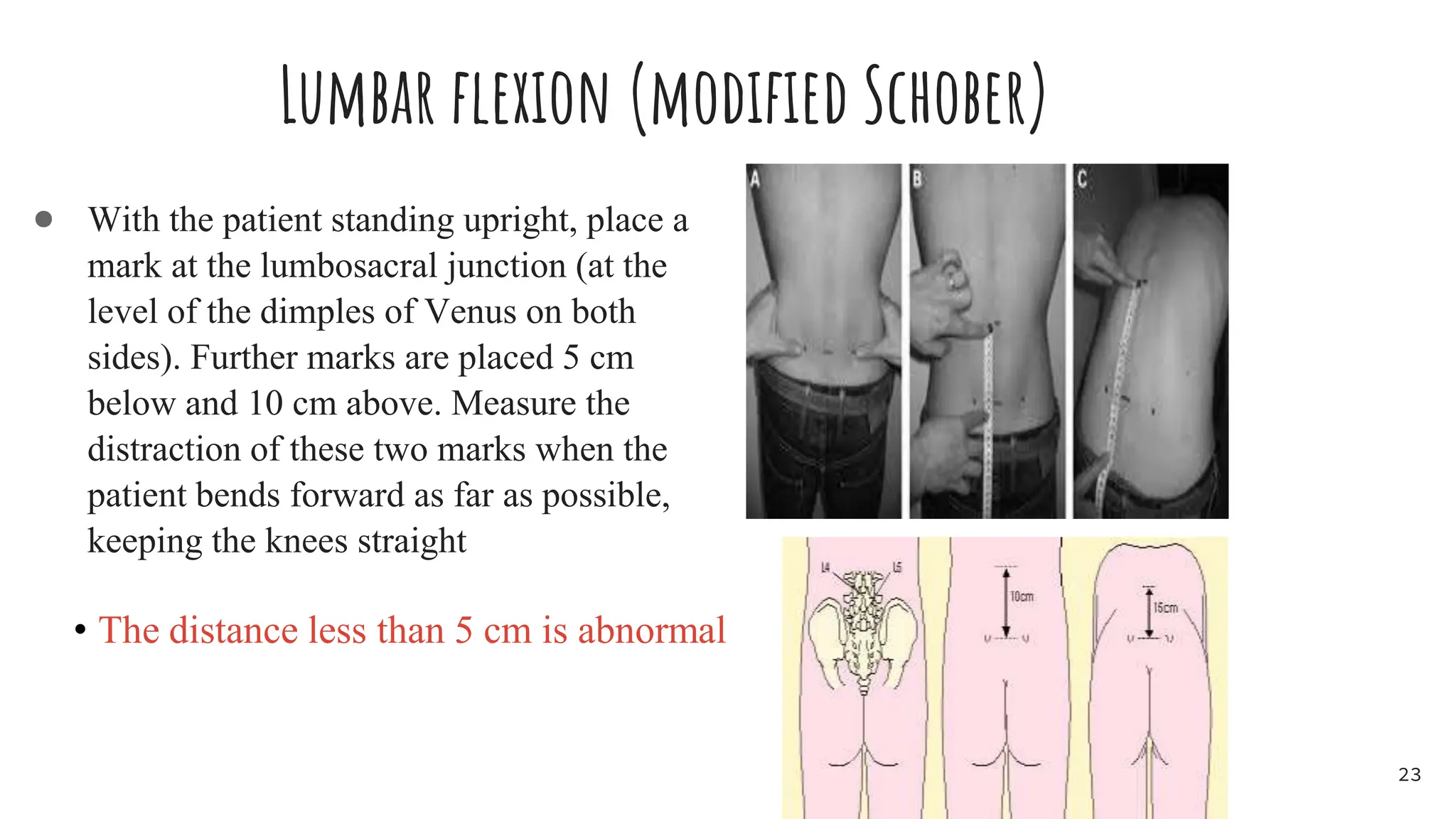
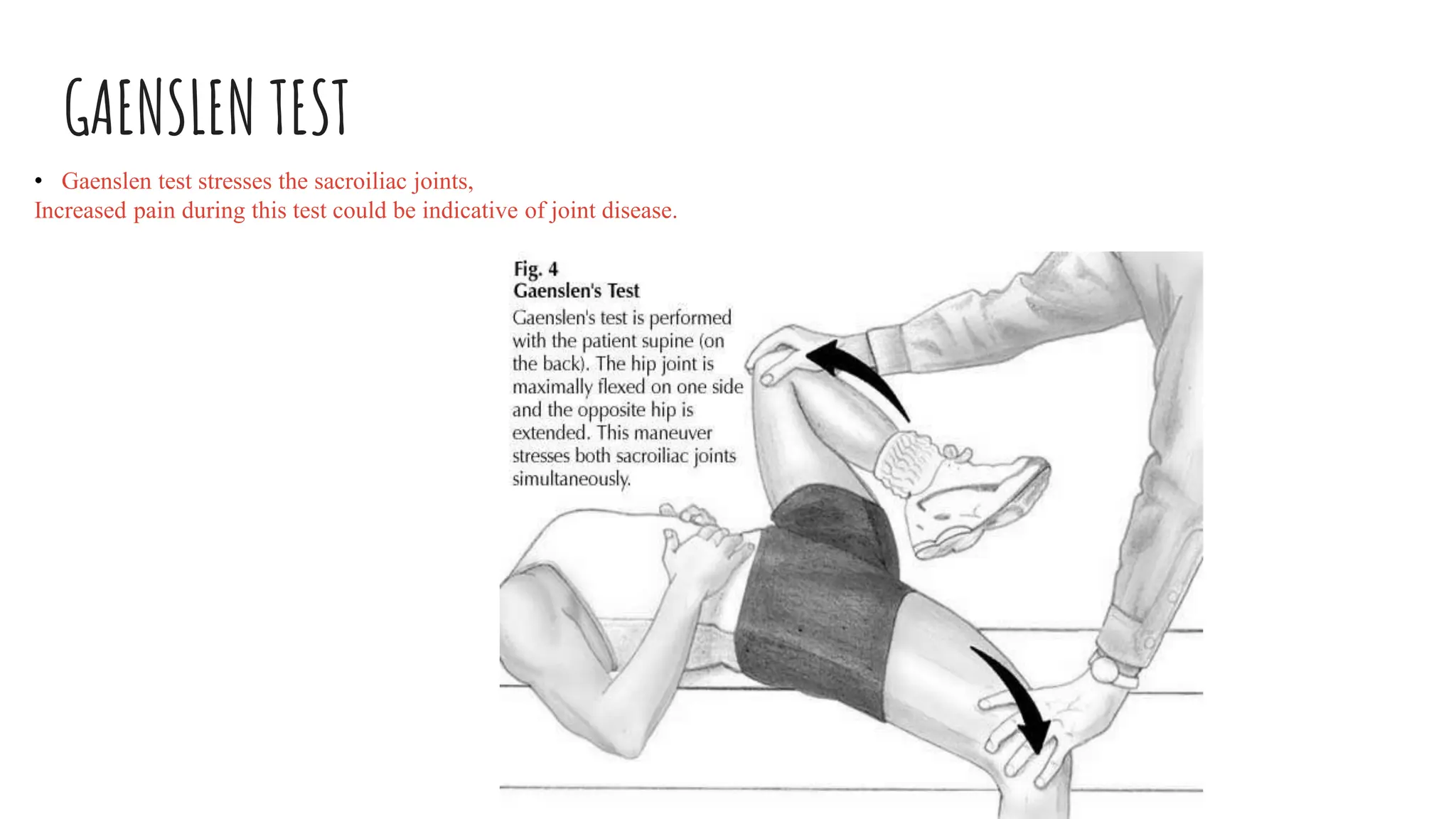
Ankylosing spondylitis (AS) is a chronic inflammatory disease primarily affecting the spine and pelvis, characterized by pain in the sacroiliac joints and the development of syndesmophytes leading to spinal fusion. AS has a complex etiology involving genetic (notably the HLA-B27 antigen) and environmental factors, with common symptoms including back pain, stiffness, and reduced mobility, notably impacting young males aged 20-40. Diagnosis includes a combination of family history, imaging criteria, and specific tests, with management focusing on pain reduction, improving mobility through physiotherapy, and exercise.